

Cowden disease
Cowden disease, also termed Cowden syndrome and multiple hamartoma syndrome, is an autosomal dominant condition with variable expression that results most commonly (80%) from a mutation in the PTEN gene on arm 10q, as reported by Liaw et al.1 Originally described in 1963 by Lloyd and Dennis, Cowden disease (multiple hamartoma syndrome) was named after the family in which it was first reported.2 A broader category, PTEN (phosphatase and tensin homolog) hamartoma tumor syndrome includes Cowden disease (multiple hamartoma syndrome), Bannayan-Riley-Ruvulcaba syndrome (BRRS), Proteus syndrome, and Proteuslike syndrome, which all have PTEN mutations. Rare cases of Cowden disease (multiple hamartoma syndrome) are due to a germline mutation in the BMPR1A (bone morphogenetic proteins) gene.
Cowden disease (multiple hamartoma syndrome) causes hamartomatous neoplasms of the skin and mucosa, GI tract, bones, CNS, eyes, and genitourinary tract. Skin is involved in 90-100% of cases, and the thyroid is involved in 66% of cases.
Mucocutaneous features of Cowden disease (multiple hamartoma syndrome) include trichilemmomas, oral mucosal papillomatosis, acral keratoses, and palmoplantar keratoses. Cowden disease (multiple hamartoma syndrome) is associated with the development of several types of malignancy, which is why recognition of individuals with the syndrome is important. In particular, a marked increase is seen in the incidence of breast carcinoma in women and of thyroid carcinoma in both men and women. Reports also exist of several other types of malignancies, such as colon cancer and renal cell carcinoma, in patients with Cowden disease (multiple hamartoma syndrome).
Cowden disease (multiple hamartoma syndrome) is caused by a mutation in the PTEN tumor suppressor gene (also termed MMAC1 or TEP1) on band 10q23.3. The protein product of the gene is a phosphatase that regulates the function of other proteins by removing phosphate groups from those molecules. The PTEN protein product negatively controls the phosphoinositide 3-kinase–signaling pathway for regulating cell growth and survival by dephosphorylating the 3 position of phosphoinositide.
The PTEN protein is believed to promote cell death. A mutation that causes loss of the protein's function may result in overproliferation of cells, resulting in hamartomatous growths. Part of this overproliferation may be due to some interaction between the PTEN tumor suppressor gene and a more widely known tumor suppressor gene, TP53. PTEN mutations have been found to occur most frequently in association with endometrial cancer, glioblastomas, and prostate cancer.
Identical mutations in PTEN have been described in Bannayan-Ruvulcaba-Riley syndrome (BRRS). Alternate names for BRRS include Bannayan-Zonana syndrome, Riley-Smith syndrome, and Ruvulcaba-Myhre-Smith syndrome.4 Patients with BRRS have a much lower predisposition to cancer, which suggests that a mutation in the PTEN gene is not the only factor responsible for the clinical features of the disease.
A percentage of patients with Proteuslike syndromes, adult Lhermitte-Duclos disease (LDD), and autismlike disorders associated with macrocephaly have also demonstrated PTEN mutations.
Approximately 18% of Cowden disease (multiple hamartoma syndrome) patients are negative for PTEN mutations and have no identified genetic explanation for their clinical features. Various other possible mechanisms of PTEN inactivation have been explored, but no clear answer has been identified.
Most patients present to the physician because of cutaneous manifestations. Individuals suspected of having Cowden disease (multiple hamartoma syndrome) should be questioned carefully about other family members with malignancies, especially concerning the breast and thyroid. A more detailed family history, including other cutaneous and mucosal lesions and cancers, as well as the developmental and neurologic abnormalities, may be helpful. A full review of systems also is warranted.
l
A baseline full physical examination with yearly follow-up examinations to help detect early changes resulting from malignancies is an essential component of Cowden disease (multiple hamartoma syndrome) patients' management. The physical signs that may be present with Cowden disease (multiple hamartoma syndrome) are discussed below.
