|
                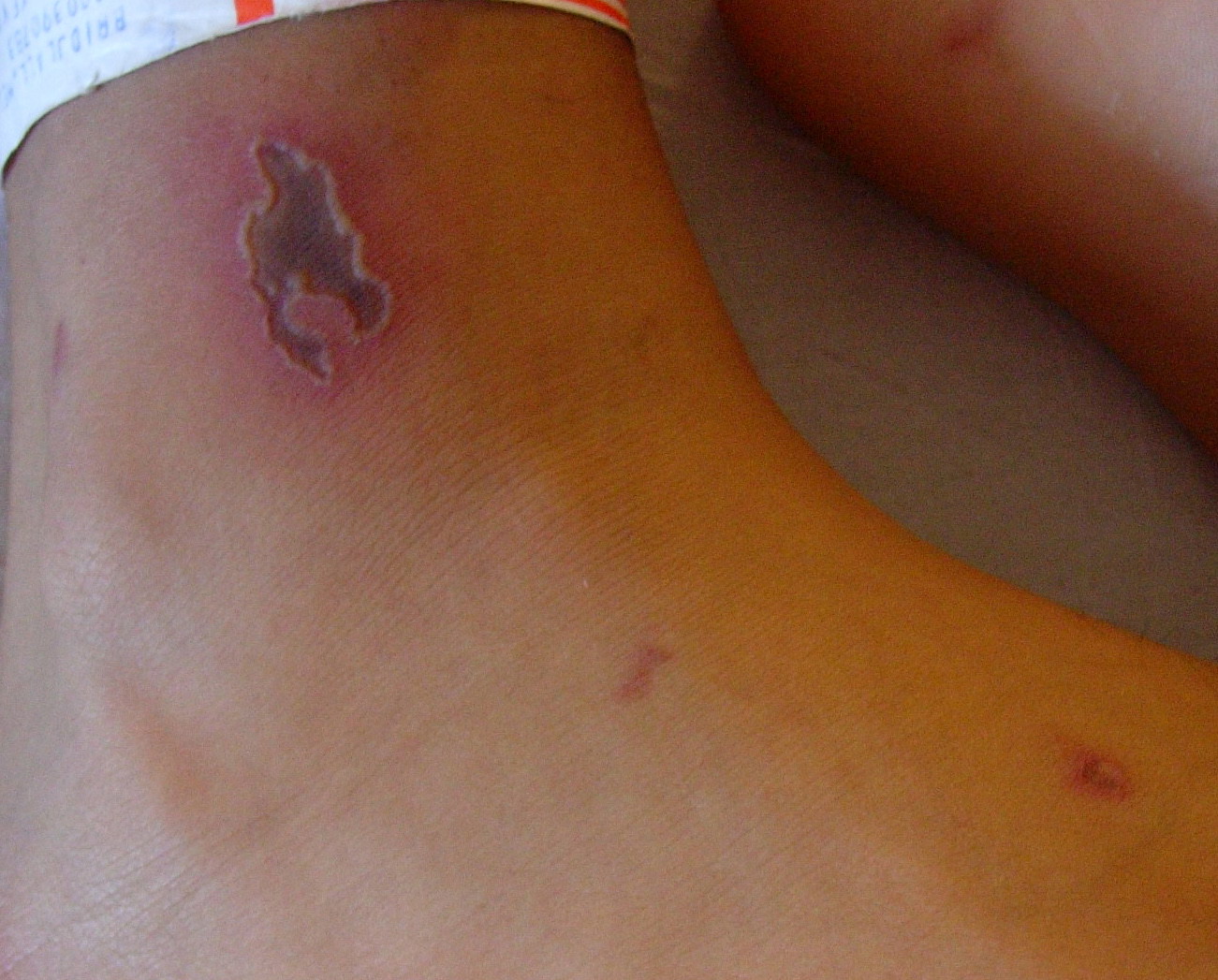 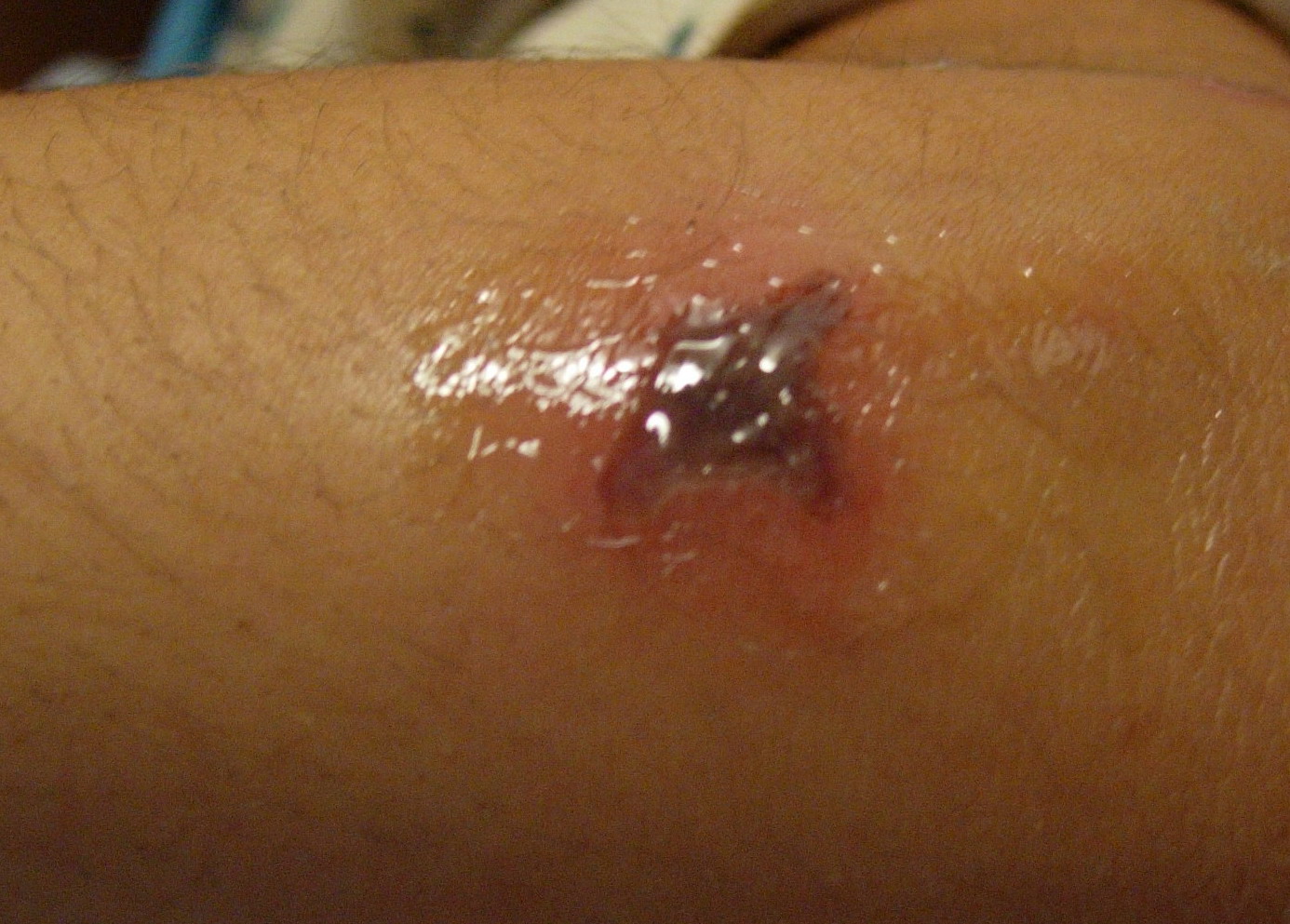
Meningococcemia – Acute- and
Meningitis
CLINICAL MANIFESTATIONS
History.
The disease often follows a mild upper respiratory tract infection associated with headache, grippe-like complaints, nausea, and muscle soreness. These symptoms can be so short-lived that fever, obtundation, and other manifestations of meningitis are the initial findings. In fulminant meningococcemia, vomiting, stupor, precipitous development of a hemorrhagic rash, and hypotension may be evident within a few hours of the onset of symptoms. Milder cases develop at a slower pace.
