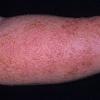
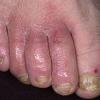
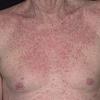
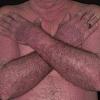
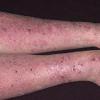
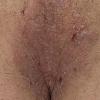
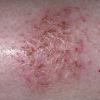
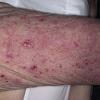
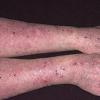
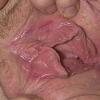
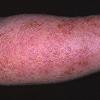

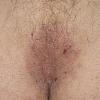
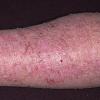
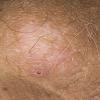
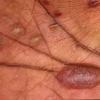
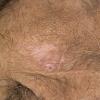
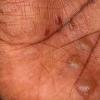
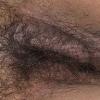
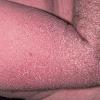
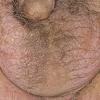
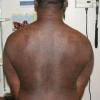
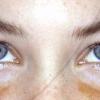
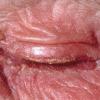

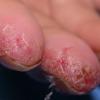

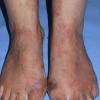
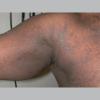
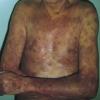
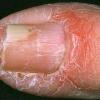
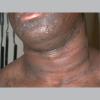
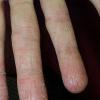
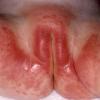
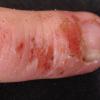

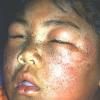

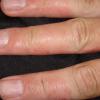
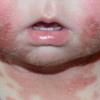
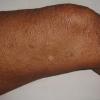

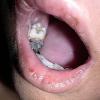
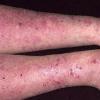
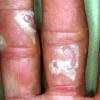
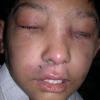




