|
Erythroderma = الاحمرية الجلدية |
|
|
Erythroderma and Generalized Exfoliative Dermatitis
Erythroderma is characterized by generalized erythema and scale, often in association with fever. The eruption is nonspecific and may be caused by a variety of underlying conditions. In one study, 74.4% were associated with a preexisting dermatosis, 14.6% were idiopathic, and 5.5% were related to drugs and malignancy . Psoriasis is the most common preexisting dermatosis; others include spongiotic dermatitis, pityriasis rubra pilaris, photosensitivity syndromes, and, rarely, stasis dermatitis, dermatophytosis, pemphigus foliaceus, and even bullous pemphigoid. Many drugs have been incriminated, such as phenytoin, thiazides, nonsteroidal antiinflammatory drugs (NSAIDS), and recombinant cytokines. A small percentage of erythroderma is associated with lymphoma, most frequently cutaneous T cell lymphoma, in the form of Sezary syndrome or erythrodermic mycosis fungoides. The "red man syndrome" is erythroderma without knowing underlying causes. Some cases may progress to mycosis fungoides after many years.
|
|
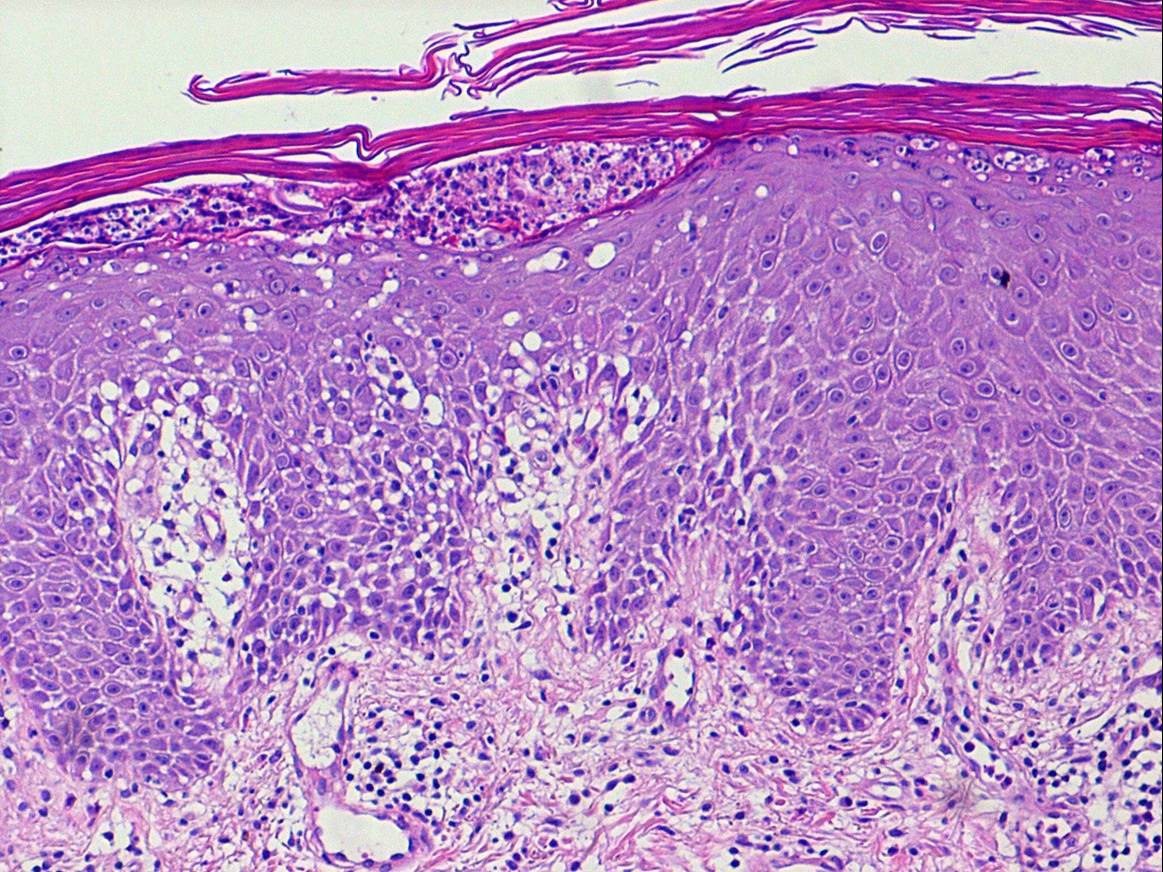
Histopathology.
A careful search for histologic features of any of the above listed etiologies must be undertaken; however, the nature of the underlying dermatosis is not always discernible in the erythrodermic phase, and the changes are often those of nonspecific subacute or chronic spongiotic dermatitis. Erythrodermic lesions associated with underlying psoriasis resemble early lesions of psoriasis with only mild epidermal hyperplasia, mild spongiosis, mounds of parakeratosis with a few neutrophils, and red cell extravasation in the papillary dermis. Blood vessels in the upper dermis are usually dilated. In cases of erythroderma related to mycosis fungoides, atypical cells with cerebriform nuclei are present in the infiltrate. Eosinophils may be present. Drug-related cases might simulate mycosis fungoides with exocytosis, lymphocytic atypia, and the presence of eosinophils. The presence of rare apoptotic keratinocytes may be a clue to the drug etiology.
|
The histopathologic findings are helpful in establishing the etiologic diagnosis in only about 40% of cases . Repeat biopsies and hematologic studies at regular intervals are recommended in patients without definitive diagnosis
|