Cutaneous Lesions.
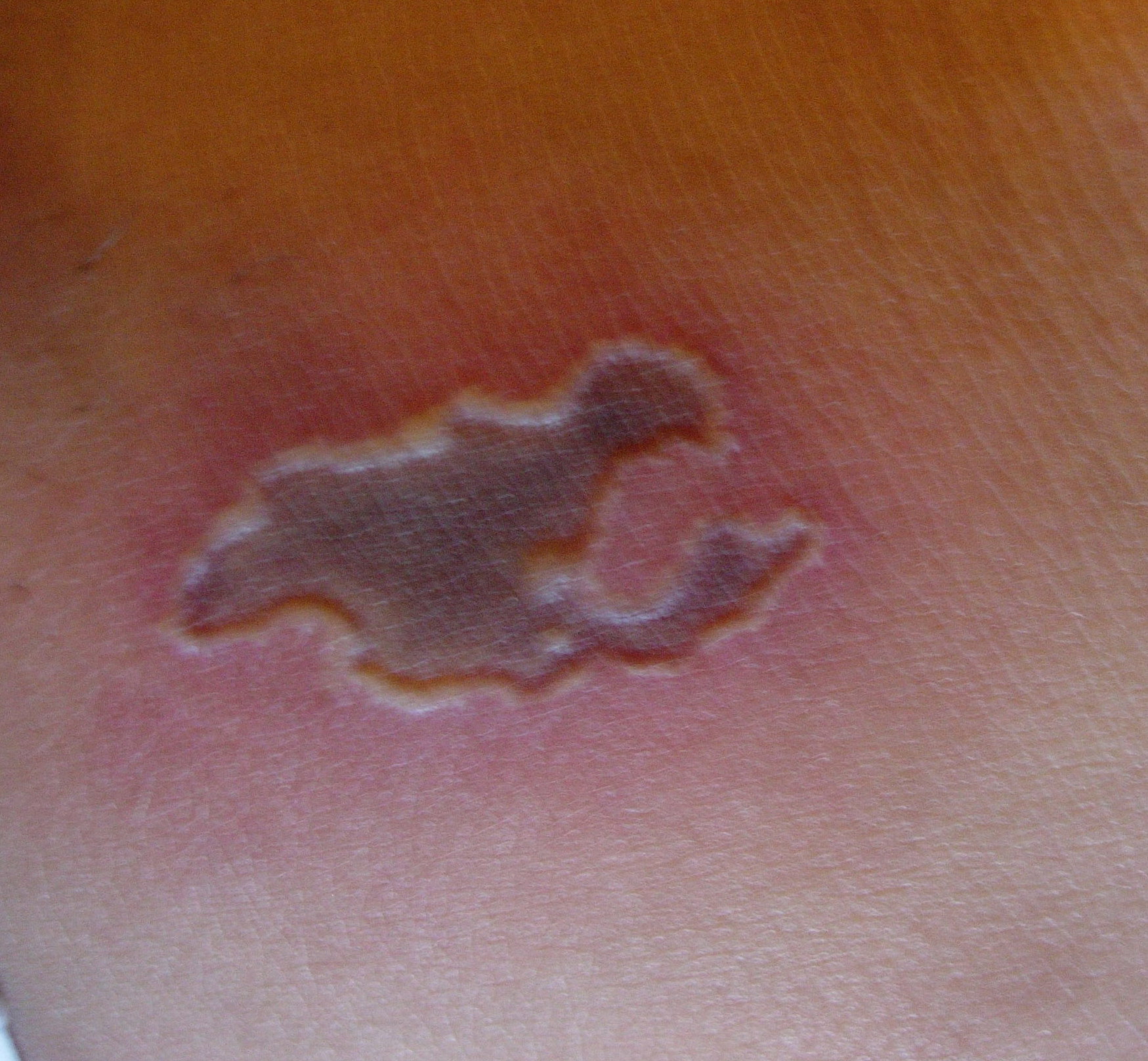
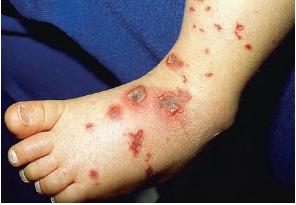
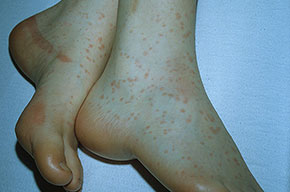
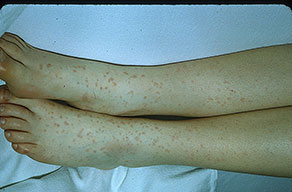
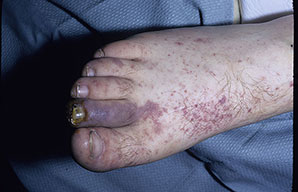
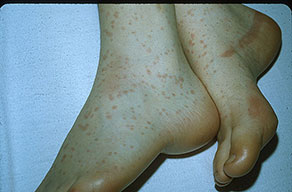
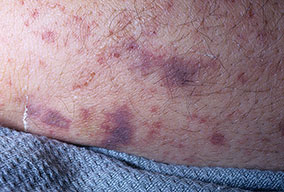
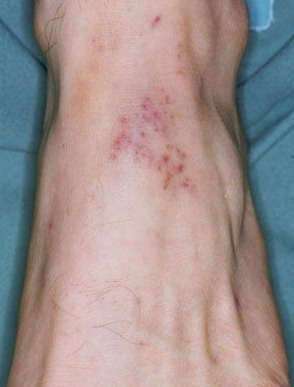
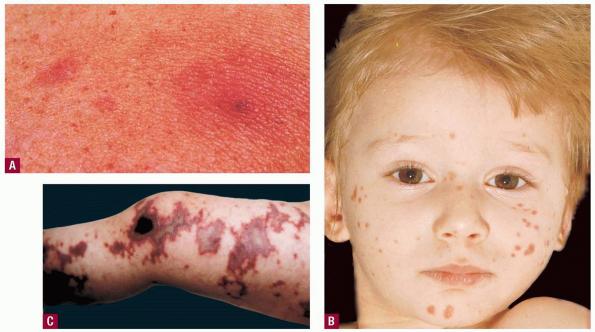
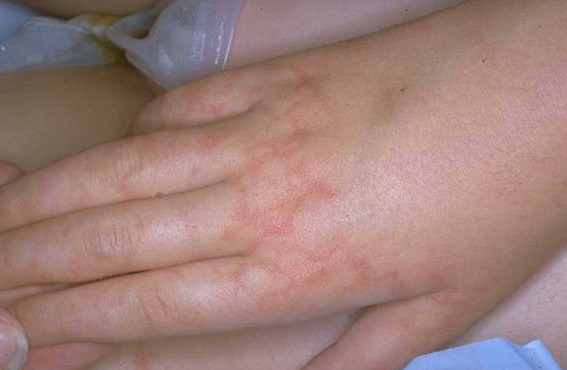
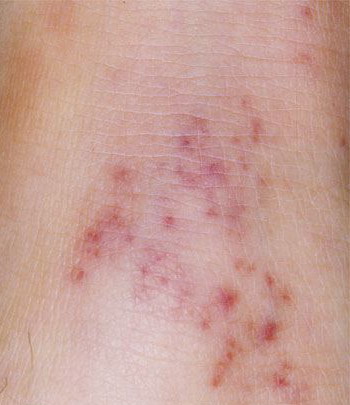
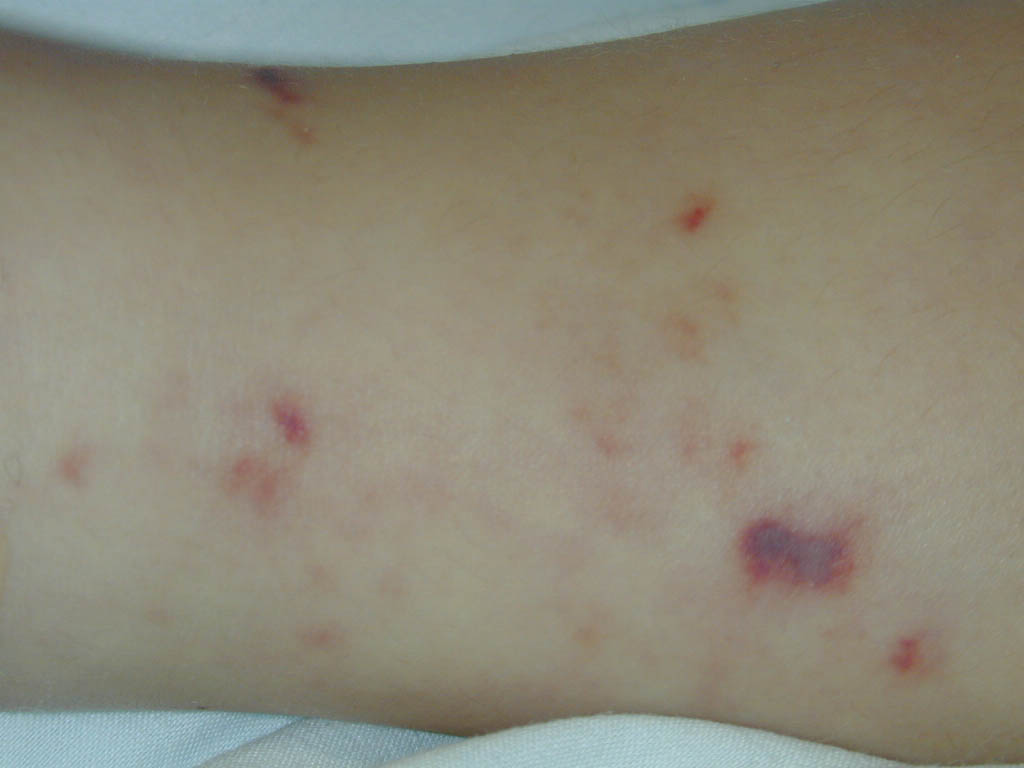
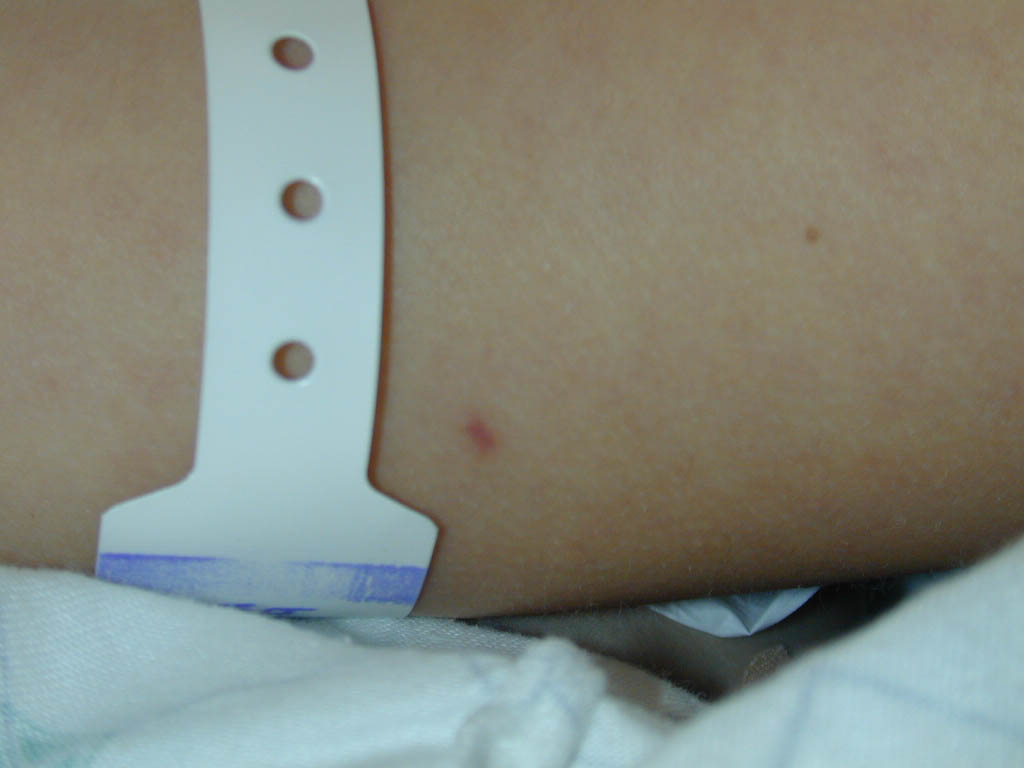
