|
Essential telangiectasias = توسع الشعريات الاساسي |
 |
 |
 |
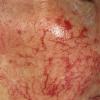 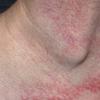 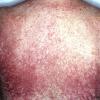 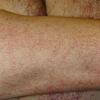  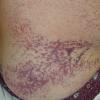  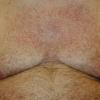  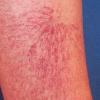
Essential telangiectasias
A telangiectasis refers to a visibly dilated blood vessel on the skin or mucosal surface. Telangiectases that develop in the absence of any preceding or coexisting cutaneous or systemic disease are considered to be primary or essential. Telangiectases resulting from or in association with a known disease state are classified as secondary.
Different presentations of primary telangiectases have been arbitrarily classified as distinct syndromes, designated by terms that often are descriptive based on inheritance, age of onset, anatomic distribution, morphology, prognosis, or associated findings. No recognized nomenclature exists for these telangiectatic disorders. Generalized essential telangiectasia refers to one syndrome of acquired primary telangiectases that are so termed because of their widespread anatomic distribution.1
The pathophysiologic factors causing blood vessel dilatation in generalized essential telangiectasia are yet to be elaborated. Familial cases have been reported with an autosomal dominant pattern of inheritance
- The most commonly observed initial clinical presentation of generalized essential telangiectasia is telangiectasia on the feet, ankles, and distal legs. Subsequently, telangiectases appear more proximally on the lower extremities, and they also may develop on the upper extremities and trunk. In a report of 13 patients, 12 had involvement of the lower extremities. Occasionally, telangiectases first become apparent on the upper extremities or trunk.2
- Bleeding from the ectatic vessels is rare.
- Usually, no family history exists of a similar disorder; however, some familial cases have been reported.
- Generalized essential telangiectasia is usually asymptomatic, but tingling burning or numbness is occasionally reported.
- The age of onset is usually in the fourth or fifth decade, but symptoms may be observed in younger adults.
- The progressive development of the telangiectases, without spontaneous regression, is the usual course.
- In generalized essential telangiectasia, dilated blood vessels represent capillary telangiectases (not venous), ie, they appear red or pink and are usually less than 0.2 mm in diameter, unlike venous telangiectases, which usually appear more blue in color and are greater than 0.2 mm in diameter.
- Most often, generalized essential telangiectasia presents as numerous discrete pink and red capillaries, appearing punctate, linear, or as a lacework or syncytial network. Occasionally, discrete, well-circumscribed, red macules lend the skin a speckled appearance.
- Capillaries are usually bilateral and are symmetrically distributed on the skin. When they are numerous enough to become confluent, the skin appears diffusely erythematous, and discerning individual telangiectases becomes impossible.
- Telangiectases rarely protrude above the normal plane of the skin. Pressure on the skin readily displaces the blood, causing blanching; however, rapid refilling occurs.
- On infrared photography, the underlying venous vasculature appears normal.
- Even in the presence of significant cutaneous involvement, mucous membranes and conjunctivae are not usually affected, although extracutaneous involvement of the oral mucosa and conjunctiva has been reported.3,4,5,6,7 No changes occur within the epidermis or dermis.
Treatment
Capillary telangiectases (red telangiectases, usually <0.2 mm in diameter) in generalized essential telangiectasia, as with randomly occurring capillary telangiectases of the lower extremity, are relatively refractory to treatment. No consistently effective treatment can remove the capillary telangiectases of generalized essential telangiectasia, although case reports describe success using photothermal coagulation with laser and intense pulsed light (IPL).14
Capillary telangiectases should be distinguished from venous telangiectases (blue telangiectases, usually >0.2 mm in diameter). While venous telangiectases are quite responsive to sclerotherapy, capillary telangiectases are usually resistant to sclerotherapy.15 In fact, attempting sclerotherapy to remove capillary telangiectases carries a high risk of local development of new capillary telangiectases. These new capillaries often appear as pink or red patches because the capillaries are so numerous. These patches of capillary telangiectases—a well-recognized effect of sclerotherapy—are known as telangiectatic capillary mattes, and this adverse effect of treatment is known as telangiectatic capillary matting.
- In one case report, a 39-year-old woman with a 7-year history of progressive generalized essential telangiectasia who was treated empirically using tetracycline noted a decrease in the telangiectases within 3 weeks of beginning oral tetracycline, with complete resolution within 3 months.16 Treatment using tetracycline had been initiated empirically in this patient because of the vascular resemblance to tetracycline-responsive rosacea. The mechanism of action of the amelioration remains obscure.
- In another report, a patient with widespread telangiectases along with autoimmune thyroiditis, progressive muscle weakness, and small varicose veins of the legs had complete clearing of the telangiectases after treatment using oral acyclovir.17 Involution was noted within 3 weeks, with almost complete clearance at 2 months. Treatment was continued for 5 months without recurrence. Acyclovir had no effect on the larger ectatic veins, muscle weakness, or thyroiditis. Acyclovir was initiated because of the possibility that a viral infection may have been the underlying cause of an autoimmune syndrome.
- Another report noted the disappearance of generalized telangiectases with ketoconazole18 ; however, in most patients affected by generalized essential telangiectasia, no improvement occurs using these or other medications.
- Cover-up cosmetic makeup and self-tanning lotion can be used to conceal telangiectases. Makeup provides some relief to patients who are self-conscious about their appearance.
Treatment can be attempted with a laser that specifically targets vascular lesions, including long-pulse Nd:YAG (532 nm), long-pulse frequency-doubled Nd:YAG (1064 nm), or flashlamp-pumped pulsed dye laser (585 nm).19,20 However, capillary telangiectases of the lower extremity, unlike those on the face, are not as responsive to photothermal coagulation with currently available vascular lasers. Multiple treatments are usually required, and, often, many of the treated capillaries remain.
|
|
|
|