Mucocutaneous surfaces
In 90-100% of patients, 1 of 4 types of mucocutaneous lesions is present.
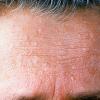
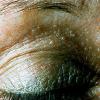
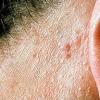
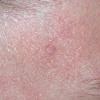
Cutaneous facial papules are present. Most patients exhibit either flesh-colored, flat-topped lichenoid, or elongated verrucoid papules. The lesions may have a central keratin-plugged center and a diameter ranging from 1-5 mm. Typically, large numbers of lesions are present and have a predisposition for the periorificial region. Most of these lesions are trichilemmomas
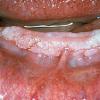
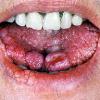
Oral lesions are common. Papules are 1-3 mm with a smooth surface and a whitish appearance and are present in the gingival, labial, and palatal surfaces of the mouth in more than 80% of patients. Lesions often coalesce into confluent sheets, which are described as having a cobblestone appearance. Histologically, they are benign fibromas. Thickening or furrowing of the tongue (scrotal tongue) also may be present
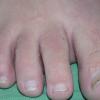
Acral keratoses are flesh-colored or slightly pigmented smooth or verrucoid papules on the dorsal hands and feet, and they occur in more than 60% of patients. The lesions must be differentiated from verruca plana and acrokeratosis verruciformis.
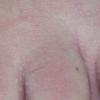
Palmoplantar keratoses are noted. Approximately 40% of Cowden disease (multiple hamartoma syndrome) patients have translucent punctate keratoses on the palms or soles. These need to be distinguished from benign keratoses and arsenic-induced keratoses.
Other cutaneous lesions may occur. Less frequently noted lesions include lipomas, neuromas, and hemangiomas and sclerotic fibromas. A report in 2006 documents multiple mucosal neuromas as the presenting sign of Cowden syndrome, adding this syndrome to the differential diagnosis list for multiple mucosal neuromas.8 Multiple sclerotic fibromas are also documented by Requena et al as a cutaneous marker for Cowden disease (multiple hamartoma syndrome).9
Head, nose, eyes, and throat
Findings may include macrocephaly (in as many as 80% of patients), adenoid facies, eye findings (in as many as 13% of patients, including angioid streaks, myopia), small jaw, and a high-arched palate.
Thyroid lesions
Abnormalities of the thyroid are present in approximately 60% of patients. Manifestations include goiter, benign adenomas, thyroglossal duct cysts, and follicular adenocarcinomas. Patients should be followed carefully for the development of thyroid carcinoma.
Breast disease
Carcinoma of the breast occurs in 20-36% of female patients and is one of the most serious consequences of Cowden disease (multiple hamartoma syndrome). Carcinoma of the breast also has been reported in 2 men with Cowden disease (multiple hamartoma syndrome).10 Fibrocystic disease and fibroadenomas are present in approximately 75% of patients.
GI tract
GI abnormalities are present in as many as 72% of patients. Polyps can occur in the esophagus, stomach, small or large intestine, or anus and are most common in the colon. Although Chen et al reported a few cases of adenocarcinoma of the colon in Cowden disease (multiple hamartoma syndrome) patients, the malignant potential of polyps is low.11 Esophageal and gingival glycogen acanthosis has been documented in several patients with Cowden disease (multiple hamartoma syndrome).12
Genitourinary tract
The most common genitourinary tract manifestations are ovarian cysts and leiomyomas. The most serious genitourinary tract manifestation is endometrial cancer. One case of endometrial cancer has been reported in an adolescent.13
Teratomas, adenocarcinomas of the urethra and cervix, transitional carcinomas, renal cell carcinomas, and benign urethral polyps have been reported. In 2006, Woodhouse and Ferguson reported multiple bilateral hyperechoic testicular lesions in a small series of 8 male patients with documented PTEN mutations. Further testing indicated no effect on spermatogenesis or testicular function. Biopsies revealed lipomatosis in all but the youngest patient.14
Skeletal abnormalities
These include bone cysts, thoracic kyphosis, and kyphoscoliosis, as well as 1 case of osteosarcoma reported by Yen et al.15
CNS abnormalities
Lhermitte-Duclos disease (dysplastic gangliocytoma of the cerebellum) currently is considered to be part of Cowden disease (multiple hamartoma syndrome) and is caused by hamartomatous growths of the cerebellum. Patients have macrocephaly, slowly progressive cerebellar ataxia (which usually appears in adulthood), and signs of increased intracranial pressure. Cases of Lhermitte-Duclos disease occurring without any other evidence of Cowden disease (multiple hamartoma syndrome) have been reported.