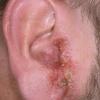

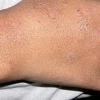
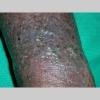
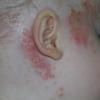
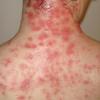
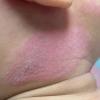
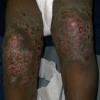
eczema
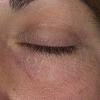
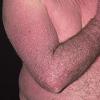
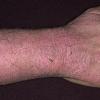
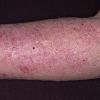
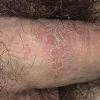
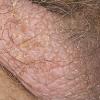
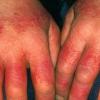
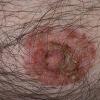
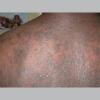
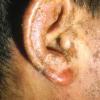
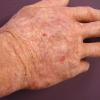
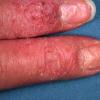
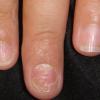
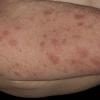
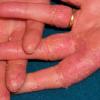
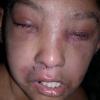
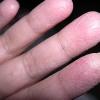
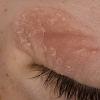
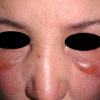
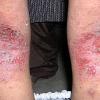
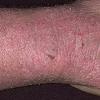
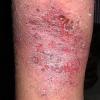
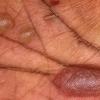
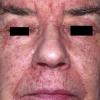
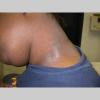
The term eczema is derived from the Greek, meaning "to boil out." The name is particularly apt since to ancient medical practitioners it may have appeared that the skin was "boiling." Today the usage is rather imprecise since it is frequently used to describe any sort of dermatitis (inflammatory skin conditions). Not all dermatitis is eczematous. All eczematous dermatitis has a similar appearance. Acute lesions are composed of many small fluid-filled structures called vesicles that usually reside on red, swollen skin. When these structures break, the fluid leaks out, causing characteristic weeping and oozing. When the fluid dries, it produces a thin crust. In older lesions, these vesicles may be harder to appreciate, but an examination of the tissue under the microscope will reveal their presence. Eczematous dermatitis has many causes. One of the most common is a condition called atopic dermatitis. Often those using the term eczema are referring to atopic dermatitis. Although atopy refers to a lifelong. inherited (genetic) predisposition to inhalant allergies such as asthma and allergic rhinitis (hay fever), atopic dermatitis is not an allergic disease. Atopic patients are likely to have asthma, hay fever, and dermatitis. Atopy is a very common condition, and it affects all races and ages, including young infants. About 1%-2% of adults have the skin rash, and it is even more common in children. Most affected individuals have their first episode before 5 years of age. For most, the disease will improve with time. For an unlucky few, atopic dermatitis is a chronic, recurrent disorder.
Other eczematous dermatoses include, but are not limited to, allergic contact dermatitis (cell-mediated allergy to a common substance such as poison oak or nickel), irritant dermatitis (from excessive contact with a chemical substance), fungal infections, scabies infestations, stasis dermatitis, asteatosis, pompholyx (dyshidrosis), nummular dermatitis, and seborrheic dermatitis. The differentiation among these conditions is often difficult and time-consuming. In addition, it is not uncommon for atopic dermatitis to coexist with another eczematous dermatitis.
Eczema Causes
It is generally agreed that the tendency to atopy is genetically inherited. People with eczematous dermatitis have a variety of abnormal immunologic findings which are probably related to more than one genetic defect. For example, such individuals tend to have elevated IgE antibody (immunoglobulin E) levels and have difficulty in fighting off certain viral, bacterial, and fungal infections.
Like most other noninfectious diseases, atopic skin disease can be triggered by environmental factors.
- One of the hallmarks of atopic dermatitis is excessive skin dryness, which seems to be due a lack of certain skin proteins. Any factor that promotes dryness is likely to exacerbate atopic dermatitis.
- Common triggers of atopic dermatitis include the following:
- Harsh soaps and detergents
- Solvents
- Low humidity
- Lotions
- Rough wool clothing
- Sweating
- Occlusive rubber or plastic gloves
- Rubbing
- Staphylococcal bacteria
- Repeated wetting and drying of the skin (food handling)
Eczema Symptoms and Signs
Medical professionals sometimes refer to eczema as "the itch that rashes."
- Usually, the first symptom of eczema is intense itching.
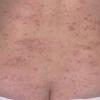
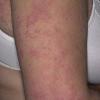
- The rash appears later and is red and bumpy.
- The rash itches or burns.
- If it is scratched, it may ooze and become crusty.
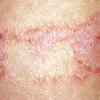
- In adults, chronic rubbing produces thickened plaques of skin.
- Some people develop red bumps or clear fluid-filled bumps that look "bubbly" and, when scratched, add wetness to the overall appearance.
- Painful cracks can develop over time.
- Although the rash can be located anywhere on the body, in adults it is most often found on the neck, flexures of the arms (opposite the elbow) and flexures of legs (opposite the knee). Infants may exhibit the rash on the torso and face. As the child begins to crawl, the rash involves the skin of the elbows and knees. The diaper area is often spared
Exams and Tests
A medical professional can usually identify the type of eczematous dermatitis by looking at the rash and asking questions about how it appeared. Samples of scale from the rash may need to be examined microscopically to search for a fungus. Occasionally, a portion of skin may be removed (a biopsy) to be examined by a pathologist.
The three key elements in identifying atopic dermatitis are
- characteristic appearance and distribution of a chronic rash;
- severe itching;
- atopy, or a personal or family tendency toward asthma and hay fever.
Eczema Treatment
Self-Care at Home
Removing whatever is causing the allergic reaction is the easiest and most effective treatment. This may be as simple as changing your laundry detergent or as difficult as moving to a new climate or changing jobs.
Prevent dry skin by taking warm (not hot) showers or baths. Use a mild soap or body cleanser. Prior to drying off, apply an effective emollient to your wet skin.. Emollients are substances that inhibit the evaporation of water. Generally, they are available in jars and have a "stiff" consistency. They do not flow and ought to leave a shine with a slightly greasy feel on the skin. Most good emollients contain petroleum jelly although certain solid vegetable shortenings do a more than creditable job.
Avoid wearing tight-fitting, rough, or scratchy clothing.
Avoid scratching the rash. If you can't stop yourself from scratching, cover the area with a dressing. Wear gloves at night to minimize skin damage from scratching.
Anything that causes sweating can irritate the rash. Avoid strenuous exercise during a flare.
An anti-inflammatory topical agent may be necessary to control a flare of atopic dermatitis.
- Apply an nonprescription steroid cream (1% hydrocortisone). The cream must be applied as often as possible without skipping days until the rash is gone.
- Diphenhydramine (Benadryl) in pill form may be taken for the itching. Caution: This medication may make you too drowsy to drive a car or operate machinery safely.
- Clean the area with a hypoallergenic soap as necessary. Apply an emollient over the topical steroid.
Avoid physical and mental stress. Eating right, light activity, and adequate sleep will help you stay healthy, which can help prevent flares.
Do not expect a quick response. Atopic dermatitis is controllable but consistency in application of treatment products is necessary.
Medical Treatment and Medications
Once your health-care provider is sure you have atopic dermatitis, the mainstays of therapy are anti-inflammatory medications and relief from the itching.
Prescription-strength steroid cream and antihistamine medications are the usual treatments.
If your health-care provider determines that you have a secondary bacterial infection complicating your rash, an oral antibiotic may be prescribed.
For severe cases not responding to high-potency steroid cream, alternate treatments may be tried. These include coal tar, PUVA (psoralen + ultraviolet A light), and chemotherapeutic agents.
Allergy shots (immunotherapy) usually do not work in eczema.
Follow-up
- Take all your medicines as prescribed and expect slow improvement.
- Keep the affected area as clean, dry, and protected as possible to avoid further breakdown of the skin and prevent infection.
- Apply steroid cream until the rash has completely gone away.
- If prescription medications are not controlling the eczema or your prescription medications are running out, make an appointment with your health-care provider.
- Watch the area carefully for signs of infection: increased redness, warmth, pain, pustules, or a discharge from the area. See your health-care provider if you suspect infection.