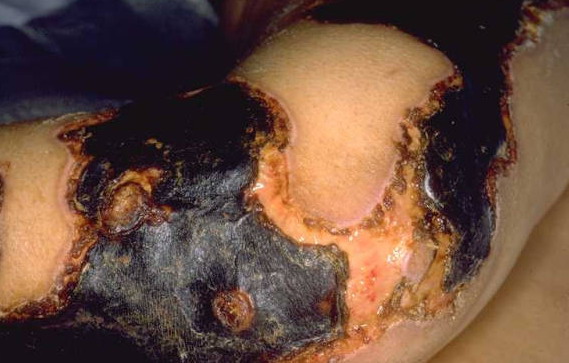
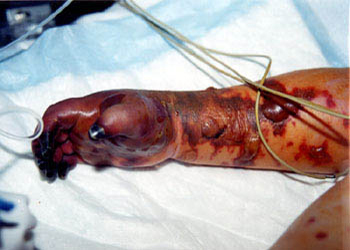
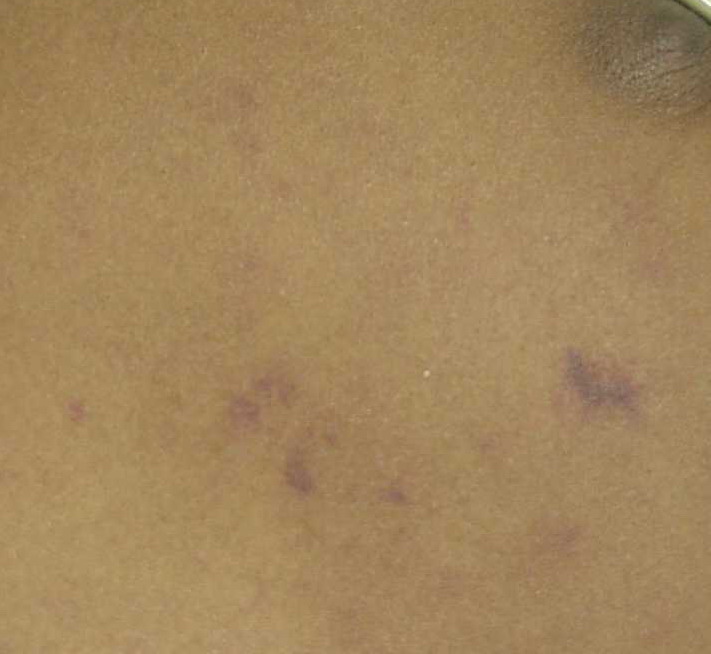
Skin findings in acute meningococcal infections are characteristically petechial, but transient macular or papular lesions , which can resemble those seen in viral exanthems, may be evident. The petechiae are small and irregular with a “smudged” appearance. Although most often located on the extremities and trunk, lesions can also be found on the head , palms, soles, and mucous membranes. Extensive hemorrhagic lesions with central necrosis (suggillations) and bullae can develop. Gangrenous hemorrhagic areas (indistinguishable from purpura fulminans; see Chap. 145) can appear in severe meningococcemia, often with DIC . Skin lesions and bacteremia are rarely seen with meningococcal pneumonia. Cellulitis has been noted occasionally, especially in children with meningococcal conjunctivitis (see Primary Meningococcal Conjunctivitis).
Other Physical Findings.
Patients with meningitis display signs of meningeal irritation and altered consciousness. Cranial nerve palsies, long-tract signs, seizures, and alterations in vital signs associated with changes in intracranial pressure may be present.
Obtundation and hypotension without meningeal signs, associated with the syndrome of DIC, are characteristic features of fulminant meningococcemia. Rarely, meningococcemia may result in septic foci in other areas: (1) septic arthritis, (2) purulent pericarditis with enlarging cardiac silhouette and findings of tamponade, and (3) bacterial endocarditis.
