
Drug pigmentation
Hyperpigmentation has multiple causes and may be focal or diffuse. Most cases are due to an increase in melanin production and deposition.
Focal hyperpigmentation is most often postinflammatory in nature, occurring after injury (eg, cuts and burns) or other causes of inflammation (eg, acne, lupus). Focal linear hyperpigmentation is commonly due to phytophotodermatitis, which results from ultraviolet light combined with furocoumarins in limes, celery, and other plants.
Hyperpigmentation also has systemic and neoplastic causes.
Melasma (chloasma): Melasma consists of dark brown, sharply marginated, roughly symmetric patches of hyperpigmentation on the face (usually on the forehead, temples, and cheeks). It occurs primarily in pregnant women (melasma gravidarum, or the mask of pregnancy) and in women taking oral contraceptives. Ten percent of cases occur in non-pregnant women and dark-skinned men. Melasma is more prevalent and lasts longer in people with dark skin.
Because all cases are associated with sun exposure, the mechanism probably involves overproduction of melanin by hyperfunctional melanocytes. Other than sun exposure, aggravating factors include
In women, melasma fades slowly and incompletely after childbirth or cessation of hormone use. In men, melasma rarely fades.
Treatment depends on whether the pigmentation is epidermal or dermal; epidermal pigmentation becomes accentuated with Wood's light or can be diagnosed with biopsy. Only epidermal pigmentation responds to treatment. First-line therapy includes a combination of hydroquinone 2 to 4%, tretinoin 0.05 to 1%, and a class V to VII topical corticosteroid. Hydroquinone 3 to 4% applied bid is often effective, but long courses are usually required; 2% hydroquinone is useful as maintenance. Hydroquinone should be tested behind one ear or on a small patch on the forearm for 1 wk before use on the face because it may cause irritation. Bleaching agents, such as 0.1% tretinoin and azelaic acid 15 to 20% cream, can be used in place of or with hydroquinone . Chemical peeling with glycolic acid or 30 to 50% trichloroacetic acid is an option for patients with severe melasma unresponsive to topical bleaching agents.
Lentigines: Lentigines (singular: lentigo) are flat, tan to brown oval spots. They are commonly due to chronic sun exposure (solar lentigines; sometimes called liver spots) and occur most frequently on the face and back of the hands. They typically first appear during middle age and increase in number with age. Although progression from lentigines to melanoma has not been established, lentigines are an independent risk factor for melanoma. They are treated with cryotherapy or laser; hydroquinone is not effective.
Nonsolar lentigines are sometimes associated with systemic disorders, such as Peutz-Jeghers syndrome (in which profuse lentigines of the lips occur), multiple lentigines syndrome (Leopard syndrome), or xeroderma pigmentosum.
Diffuse hyperpigmentation due to systemic disorders: Common systemic causes include Addison's disease (see Adrenal Disorders: Addison's Disease), hemochromatosis (see Iron Overload: Primary Hemochromatosis), and primary biliary cirrhosis (see Fibrosis and Cirrhosis: Primary Biliary Cirrhosis (PBC)). Skin findings are nondiagnostic as to cause.
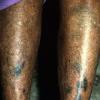
Drug-induced hyperpigmentation: Changes are usually diffuse but sometimes have drug-specific distribution patterns or hues (see Table 1: Pigmentation Disorders: Hyperpigmentation Effects of Some Drugs and Chemicals Tables ). Mechanisms include
Tables ). Mechanisms include
Focal hyperpigmentation frequently follows drug-induced lichen planus (also known as lichenoid drug reactions).
|
Table 1
|
 |
 |
 |
| Hyperpigmentation Effects of Some Drugs and Chemicals |
|
Substance
|
Effect
|
|
Drugs
|
|
Amiodarone
|
Slate-gray to violaceous discoloration of sun-exposed areas; yellowish-brown deposits in the dermis
|
|
Antimalarials
|
Yellow-brown to gray to bluish black discoloration of pretibial areas, face, oral cavity, and nails; drug-melanin complexes in the dermis; hemosiderin around capillaries
|
|
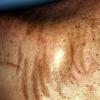
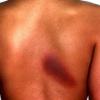
Bleomycin
|
Flagellate hyperpigmented streaks on the back, often in areas of scratching or minor trauma
|
|
Cancer chemotherapy drugs, including busulfan , cyclophosphamide , dactinomycin , daunorubicin , and 5- fluorouracil (5-FU)
|
Diffuse hyperpigmentation
|
|
Desipramine
Imipramine
|
Grayish blue discoloration on sun-exposed areas; golden-brown granules in upper dermis
|
|
Hydroquinone
|
Bluish black discoloration of ear cartilage and face after years of use
|
|
Phenothiazines, including chlorpromazine
|
Grayish blue discoloration on sun-exposed areas; golden-brown granules in upper dermis
|
|
Tetracyclines, particularly minocycline
|
Grayish discoloration of teeth, nails, sclerae, oral mucosa, acne scars, face, forearms, and lower legs
|
|
Heavy metals
|
|
Bismuth
|
Blue-gray discoloration of face, neck, and hands
|
|
Gold
|
Blue-gray deposits around the eyes (chrysiasis)
|
|
Mercury
|
Slate-gray discoloration of skinfolds
|
|
Silver
|
Diffuse slate-gray discoloration (argyria), especially in sun-exposed areas
|
|
In fixed drug eruptions, red plaques or blisters form at the same site each time a drug is taken; residual postinflammatory hyperpigmentation usually persists. Typical lesions occur on the face (especially the lips), hands, feet, and genitals. Typical inciting drugs include sulfonamides, tetracycline , NSAIDs (especially phenazone derivatives), barbiturates, and carbamazepine .