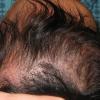
Blackdot tinea
Tinea capitis is a dermatophytic infection that is common in the pediatric population. During epidemics, it may affect 10% to 20% of susceptible children. Infection, which is less common in the postpubertal population, spreads easily from person to person. Fomites, such as combs, brushes, hats, pillows, blankets, and even the fabric on theater seats, act as common agents for transmission.
Trichophyton tonsurans is the most common cause of tinea capitis in the United States. It can be seen on hair stubs and has been known to remain alive for up to 2 years in the proper environment (1). Breakage of hairs at the roots causes the appearance referred to as black-dot tinea capitis. Evidence suggests the existence of a carrier state without clinical manifestations. In one study of 200 children without clinical evidence of tinea capitis (2), 4% had cultures positive for T tonsurans.
T tonsurans belongs to the endothrix group of infections, one of three groups of dermatophytes that cause tinea capitis (endothrix fungus, ectothrix fungus, and favus). In the past, when fluorescent ectothrix fungus predominated, examination with a Wood's lamp was used to screen for tinea capitis. However, T tonsurans does not fluoresce when examined with a Wood's lamp. The favus group of dermatophytes is rare in the United States but is often found in the Middle East and North Africa (3).
Infection with T tonsurans often begins in the perifollicular stratum corneum. After a period of incubation, hyphae spread into and around the hair shafts. Arthroconidia in the shafts cause the hairs to become brittle. The hairs break at the surface of the scalp, where they lose the support of the follicular wall (4). The broken hairs that remain below the surface of the scalp give the appearance of black dots in the area of hair loss. (Of course, "blond-dot" tinea capitis occurs in persons with blond hair.)
The patient in the case described here had pruritic, noninflammatory lesions and slowly advancing, scaly patches with broken hairs resembling black dots. Some patients also have inflammatory lesions, such as pustules, abscesses, and kerions. Kerions are discrete, purulent, boggy, tender masses that are often related to cervical lymphadenopathy. Inflammatory tinea is often caused by zoophilic or geophilic organisms.
Scalp conditions that resemble tinea capitis include seborrheic dermatitis (characterized by yellow, greasy scales), atopic dermatitis (widespread eczematous rash), psoriasis (white or silver scales on a purple-red base), alopecia areata (no scales), and trichotillomania (hairs of different lengths). The diagnosis of tinea capitis is best confirmed by microscopic examination of a potassium hydroxide preparation of scalp scrapings and broken hairs that demonstrates chains of arthrospores inside hair shafts (5). Fungal culture of several broken hairs and scales from the affected area is another method. At least one of these tests should be done to rule out tinea capitis in any child with pruritus and scaling of the scalp--even in the absence of hair loss and broken hairs resembling black dots.
A systemic approach to treatment is required. The drugs of choice are griseofulvin ultramicrosize (Fulvicin P/G, Grisactin Ultra, Gris-PEG) and liquid griseofulvin microsize (Grifulvin V). Treatment with ketonconazole 2% shampoo and topical antifungal creams can decrease scaling, but prompt recurrence is common because these products do not reach deeply enough into the hair follicle to eradicate the fungus. Because the infection can be easily spread to others, family members of patients with tinea capitis should be examined and treated if diagnostic tests are positive.
Treatment can fail when drug dosages are suboptimal. In our experience, the doses recommended in the Physicians' Desk Reference are too low. We recommend griseofulvin ultramicrosize, 10 to 15 mg/kg daily, crushed and taken with chocolate chip ice cream (dairy enhances absorption) for 6 to 8 weeks, or griseofulvin microsize, 20 mg/kg daily, taken with milk for 6 to 8 weeks (4). Ketoconazole 2% shampoo can be used as an adjunctive treatment to decrease the spread of tinea to others.