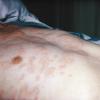


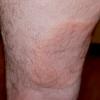

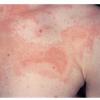
Acute urticaria
Urticaria was first described in the English literature in 1772, although the disease has been recognized throughout history. Urticaria is marked by the onset of evanescent wheals (hives) associated with pruritus. Acute urticaria is a common disorder that often prompts patients to seek treatment in the emergency department (ED). In fact, acute urticaria is the most common cutaneous disease treated in the ED.1 The eruption is symptomatic and can be visually apparent over many different parts of the skin. The natural course acute urticaria lasts from a one-time event of several hours' duration up to 6 weeks, depending on the etiology. If urticaria is present continuously over a 6-week period, it is categorized as chronic urticaria.
Individual lesions of acute urticaria can appear at different locations and fade without scarring, often in a matter of hours. In 50% of patients with acute urticaria, a specific etiology can be identified. Brief episodes of urticaria can be associated with identifiable causes, and the method of exposure (ie, direct contact, oral or intravenous routes) is usually known. If the location of the wheals remains fixed for longer than 24 hours, the diagnosis may be urticarial vasculitis or bullous pemphigoid, and a skin biopsy is indicated for diagnosis.
Pathophysiology
The release of histamine and other compounds by mast cells and basophils causes the appearance of urticaria. Immune-mediated urticaria is from immunoglobulin E (IgE) binding specific antigen, and the IgE-complex binding to FcER1 receptors to activate mast cells. Mast cell activation from crosslinking of FcER1 receptor causes degranulation of intracellular vesicles that contain histamine, leukotriene C4, prostaglandin D2, and other chemotactic mediators that recruit eosinophils and neutrophils into the dermis.2,3 Histamine and chemokine release lead to extravasation of fluid into the dermis (edema). Histamine effects account for many of the clinical and histologic findings of urticaria.
Histamine is the ligand for at least 2 types of membrane-bound receptors, H1 and H2 receptors, which are present on numerous cells. The activation of H1 histamine receptors on smooth muscle cells and endothelial cells leads to cellular contraction and increased vascular permeability. The activation of H2 histamine receptors causes vasodilation. Urticaria is a reaction pattern that reflects the activation of mast cells and basophils. The exact mechanism of action resulting in the release of the intracellular contents of mast cells and basophils is varied and can occur through immune-mediated or non–immune-mediated mechanisms.
Immune-mediated urticaria
Immune-mediated urticaria can be caused by 3 of 4 types of immune mechanisms, as follows:
- The type I allergic IgE response is initiated by antigen-mediated IgE immune complexes that bind and cross-link Fc receptors on the surface of mast cells and basophils. The types of antigens that bind to IgE are varied and include proteins, polysaccharides, and other immunogenic molecules.
- Type II responses are mediated by cytotoxic T cells. The disease process activates byproducts that cause urticarial vasculitis or bullous pemphigoid.
- Type III immune-complex disease is associated with systemic lupus erythematosus and other connective tissue disorders that activate urticaria.
Non–immune-mediated urticaria
Chemicals that can directly induce mast cell degranulation, presumably by altering the membrane properties, cause non–immune-mediated urticaria. Common agents associated with direct mast cell activation are opiates, antibiotics, curare, radiocontrast media, azo dyes, aspirin, and aspirin derivatives
History
Acute urticaria is characterized by the onset of clinically apparent, edematous, evanescent, erythematous plaques. Individual acute urticaria lesions remain for less than 24 hours, exhibiting a transitory and migratory behavior. The etiology can be inferred in as many as 50% of new cases. In general, greater than 80% of new-onset urticaria resolves in 2 weeks and greater than 95% of new-onset cases resolve by 3 months. Atopy can often be identified in the patient or his or her family members. When urticaria persists for more than 6 weeks, it is considered chronic urticaria. Additional etiologies exist for chronic urticaria. A thorough medical evaluation is indicated to eliminate the possibility of treatable causes of urticaria, which include malignancies, connective tissue disorders, and chronic infections.