Seven reports in the literature describe meningiomas in patients with Cowden disease (multiple hamartoma syndrome).16
Diagnostic criteria
The National Comprehensive Cancer Network 2008 has proposed operational criteria for the diagnosis of Cowden disease (multiple hamartoma syndrome) that have a few modifications from the original Cowden Syndrome Consortium. Unfortunately, the "pathognomonic" criteria (which include facial trichilemmomas, acral keratoses, papillomatous papules, and mucosal lesions) are not specific enough. The other and more useful criteria are described.
Major criteria
- Breast cancer
- Thyroid carcinoma, especially follicular thyroid carcinoma
- Macrocephaly (>97 percentile)
- Lhermitte-Duclos disease
- Endometrial cancer
Minor criteria
- Other thyroid lesions (eg, adenoma, multinodular goiter)
- Mental retardation (intelligence quotient <75)
- GI hamartomas
- Fibrocystic disease of the breast
- Lipomas
- Fibromas
- Genitourinary tumors (eg, uterine fibroids, renal cell carcinoma) or malformations
Operational diagnosis in an individual
- Mucocutaneous lesions alone meet the criteria if (1) 6 or more facial papules are present, of which 3 or more must be trichilemmomas; (2) cutaneous facial papules and oral mucosal papillomatosus are present; (3) oral mucosal papillomatosus and acral keratoses are present; or (4) 6 or more palmoplantar keratoses are present.
- Two major criteria, but one must include either macrocephaly or Lhermitte-Duclos disease
- One major and 3 minor criteria
- Four minor criteria
Operational diagnosis in a family in which one individual is diagnostic for Cowden disease (multiple hamartoma syndrome)
- One pathognomonic criterion
- Any single major criterion with or without minor criteria
- Two minor criteria
- History of Bannayan-Riley-Ruvulcaba syndrome
Causes
Cowden disease (multiple hamartoma syndrome) is caused by a mutation in the tumor suppressor gene PTEN (also termed MMAC1 or TEP1) on band 10q23. At least 80% of Cowden disease (multiple hamartoma syndrome) patients have a PTEN mutation. Sixty percent of Bannayan-Riley-Ruvalcaba syndrome patients have a similar mutation.
PTEN is a lipid phosphatase that removes phosphate groups from signaling molecules. This activity normally restricts growth and survival signals, allowing for normal cell death. When PTEN is mutated, some cells are allowed to proliferate, sometimes (as in cancer) uncontrollably. Cowden disease (multiple hamartoma syndrome) is inherited as an autosomal dominant condition. The percent of cases resulting from new mutations is unknown. An infant with Proteus syndrome born to a mother with Cowden syndrome also correlates these 2 diseases with the PTEN mutation.17
Laboratory Studies
Because a large number of hamartomas and malignancies have been reported in patients with Cowden disease (multiple hamartoma syndrome), monitoring patients closely using appropriate laboratory procedures is essential. Perform the following laboratory studies at baseline and as indicated clinically in subsequent years:
- CBC count: Anemia can be a sign of malignancy (usually from GI blood loss), and an abnormal WBC count may indicate a lymphoproliferative disorder.
- Thyroid function tests: A high risk of thyroid disease (including goiter, Hashimoto thyroiditis, adenomas, and carcinomas) exists in patients with Cowden disease (multiple hamartoma syndrome); therefore, routine monitoring is appropriate.
