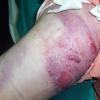
Extremity compartment syndrome
Compartment syndrome (CS) is a limb-threatening and life-threatening condition observed when perfusion pressure falls below tissue pressure in a closed anatomic space. The current body of knowledge unequivocally reflects that untreated compartment syndrome leads to tissue necrosis, permanent functional impairment, and, if severe, renal failure and death.
The original description of the consequences of unchecked rising intracompartmental pressures is widely attributed to Richard vonVolkmann. His 1872 publication documented nerve injury and subsequent contracture from compartment syndrome following supracondylar fracture.1 That injury remains known as Volkmann contracture.
Although long bone fractures are a common cause of compartment syndrome, other injuries are also a common antecedent to compartment syndrome. Approximately 50 years after vonVolkmann's seminal paper, Jepson described ischemic contractures in dog hind legs caused by limb hypertension after experimentally induced venous obstruction. In 1941, Bywaters and Beall reported on the significance of crush injury while working with victims of the London Blitz. These pioneers revealed mechanisms and consequences of compartment syndrome. In the 1970s, the importance of measuring intracompartmental pressures became apparent.
Owen et al published a series of articles describing the use of the wick catheter for pressure measurement and then documented high compartmental pressures in various circumstances.2 Almost simultaneously, Matsen published his findings, which are the most commonly annotated group of articles in present literature.
Compartment syndrome has been found wherever a compartment is present: hand, forearm, upper arm, abdomen, buttock, and entire lower extremity. Almost any injury can cause this syndrome, including injury resulting from vigorous exercise.
This article presents current thoughts and findings regarding compartment syndrome. Most importantly, it urges physicians to maintain a high level of suspicion when dealing with complaints of extremity pain.3
Pathophysiology
Compartment syndrome pathophysiology follows the path of ischemic injury. Intracompartmental structures cannot withstand infinite pressure. When fluid is introduced into a fixed volume, or when volume decreases with fixed volume, pressure rises. Various osseofascial compartments have a relatively fixed volume; introduction of excess fluid or extraneous constriction increases pressure and decreases tissue perfusion, until no oxygen is available for cellular metabolism.
Elevated perfusion pressure is the physiologic response to rising intracompartmental pressure. As intracompartmental pressure rises, autoregulatory mechanisms are overwhelmed and a cascade of injury develops. Tissue perfusion is determined by measuring capillary perfusion pressure (CPP) minus the interstitial fluid pressure. When this pressure falls below a critical threshold, injury results.
Normal cellular metabolism requires 5-7 mm Hg oxygen tension; this is easily maintained with the CPP averaging 25 mm Hg and interstitial pressure 4-6 mm Hg. However, rising interstitial pressure overwhelms perfusion pressure.
Matsen demonstrated that as intracompartmental pressure rises, venous pressure rises. When venous pressure is higher than CPP, capillaries collapse. The pressure at which this occurs is under debate; however, intracompartmental pressures greater than 30 mm Hg are generally agreed to require intervention.
At this point, blood flow through the capillaries stops. In the absence of flow, oxygen delivery stops. Hypoxic injury causes cells to release vasoactive substances (eg, histamine, serotonin), which increase endothelial permeability. Capillaries allow continued fluid loss, which increases tissue pressure and advances injury. Nerve conduction slows, tissue pH falls due to anaerobic metabolism, surrounding tissue suffers further damage, and muscle tissue suffers necrosis, releasing myoglobin. The end result is loss of the extremity and, possibly, the loss of life.
History
- Suspect compartment syndrome (CS) whenever significant pain occurs in an extremity.
- Pressure rises and ischemic injury begins to impair nerve function.
- Nerve impairment causes the patient to complain of severe pain, out of proportion to examination, often described as a burning sensation or tightness.
- The traditional 5 Ps (ie, pain, paraesthesia, pallor, poikilothermia, pulselessness) are not diagnostic of compartment syndrome. Literature warns that, with the exception of pain and paraesthesia, these traditional signs are not reliable, and the presence or absence of them should not affect injury management.
- Importantly, note that these symptoms assume a conscious patient who did not suffer any additional injury that hinders sensory input (eg, spinal cord injury).
- In young children, the ability to gather a history of complaints is limited.
- Maintain a high level of suspicion in any injury that causes limb pain.
- High-velocity injuries are particularly worrisome.