Acute urticaria is commonly caused by a variety of infections, medications, food allergies, physical stimulants, chemicals, chronic inflammatory diseases, and insect bites, as follows7,8 :
- Recent infection from a viral syndrome or an upper respiratory tract illness (39%)
- Medications (eg, ACE inhibitors, aspirin, nonsteroidal anti-inflammatory drugs, sulfa-based drugs, penicillins, diuretics, opioids, polymyxin B)
- Food and food additives (eg, nuts, fish, shellfish, eggs, chocolate, strawberries, salicylate, benzoates)
- Parasitic infections (eg, Ascaris, Ancylostoma, Strongyloides, Echinococcus, Trichinella, Filaria)
- Physical stimulants (eg, cold, pressure, aquagenic)
- Chemicals (eg, latex, ammonium persulfate in hair chemicals)
- Intravenous radiocontrast media
- Arthropod bites
New-onset fever and constitutional symptoms suggest chronic autoimmune disease.
Physical
Lesions of urticaria can be polymorphic and vary from several millimeters to large, continuous plaques. Plaques have smooth surfaces with polycyclic curved borders. Lesions do not have scales.
Lesions show an intense erythema in the newest areas, with a trailing clearing region in older areas. Central clearing can cause a target configuration in expanding plaques. The advancing border shows a discrete edge followed by a faint, trailing, diffuse border. Lesions last less than 24 hours, and scars do not develop
Erythema multiforme can resemble urticaria. Both processes can be a reaction to medication. Early lesions of erythema multiforme may appear edematous, round, targetoid, and polycyclic as the lesion expands. However, in erythema multiforme, each lesion can be differentiated by the stationary nature and the progression to a dusky color with bulla formation.
Causes
A definitive inciting agent can be identified in 40-50% of cases of acute urticaria. In one study, causes were identified as an upper respiratory tract infection in 39.5% of the total cases, analgesics in 9%, and food intolerance in 0.9%.9 Urticaria associated with the onset of autoimmune disorders or malignancy (eg, systemic lupus erythematosus, lymphoma) becomes chronic. Most cases of new-onset urticaria are idiopathic in nature
Laboratory Studies
No specific laboratory study is needed for acute urticaria unless the patient's history suggests a particular diagnostic test. A complete thorough medical and travel history is important to provide clues to a new presentation of infectious or medical problems. A thorough review of systems is essential.10
Obtain imaging studies if indicated by the patient's history.
Obtain other tests if indicated by the patient's history.
No procedures are necessary for the diagnosis of acute urticaria. If the lesion remains for longer than 24 hours or if it blisters, a skin biopsy is suggested to investigate for other possibilities in the differential diagnosis.
Histologic Findings
The histologic findings of acute urticaria are not dramatic. No epidermal change is present. Acute urticaria demonstrates intravascular margination of neutrophils. Later lesions demonstrate diapedesis of neutrophils through the vessel wall in the absence of karyorrhexis. Late lesions demonstrate intravascular, perivascular and interstitial neutrophils with little to no karyorrhexis. A moderate number of eosinophils may be present
Medical Care
Identify the etiology of the acute urticaria if possible. If an inciting agent can be identified, instruct the patient to avoid it. The major goal is to control the severity of acute urticaria lesions until the process resolves over 4-6 weeks.
The cause is not known in greater than 50% of acute urticaria cases. The most commonly identified cause is a recent infection or viral syndrome, and, under these circumstances, the patient should be informed of the self-limiting duration of the disorder.12
Palliation of pruritus and discomfort associated with the acute urticaria lesions is the primary goal of treatment in the initial visit. Therapy aims to block histamine action. Classes of drugs to consider are H1 antihistamines, H2 antihistamines, glucocorticoids, and tricyclic antidepressants that have combined H1 and H2 antagonists (eg, doxepin).
Selected clinical guideline summaries are as follows:
- British Association of Dermatologists - Guidelines for evaluation and management of urticaria in adults and children13
- American Academy of Allergy, Asthma & Immunology -Consultation and referral guidelines citing the evidence: how the allergist-immunologist can help14
- Joint Council of Allergy, Asthma and Immunology -The diagnosis and management of anaphylaxis: an updated practice parameter15
Surgical Care
Surgical care is not indicated in acute urticaria.
Consultations
Consult appropriate specialists as indicated by the patient's history and a thorough review of systems.
Diet
Educate patients to avoid food and food additives if identified as the cause of urticaria. Review medications to screen for the use of aspirin, salicylates, and nonsteroidal anti-inflammatory drugs. If identified, these nonimmunologic histamine releasers should be discontinued.