More commonly, a delayed immune complex-mediated syndrome results in a sterile arthritis, pericarditis, or episcleritis.3 The acute arthritis-dermatitis syndrome, characterized by petechiae and nontraumatic arthritis, has traditionally been identified with disseminated N. gonorrhoeae infection . There has been a decline of gonococcal cases and an increase in cases of this syndrome caused by N. meningitidis.
LABORATORY FINDINGS
A polymorphonuclear leukocytosis is present in peripheral blood and cerebrospinal fluid (CSF) in meningitis. The CSF glucose value is commonly reduced. Characteristic organisms may be seen on Gram-stained smears of fluid, and meningococci are usually isolated from the CSF. N. meningitidis may be isolated from the blood of approximately one-third of patients with meningitis and from almost 100 percent of patients with acute meningococcemia. Demonstration of organisms in cutaneous lesions has been variable, and the presence of Gram-negative commensal organisms on the skin requires cautious interpretation. Reports describe positive results for 50 percent to 80 percent of aspirates, skin film samples, and punch biopsy specimens of petechial lesions.
In patients already exposed to antimicrobial agents, the development of rapid, accurate, and inexpensive procedures for detection of soluble antigens in the CSF has been a major advance. The latex agglutination method and enzyme-linked immunosorbent assay methods are sensitive and very specific, but their clinical usefulness in most situations has been questioned. Rapid diagnosis using polymerase chain reaction (PCR) testing is available in research settings.
HISTOPATHOLOGY
Endothelial swelling is seen, a perivascular infiltrate of polymorphonuclear leukocytes is present, thrombi occlude capillaries and postcapillary venules, and the walls of capillaries and venules are destroyed, as in leukocytoclastic vasculitis .
DIFFERENTIAL DIAGNOSIS
Meningococcal infection warrants consideration in a patient with fever and a petechial or purpuric eruption, even in the absence of clinical meningitis (Box 180-1). Occasionally, the characteristic rash is absent, which delays consideration of meningococcal disease.
COURSE AND PROGNOSIS
Untreated, acute meningococcal disease usually ends fatally. With treatment, recovery occurs in 90 percent of patients with meningitis.
In severe meningococcemia, especially with the rapid emergence of cutaneous hemorrhages, hypotension, and
DIC, the entire course from onset to death can be measured in hours. In patients with sepsis-associated DIC, cutaneous thrombotic hemorrhages on the distal extremities may lead to skin and digital necroses that necessitate amputation. Rarely, young children with meningococcal sepsis, shock, and DIC suffer thrombotic injury that causes growth plate arrest. Myocardial dysfunction often occurs in meningococcal septic shock and is associated with high circulating levels of interleukin 6. These cases are often associated with massive adrenal hemorrhage (Waterhouse-Friderichsen syndrome). Children who die from meningococcal septic shock have relatively low cortisol levels (but not in the range expected in adrenal insufficiency). The mortality rate for meningococcal septic shock approaches 100 percent. Gradations in the severity of meningococcal disease make it difficult to assign an accurate prognosis, although a bedside predictive model has been proposed.
Differential Diagnosis of Acute Meningococcemia
· Acute bacteremias and endocarditis: In endocarditis, mucous membrane and conjunctival lesions, as well as subungual “splinter” hemorrhages, occur. Very infrequently, numerous petechial and purpuric lesions occur in patients with acute Staphylococcus aureus endocarditis. Usually, a few skin lesions in a patient with acute S. aureus endocarditis are purulent purpura. In acute gonococcemia, the skin lesions are usually acral, nodular, hemorrhagic, and few in number . Occasional patients with Haemophilus influenzae or Streptococcus pneumoniae bacteremia develop petechial eruptions.
· Cutaneous necrotizing vasculitis : Here, lesions are usually palpable. Renal involvement and hypertension may be present.
· Enteroviral infections: Fever, petechial eruptions, and aseptic meningitis are frequent features.
· Rocky Mountain spotted fever: The history of exposure to ticks in an endemic area, absence of an antecedent respiratory infection, and delay in appearance of the rash are clues .
· Toxic shock syndrome .
· Purpura fulminans .
· Weil disease (leptospirosis) .
|