- Determine the mechanism of injury.
- Long bone fractures
- High-energy trauma
- Penetrating injuries (eg, gunshot wounds, stabbings) - Often cause arterial injury, which can quickly lead to compartment syndrome
- Venous injury - May cause compartment syndrome (do not be misled by palpable pulses)
- Crush injuries
- Anticoagulation therapy significantly increases the likelihood of compartment syndrome; remember to ask if patients are anticoagulated for any reason.
- Compartment syndrome requiring fasciotomy has been observed after simple venipuncture in an anticoagulated patient.
- Vigorous exertion may lead to compartment syndrome.
- Compartment syndrome has been found in soldiers and athletes without any trauma. This can be acute or chronic with acute compartment pressures as high as those found in severe trauma.
- If compartment syndrome is suspected, check intracompartmental pressure, even with no presence of any trauma.7
-
- Certain physical signs are associated with compartment syndrome. After initial symptoms of pain or burning, decreased strength and eventually paralysis of the affected extremity occur. Follow-up physical examinations are important to determine if any progression of symptoms is noted.
- Severe pain at rest or with any movement should raise suspicion.
- Pain with certain movements, particularly passive stretching of the muscles, is the earliest clinical indicator of compartment syndrome.
- A patient may report pain with active flexion.
- If a patient complains of pain, determine if any neural compromise is present.
- Sensory nerves begin to lose conductive ability, followed by motor nerves.
- Some nerves may reveal effects of increasing pressure before others.
- For example, in the anterior compartment of the lower leg, the deep peroneal nerve is quickly affected, and sensation in the web space between first 2 toes may be lost.
- The affected limb may begin to feel tense or hard, as if filling with fluid.
- Compare the affected limb to the unaffected limb.
- Any discharged patient should be given these specific signs and return immediately if they develop.
Causes
- A myriad of precipitating injuries leading to compartment syndrome share some pathophysiology.
- The cause of compartment syndrome is extremely simple: the pressure is too high.
- The underlying reason for increasing pressure, as proposed by Mubarak and Hargens, is increased fluid content or decreased compartment size.8
- Increased fluid content can be caused by the following:
- Intensive muscle use (eg, tetany, vigorous exercise, seizures)
- Everyday exercise activities (eg, stationary bicycle use, horseback riding9 )
- Burns
- Intraarterial injection (frequently iatrogenic)
- Envenomation
- Decreased serum osmolarity (eg, nephrotic syndrome)
- Infiltrated infusion
- Hemorrhage (particularly from a large vessel injury)
- Decreased compartment size can be caused by the following:
- Military antishock trousers (MAST)
- Burns
- Casts
- Lying on a limb can cause compartment syndrome. In 1979, Owen et al published a landmark study in which researchers measured intracompartmental pressures in various positions common in drug overdoses.2 Average pressures of 48 mm Hg with the head resting on forearm, 178 mm Hg when the forearm was under ribcage, and 72 mm Hg when one leg was folded under the other were reported.
Laboratory Studies
Laboratory results are often normal and are not necessary to diagnose compartment syndrome (CS) and are not helpful to rule out compartment syndrome.
- Complete metabolic profile (CMP)
- CBC count with differential
- Creatine phosphokinase (CPK) and urine myoglobin levels
- Serum myoglobin level
- Urine toxicology screen: This subsequently may help define the etiology, but it is rarely helpful in patient treatment.
- Initial urinalysis: This may be positive for blood but negative for RBC on microscopic analysis, which may indicate myoglobin in the urine (rhabdomyolysis).
- Prothrombin time (PT) and activated partial thromboplastin time (aPTT)
- Radiography of the affected extremity
- Ultrasonography
- Ultrasonography aids in evaluating arterial flow as well as in visualizing any deep venous thrombosis (DVT).
- Ultrasonography is not helpful in diagnosis of compartment syndrome; however, it aids in the elimination of differential diagnoses.
- Compartment pressure measurement
- This measure should be at the top of the list when searching for compartment syndrome; perform it as soon as the diagnosis of compartment syndrome is considered.
- Numerous commercial model tonometers are available (eg, Stryker, ACE). The Stryker STIC device is shown in the image below.
- Numerous "build-it-yourself" techniques, without evidence of reliability, are also available; their use is not recommended.