Medication
With the development of numerous classes of drugs that affect the immune system, there are now many choices for the treatment of urticaria.16 The drug of choice for control of urticaria initially is an H1 antihistamine. Numerous choices are available from this group, each with a different adverse effect profile. The choice is based on the patient's needs and tolerability to a particular antihistamine. With the number of nonsedating antihistamines available today, these agents should be tried first to facilitate disappearance of the lesions and symptoms of pruritus.
To achieve optimal control of urticaria, try different agents or increase the dose to maximum tolerable levels for that agent. In difficult cases, a combination of H1 and H2 antihistamines may be more effective. Doxepin has both H1 antihistaminic properties and H2 antihistaminic properties and can be used when a single H1 agent fails to control disease activity. Additionally, leukotriene inhibitors can be added to antihistamines for recalcitrant cases of urticaria.17 Finally, severe or refractory urticaria may benefit from a tapering course of prednisone in combination with an antihistamine.18
Antihistamines
Newer nonsedating antihistamines may be tried initially to control urticaria. Agents include fexofenadine, loratadine, desloratadine, and cetirizine.19,20 If additional antihistamines are needed, traditional agents can be considered. The 6 traditional classes of antihistamines are alkylamine, ethylenediamine, ethanolamine, propylamine, phenothiazine, and piperazine. Each has different adverse effects that may vary among individuals. Nonsedating H1 antihistamines with similar effectiveness in the treatment of urticaria are available. The choices for treatment are broad, and therapeutic options are tailored to the patient. The examples of drugs below do not represent the preferred agents or the specific recommendation of the author. Other antihistamines should also be considered and reviewed before treatment.
Diphenhydramine (Benadryl, Benylin, Diphen, AllerMax)
For symptomatic relief of symptoms caused by release of histamine in allergic reactions. Ethanolamine antihistamine that is commonly prescribed. Can be purchased over-the-counter, but prescription doses are often necessary. Sedation is an associated effect.
Adult
25-50 mg PO q6-8h prn; not to exceed 400 mg/d
Pediatric
5 mg/kg PO qd in divided doses; not to exceed 300 mg/d
Potentiates effect of CNS depressants; because of alcohol content, do not give liquid dosage form to patient taking medications that can cause disulfiramlike reactions
Documented hypersensitivity; MAOIs
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Can exacerbate conditions associated with increased cholinergic tone (eg, angle-closure glaucoma; urinary retention; dryness of the mouth, nose, and throat); other effects include vertigo, visual disturbance, tremors, and impotence; may exacerbate hyperthyroidism and peptic ulcer; has been associated with QT prolongation at toxic doses
Hydroxyzine (Atarax, Vistaril)
Antagonizes H1 receptors in periphery. May suppress histamine activity in subcortical region of CNS. Piperazine type of antihistamine that is effective and has fewer sedating effects compared with diphenhydramine. Usually well tolerated in most individuals.
Adult
25-100 mg PO qd/qid
Pediatric
2 mg/kg/d PO; 0.6 mg/kg/dose PO q6h
CNS depression may increase with alcohol or other CNS depressants
Documented hypersensitivity
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Associated with clinical exacerbations of porphyria (may not be safe for patients with porphyria); ECG abnormalities (alterations in T waves) may occur; may cause drowsiness
Loratadine (Claritin)
Nonsedating antihistamine that has long-acting characteristics. Selectively inhibits peripheral histamine H1 receptors. Available as 10-mg tab, 10-mg RediTab, and syr at 5 mg/5 mL (tsp).
Adult
10 mg PO qd; qod in patients with renal or hepatic impairment
Pediatric
<2 years: Not established
2-6 years: 5 mg/d
>6 years: Administer as in adults
Ketoconazole, erythromycin, procarbazine, and alcohol may increase loratadine levels
Documented hypersensitivity
Pregnancy
B - Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
Initiate therapy at lower dose or administer qod in liver impairment
Cetirizine (Zyrtec)
Second-generation antihistamine with markedly reduced sedative effects and reduced anticholinergic effects. Forms complex with histamine for H1 receptor sites in blood vessels, GI tract, and respiratory tract. Available as 5- and 10-mg tab, 5- and 10-mg chewable tab, and syr at 1 mg/mL or 5 mg/5 mL (tsp).