- Urinalysis: Check for proteinuria or hematuria that may indicate kidney or bladder neoplasia.
- Chemistry panels: These should include a calcium level to screen for parathyroid disease and liver function tests to detect possible hepatocellular carcinoma.
- Skin biopsy: Perform skin biopsy for the pathologic diagnosis of potential trichilemmomas or sclerotic fibromas.
Imaging Studies
Initiate annual or biannual screening mammograms early in women, and perform them regularly to screen for breast cancer. See Medical Care for considerations regarding prophylactic mastectomy. Mammograms in men may be considered, especially if clinically indicated, but men’s risk for breast cancer may not be increased over the general male population.
Chest radiography may be performed, as may thyroid scanning.
Consider MRI of the brain if CNS symptoms are present to exclude Lhermitte-Duclos disease (dysplastic gangliocytoma of cerebellum). Based on a report by Lok et al, obtaining baseline head MRI findings from all patients diagnosed with Cowden disease (multiple hamartoma syndrome) may be reasonable because 35% of the Cowden disease (multiple hamartoma syndrome) patients studied had significant findings when one was obtained.16 Significant CNS symptoms (including headache or other focal neurologic signs) also may indicate the need for a follow-up head MRI in Cowden syndrome patients. A study of Lhermitte-Duclos disease patients using positron emission tomography suggested that these patients should be followed regularly in case of progression of these lesions.18
Perform barium swallow and enema to exclude hamartomas of the GI tract. Alternatively, upper and lower GI endoscopy may be used. Routine occult blood tests should also be performed, although the real increased risk of colon cancer is yet to be determined. Polyps in Cowden syndrome patients may be nonadenomatous, but these hamartomatous polyps have been documented to progress to colonic adenocarcinoma.19
Perform intravenous pyelography if indicated clinically or if urinalysis shows an abnormality. Additionally, ultrasonography of the testes can also be considered. Seven of 8 patients with Cowden syndrome were shown to have testicular lipomatosis.14
Other Tests
A multitude of methodologies are available to detect PTEN deletions in patients suspected to have Cowden disease (multiple hamartoma syndrome). Multiple ligation-dependent probe amplification (MLPA) is currently preferred. Other methods include Southern blotting, monochromosomal hybrid analysis, real-time polymerase chain reaction, and semiquantitative multiplex polymerase chain reaction.7
In practice, no set guidelines are available to determine when a patient is a candidate for PTEN mutation testing. In 2009, Pilarski recommended genetic testing in the following circumstances20 :
- Patients meeting or coming close to meeting the International Cowden Syndrome Consortium diagnostic criteria
- All patients with adult Lhermitte-Duclos disease or multiple trichilemmomas
- Patients with macrocephaly with other Cowden disease (multiple hamartoma syndrome) findings
PTEN mutation analysis is not indicated in patients with breast and thyroid cancer with no other manifestations of Cowden disease (multiple hamartoma syndrome) or in women with double primary cancers such as breast cancer and endometrial cancer with no other signs of Cowden disease (multiple hamartoma syndrome).11
Procedures
Perform fine-needle aspiration or surgical biopsy on thyroid nodules found on physical examination or thyroid imaging studies.
Consider upper and lower GI endoscopy as a screening procedure or to obtain a biopsy specimen of lesions found on the barium study. Esophageal glycogenosis is very suggestive of Cowden disease (multiple hamartoma syndrome).
Submit skin biopsy specimens to a dermatopathologist for pathologic diagnosis of potential trichilemmomas or sclerotic fibromas.
Histologic Findings
Trichilemmomas are lobular proliferations of squamoid cells, often with a distinctive clear (glycogenated) appearance that resembles the outer root sheath of the hair follicle. Peripheral palisading of the lobules is apparent. Lobules often are bound by a thickened eosinophilic basement membrane. A small risk of trichilemmal carcinoma exists, as reported by O'Hare et al in 1 case.21
Sclerotic fibromas or storiform collagenomas are dermal tumors with coarse hyalinized collagen, often arranged in curved, nearly parallel strands with intervening parallel spaces, giving an overall storiform or whorled appearance. Breast fibroadenomas are the hyalinization of fibrous nodules that takes place at a young age.
