
Furuncles and Carbuncles.
A furuncle or boil is a deep-seated inflammatory nodule that develops around a hair follicle, usually from a preceding, more superficial folliculitis and often evolving into an abscess. A carbuncle is a more extensive, deeper, communicating, infiltrated lesion that develops when suppuration occurs in thick inelastic skin when multiple, closely set furuncles coalesce.
FURUNCLES.
Furuncles arise in hair-bearing sites, particularly in regions subject to friction, occlusion, and perspiration, such as the neck, face, axillae, and buttocks. They may complicate pre-existing lesions such as atopic dermatitis, excoriations, abrasions, scabies, or pediculosis, but occur more often in the absence of any local predisposing causes. In addition, a variety of systemic host factors is associated with furunculosis: obesity, blood dyscrasias, defects in neutrophil function (defects in chemotaxis associated with eczema and high levels of IgE, defects in intracellular killing of organisms as in
chronic granulomatous disease of childhood), treatment with glucocorticoids and cytotoxic agents, and immunoglobulin deficiency states. The process is often more extensive in patients with diabetes. The majority of patients with problems of furunculosis appear to be otherwise healthy.
Cutaneous Lesions.
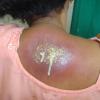
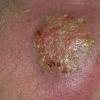
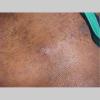
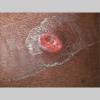
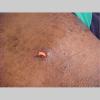
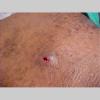
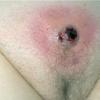
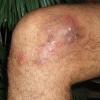
A furuncle starts as a hard, tender, red folliculocentric nodule in hair-bearing skin that enlarges and becomes painful and fluctuant after several days . Rupture occurs, with discharge of pus and often a core of necrotic material. The pain surrounding the lesion then subsides, and the redness and edema diminish over several days to several weeks. Furuncles may occur as solitary lesions or as multiple lesions in sites such as the buttocks .
CARBUNCLES.
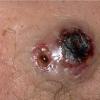
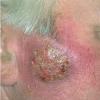
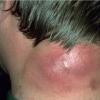
A carbuncle is a larger, more serious inflammatory lesion with a deeper base, characteristically occurring as an extremely painful lesion at the nape of the neck, the back, or thighs . Fever and malaise are often present, and the patient may appear quite ill. The involved area is red and indurated, and multiple pustules soon appear on the surface, draining externally around multiple hair follicles. The lesion soon develops a yellow-gray irregular crater at the center, which may then heal slowly by granulating, although the area may remain deeply violaceous for a prolonged period. The resulting permanent scar is often dense and readily evident.
LABORATORY TESTS.
Extensive furunculosis or a carbuncle may be associated with leukocytosis. S. aureus is almost always the cause. Histologic examination of a furuncle shows a dense polymorphonuclear inflammatory process in the dermis and subcutaneous fat. In carbuncles, multiple abscesses, separated by connective-tissue trabeculae, infiltrate the dermis and pass along the edges of the hair follicles, reaching the surface through openings in the undermined epidermis. The diagnosis is made on the basis of the clinical appearance. Gram stain of pus, clusters of Gram-positive cocci, or isolation of S. aureus on culture confirms the diagnosis.
PROGNOSIS AND CLINICAL COURSE.
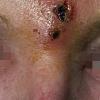
The major problems with furunculosis and carbuncles are bacteremic spread of infection and recurrence. Lesions about
the lips and nose raise the specter of spread via the facial and angular emissary veins to the cavernous sinus. Invasion of the bloodstream may occur from furuncles or carbuncles at any time, in an unpredictable fashion, resulting in metastatic infection such as osteomyelitis, acute endocarditis, or brain abscess. Manipulation of such lesions is particularly dangerous and may facilitate spread of infection via the bloodstream. Fortunately, these complications are not common. Recurrent furunculosis is a troublesome process that may continue for many years.
Differential Diagnosis of Furunculosis
- · Cystic acne
- · Kerion
- · Hidradenitis suppurativa
- · Ruptured epidermal inclusion cyst
- · Furuncular myiasis
- · Apical dental abscess
- · Osteomyelitis
TREATMENT.
Simple furunculosis may be aided by local application of moist heat. A carbuncle or a furuncle with surrounding cellulitis, or one with associated fever, should be treated with a systemic antibiotic . For severe infections or infections in a dangerous area, maximal antibiotic dosage should be employed by the parenteral route. If MRSA is implicated or suspected in serious infections, vancomycin (1.0 to 2.0 g intravenously daily in divided doses) is indicated. Antibiotic treatment should be continued for at least 1 week.
When the lesions are large, painful, and fluctuant, then incision and drainage is critical. If the infection is recurrent or complicated by co-morbidities, a culture can be sent. Antimicrobial therapy should be continued until all evidence of inflammation has regressed and altered appropriately as culture results become available. Draining lesions should be covered to prevent autoinoculation and diligent hand washing performed. Patients with recurrent furunculosis present a special and frequently exasperating problem .