Adult
5-10 mg PO qd; reduce to 5 mg qd in patients with renal and hepatic impairment; in geriatric patients (77 y or older), 5 mg qd recommended
Pediatric
6 months to <2 years: 2.5 mg (half tsp) syr qd; in those 12-23 mo, can increase to maximum of 5 mg/d, given as half tsp (2.5 mg) q12h
2-5 years: 2.5 mg PO qd (half tsp); can increase to 5 mg/d and administer as qd or bid dose; do not use in renal or hepatic impairment
>5 years: 5-10 mg PO qd depending on severity (half dose with renal impairment)
Increases CNS toxicity of depressants
Documented hypersensitivity
Pregnancy
B - Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
Caution in hepatic or renal dysfunction; doses >10 mg/d may cause drowsiness; sedation less frequent than with traditional H1 blockers (was 13.7% in adult studies and 1.2-4.9% in pediatric studies); anticholinergic adverse effects may occur (eg, dry mouth, urinary retention, orthostatic hypotension); excreted in breast milk; headache most frequent pediatric adverse effect (11-14%)
Desloratadine (Clarinex)
Long-acting tricyclic histamine antagonist selective for H1 receptor. Relieves nasal congestion and systemic effects of seasonal allergy. Is a major metabolite of loratadine, which, after ingestion, is metabolized extensively to active metabolite 3-hydroxydesloratadine. Available as 5-mg tab, syr at 0.5 mg/mL (2.5 mg/5 mL), and 2.5- and 5-mg RediTab (desloratadine orally disintegrating tab).
Adult
5 mg PO qd
Pediatric
6-11 months: 2 mL (1 mg) syr qd
12 months to 5 years: 1.25 mg/2.5 mL syr (half tsp) qd
6-11 years: 1 tsp syr qd or one 2.5-mg RediTab qd
>12 years: Administer as in adults
Limited data exist; erythromycin and ketoconazole increase desloratadine and 3-hydroxydesloratadine plasma concentrations, but no increase in clinically relevant adverse effects, including QTc, is observed
Documented hypersensitivity
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Decrease dose in hepatic impairment; rarely causes pharyngitis or dry mouth; passes into breast milk
Fexofenadine (Allegra)
Competes with histamine for H1 receptors on GI tract, blood vessels, and respiratory tract, reducing hypersensitivity reactions. Does not sedate. Available as 30-, 60-, or 180-mg tab. Allegra ODT tab formulated for disintegration in mouth immediately following administration. Each orally disintegrating tab contains 30 mg fexofenadine hydrochloride. Oral susp contains 6 mg fexofenadine hydrochloride per mL or 30 mg/5 mL.
Adult
60 mg bid or 180 mg qd with water (sustained release); 60 mg qd recommended as starting dose in patients with decreased renal function
Pediatric
6 months to <2 years: Oral susp 15 mg (2.5 mL) bid
2-11 years: Oral susp 30 mg (5 mL) bid
6-11 years: 30 mg bid with water; Allegra ODT intended for use only in children 6-11 y
12 years or older: Administer as in adults
Studies indicate that ketoconazole or erythromycin coadministration enhances fexofenadine GI absorption; observed increase in bioavailability of fexofenadine may be due to transport-related effects
Documented hypersensitivity
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Fruit juices (eg, grapefruit, orange, apple) may reduce bioavailability and exposure of fexofenadine; should not be taken closely in time with aluminum- and magnesium-containing antacids
Corticosteroids
Prednisone taper can be effective when combined with an antihistamine.
Prednisone (Deltasone, Orasone, Sterapred)
Useful in cases that have not responded to traditional antihistamine. For extensive symptomatic urticaria, a burst of prednisone over 4 d can lead to marked improvement and control of symptoms.