- A diagram of a measuring device for use when commercial devices are unavailable
Pulse oximetry
- Pulse oximetry is helpful in identifying limb hypoperfusion.
- Pulse oximetry is not sensitive enough to exclude compartment syndrome
Prehospital Care
Compartment syndrome (CS) can develop rapidly after an arterial injury. Therefore, speed of transport is essential. Perform only the necessary lifesaving procedures in the field if compartment syndrome is suspected.
Emergency Department Care
Time is of the essence in diagnosing and treating compartment syndrome. Irreversible nerve damage begins after 6 hours of intracompartmental hypertension. If compartment syndrome is suspected, pressure measurements and appropriate consultation must be performed quickly.
- Many cases of compartment syndrome are due to trauma. Follow advanced trauma life support (ATLS) guidelines to stabilize the patient before attempting to address compartment syndrome.
- Ischemic injury is the basis for compartment syndrome. Additional oxygen should be administered because it slightly increases partial pressure of oxygen (PO2).
- Keeping extremities level with the body decreases limb mean arterial pressure without changing intracompartmental pressure.
- Do not elevate the affected extremity. Styf and Wiger measured, after an elevation of 35 cm, a decrease in the mean arterial perfusion pressure of 23 mm Hg and no change in intracompartmental pressure.10
- Intravenous (IV) hydration is essential, hypovolemia worsens ischemia.
- Fasciotomy remains the definitive therapy for CS because of its well-documented, limb-saving results.
- Recently, timing and use of fasciotomy have been questioned. Fasciotomy extends hospital stay and changes a closed injury to an open injury, greatly increasing the chance of infection.
- As mentioned above, debate surrounds the threshold for fasciotomy. Numerous authors recommend 30 mm Hg, while others cite 45 mm Hg. Still others urge prophylactic fasciotomy at normal pressures to prevent compartment syndrome.
- Convincing evidence reflects that debate should center on delta-p. Delta-p is a measure of perfusion pressure (diastolic blood pressure minus intracompartmental pressure). Originally used in dogs, delta-p measurements of less than 30 mm Hg were used by McQueen for fasciotomy.11 As a result, several patients with intracompartmental pressures of 40 mm Hg or greater were observed because the delta-p was greater than 30 mm Hg. Criteria were used in 116 patients without sequelae. The converse is also true because patients with intracompartmental pressures less than 30 mm Hg but with high delta-p values have developed compartment syndrome.
- Recent studies have confirmed previously postulated theories that myonecrosis associated with compartment syndrome after envenomation is multifactorial and that fasciotomy may not prevent myonecrosis. Myonecrosis is thought to be due to a direct toxic effect of the venom and the inflammatory response. Therefore, these patients should be aggressively treated with antivenom if available because this has been shown to decrease limb hypoperfusion.
Consultations
- General surgeon
- Orthopedic surgeon
- Vascular surgeon
- Toxicologist
Medication
Some authors have advocated the use of mannitol for compartment syndrome (CS). Although its use in rhabdomyolysis is well documented, its use in acute compartment syndrome is new. More recently, Daniels and Reichman treated an Israeli soldier who developed compartment syndrome with mannitol.12 After resolution, he was discharged without a fasciotomy. Unfortunately, intracompartmental pressures were not measured, since the diagnosis was based on limb circumference and nerve conduction studies. Further investigation is warranted in this area.
Hyperbaric oxygen (HBO) therapy is a logical choice for compartment syndrome because it addresses the primary concern of ischemic injury. HBO has many beneficial effects. It reduces edema through oxygen-induced vasoconstriction while maintaining oxygen perfusion and supports tissue healing in a similar mechanism by allowing oxygen delivery when perfusion pressure is low. Reperfusion injury following CS often is voiced as an argument against HBO. However, HBO actually protects against reperfusion injury.
Bouachour performed a well-controlled randomized study with 31 patients following crush injury and demonstrated significant increase in complete healing (p <0.0005) with HBO. Wattel et al have given an appraisal of the current literature regarding HBO therapy for compartment syndrome and justifiably concluded that studies demonstrate HBO effectiveness in improving wound healing, reducing amputation rate, and lowering surgical procedure rate.13
Although HBO is currently only adjunctive therapy because of its limited availability, it should not be ignored. It may extend treatment duration and it may not reverse the compartment syndrome etiology but has been shown to be beneficial.