Medical Care
According to the National Comprehensive Cancer Network 2008, management guidelines for Cowden disease (multiple hamartoma syndrome) include the following:
- Annual history and physical examinations, monthly self-breast examinations, and baseline thyroid ultrasonography beginning at age 18 years (consider repeating annually)
- Clinical breast examinations every 6 months starting at age 25 years (or 5-10 y prior to earliest breast cancer diagnosis in family if younger than 35 y)
- Annual mammography and breast MRI screening at age 30-35 years (or 5-10 y prior to earliest breast cancer diagnosis in family if younger than 40-45 y)
- Consideration of prophylactic mastectomy on case-by-case basis
- Consideration of annual dermatologic examination
- Blind endometrial biopsy at age 30-35 years (or 5 y before earliest diagnosis of endometrial cancer in family); repeat every 12 months in premenopausal women
- Endometrial ultrasonography every 12 months in postmenopausal women
- Consideration of participation in clinical trials to determine effectiveness of endometrial and renal cell cancer screening
Systemic treatments (ie, acitretin) may be used to control some of the cutaneous manifestations of the disease; however, recurrence of lesions is typical after treatment is discontinued.22
Surgical Care
Surgical care of facial papules may include the following:
- Chemical peels
- Laser resurfacing
- Surgery and/or shave excisions only if symptomatic or malignancy is suspected because surgical removal may be complicated by recurrence or keloid formation
Consultations
Consult the following specialists as determined necessary by laboratory test results and physical examination findings:
- Ophthalmologist - For myopia, cataracts, and angioid streaks
- Endocrinologist - If thyroid studies are abnormal
- Gynecologist - For at least annual endometrial biopsy at age 35 years or at 5 years younger than the youngest age of a person in the family with a diagnosis of endometrial cancer
- Neurologist and neurosurgeon - If initial MRI shows cerebellar enlargement or other abnormalities or if patient has a new onset of focal CNS symptoms
- GI or general surgeon - If barium swallow and/or enema shows significant lesions (A consultation may also be obtained if the diagnosis has not yet been established in a suspected case.)
- General surgeon - For mammogram abnormalities or consideration of prophylactic bilateral mastectomy, which some physicians recommend (Walton, et al23 ) due to the 1 in 3 risk of women developing breast cancer
- Radiologist - Annual mammography at age 30 years or at 5 years younger than the youngest age of a person in the family with a diagnosis of breast cancer
Medication
Systemic therapy with retinoids may temporarily control some of the cutaneous lesions of Cowden disease (multiple hamartoma syndrome). Topical treatment usually is unsatisfactory.
Rapamycin has shown great promise in both regression of cutaneous lesions and prevention of the development of manifestations of Cowden disease (multiple hamartoma syndrome) in a mouse model with a PTEN deletion. In the mouse model, rapamycin inhibited a key downstream target, mammalian target of rapamycin (mTOR), which caused rapid regression of Cowden disease (multiple hamartoma syndrome)–like lesions.24 At this time, however, use of rapamycin, should be limited to clinical trials. A clinical trial is currently underway that is studying the effects of rapamycin on syndromes with PTEN mutations.
Also see the following clinical trials:
- Sirolimus to Treat Cowden Syndrome and Other PTEN Hamartomatous Tumor Syndromes
- Sirolimus in Treating Patients With Cowden Syndrome or Another Germline Mutation Syndrome
Retinoids
These agents are partially effective in treating cutaneous lesions.
Acitretin (Soriatane)
Retinoic acid analog similar to etretinate and isotretinoin. Acitretin is the main metabolite of etretinate and has demonstrated clinical effects close to those seen with etretinate. Mechanism of action is suspected to be through its ability to cause increased differentiation of cells.
Adult
10-50 mg PO qd
Pediatric
Not recommended