Adult
40 mg PO qd burst over 4 d in combination with antihistamine; when used alone, taper over 2 wk
Pediatric
1-2 mg/kg/d PO taper over 2 wk
Ketoconazole, erythromycin, clarithromycin, estrogens, and birth control pills increase levels; aminoglutethimide, phenytoin, and phenobarbital decrease levels
Levels of potassium-depleting diuretics (potentiates potassium loss and digitalis toxicity) and cyclosporine may increase; levels of isoniazid, insulin (resistance is induced), and salicylates may decrease
Monitor anticoagulant therapy and theophylline levels
Absolute: Systemic fungal infection; herpes simplex keratitis; hypersensitivity (usually with corticotropin, occasionally noted with IV preparations)
Relative: Hypertension, active tuberculosis, congestive heart failure, prior psychosis, positive IPPD result, glaucoma, severe depression, diabetes, active peptic ulcer disease, cataracts, osteoporosis, recent bowel anastomosis, pregnancy
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Abrupt discontinuation of glucocorticoids may cause adrenal crisis; hyperglycemia, edema, osteonecrosis, myopathy, peptic ulcer disease, hypokalemia, osteoporosis, euphoria, psychosis, myasthenia gravis, growth suppression, and infections may occur with glucocorticoid use; use lower dose in hypothyroidism, liver disease, and obesity (cortisol-binding globulin level is decreased, which increases free fraction of steroid); pregnancy, hyperthyroidism, and concurrent estrogen therapy may increase cortisol-binding globulin level
Tricyclic antidepressants
Doxepin has been used in urticaria and pruritus.
Doxepin (Sinequan, Zonalon)
Inhibits histamine and acetylcholine activity. Has both H1 antagonist activity and H2 antagonist activity that is far more potent than traditional antihistamines. Has antidepressant properties attributed to blocking MAO.
Adult
10-25 mg PO tid
Pediatric
<12 years: Not recommended
>12 years: 25-50 mg/d PO hs or bid/tid and increase gradually to 100 mg/d
Decreases antihypertensive effects of clonidine but increases effects of sympathomimetics and benzodiazepines; effects of desipramine increase with phenytoin, carbamazepine, and barbiturates
Documented hypersensitivity; urinary retention; acute recovery phase following MI; glaucoma
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Caution in cardiovascular disease, conduction disturbances, seizure disorders, urinary retention, and hyperthyroidism; caution in patients receiving thyroid replacement; may cause prolonged sedation, particularly in elderly patients (use lower dose)
Histamine H2 antagonists
Used for treatment of duodenal ulcer disease; however, can be used in combination with H1 antihistamines when H1 antihistamines alone do not provide adequate relief.
Cimetidine (Tagamet)
H2 antagonist that when combined with an H1 antagonist may be useful in treating itching and flushing in urticaria and contact dermatitis that do not respond to H1 antagonists alone. Use in addition to H1 antihistamines.
Adult
300 mg PO qid; not to exceed 2400 mg/d
Pediatric
<12 years: Not established
>12 years: 20-40 mg/kg/d PO
Can increase blood levels of theophylline, warfarin, TCAs, triamterene, phenytoin, quinidine, propranolol, metronidazole, procainamide, and lidocaine
Documented hypersensitivity
Pregnancy
B - Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
Altered gastric acidity can affect absorption of cyclosporine and ketoconazole; elderly persons may experience confusional states; may cause impotence and gynecomastia in young males; may increase levels of many drugs; adjust dose or discontinue treatment if changes in renal function occur
Leukotriene Receptor Antagonist
Can be added to H1 antihistamines for recalcitrant patients.
Montelukast (Singulair)
Leukotriene inhibitors can be a helpful addition to urticaria not well controlled with H1-receptor blockers.
Adult
10 mg PO qd
Pediatric
<2 years: Not established
2-5 years: 4 mg PO every pm
6-14 years: 5 mg PO every pm
Phenobarbital and rifampin may reduce AUC of montelukast
Documented hypersensitivity
Pregnancy
B - Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
Not indicated for immediate relief of acute asthma symptoms, use appropriate short-acting inhaled beta2-agonist inhaler for exacerbations; not for use as monotherapy in management of exercise-induced bronchospasm (EIB); if already taking montelukast daily (eg, chronic asthma, allergic rhinitis), do not take an additional dose to prevent EIB; administration for chronic asthma has not been established to prevent acute EIB; chewable tab contains phenylalanine, caution with phenylketonuria
Neuropsychiatric events have been reported, and following further FDA evaluation, the prescribing information has been updated to include case reports during postmarketing surveillance that include agitation, aggression, anxiousness, dream abnormalities, hallucinations, depression, insomnia, irritability, restlessness, suicidal thinking and behavior (including suicide), and tremor
Zafirlukast (Accolate)
Inhibits effects by leukotriene receptor, whose activity has been associated with airway edema, smooth muscle contraction, and cellular activity associated with the symptoms.
Adult
20 mg PO bid
Pediatric
5-11 years: 10 mg PO bid
>12 years: 20 mg PO bid


