Bullosis diabeticorum
Bullous disease of diabetes (bullosis diabeticorum) is a distinct, spontaneous, noninflammatory, blistering condition of acral skin unique to patients with diabetes mellitus. Kramer first reported bullouslike lesions in diabetic patients in 19301 ; Rocca and Pereyra first characterized this as a phlyctenar (appearing like a burn-induced blister) in 1963.2 Cantwell and Martz are credited with naming the condition, bullous diabeticorum, in 1967.3 It is also termed bullous disease of diabetes and diabetic bullae.
Also see the eMedicine articles Diabetes Mellitus, Type 1 and Diabetes Mellitus, Type 2.
Pathophysiology
The etiology of bullous disease of diabetes (bullosis diabeticorum) is not known. Patients with diabetes have been shown to have a lower threshold for suction-induced blister formation, and because of the acral prominence of diabetic bullae, the role of trauma has been speculated; however, this alone does not explain the often spontaneous development of multiple lesions at several locations. The pathophysiology is likely multifactorial.
Many, but not all, patients with bullous disease of diabetes (bullosis diabeticorum) have nephropathy or neuropathy; some authors have hypothesized an etiologic association, possibly related to a local, subbasement, membrane-zone, connective-tissue alteration. Hyalinosis of small vessels noted on biopsy specimens has led some authorities to speculate microangiopathy-associated blister induction. In some, the blisters are related to UV exposure, especially in patients with nephropathy.4 Glycemic control does not appear to have a direct correlation with blister formation.
Some electron microscopic evidence has suggested an abnormality in anchoring fibrils. A reduced threshold to suction-induced blister formation in diabetic persons as compared with nondiabetic controls has been reported.5 Prominent acral accentuation of these lesions suggests a susceptibility to trauma-induced changes, but the definitive explanation awaits elucidation
History
Bullous disease of diabetes blisters occur spontaneously and abruptly, often over night, and usually without known antecedent trauma.
Bullous disease of diabetes lesions tend to be asymptomatic, although mild discomfort or burning has been described.
Bullous disease of diabetes blisters heal spontaneously within 2-6 weeks of onset.
Physical
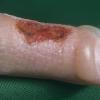
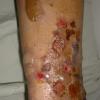
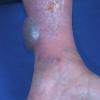
Bullous disease of diabetes (bullosis diabeticorum) manifests as tense, nontender blisters arising on nonerythematous skin. Some blisters may be flaccid.
Bullous disease of diabetes blisters typically occur on the feet or lower legs (see below), but they also may occur on fingers, toes, hands, and arms.
.
Causes
Prominent acral accentuation of bullous disease of diabetes lesions suggests a susceptibility to trauma-induced changes, but the definitive explanation awaits elucidation. Neuropathology, UV exposure, and microangiopathy associated with diabetes also are thought to play a role.
Laboratory Studies
Consider evaluation of porphyrin levels if lesions prominently involve the hands. Elevated levels may indicate porphyria cutanea tarda. Levels reportedly are normal in persons with bullous disease of diabetes (bullosis diabeticorum).
If the bullous disease of diabetes blister fluid is cloudy instead of clear, consider excluding secondary bacterial infection with culture of the blister fluid.
Other Tests
Immunofluorescence: No primary immunologic abnormality is noted. Nonspecific capillary-associated immunoglobulin M and C3 have been reported rarely.8 Immunofluorescence findings have not been consistently reproduced by others, and direct immunofluorescence findings are usually negative.9 This study may be required to exclude clinically similar conditions (eg, bullous pemphigoid, epidermolysis bullosa acquisita) that typically show deposition of C3 and immunoglobulin G along the basement membrane zone.
Procedures
Skin biopsy
- Consider shave biopsy or excisional/incisional biopsy to help distinguish bullous disease of diabetes (bullosis diabeticorum) from clinically similar conditions.
- For routine histologic sections, include the blister and portions of the underlying dermis in the biopsy specimen, and submit it in formalin. For biopsy findings, see Histologic Findings below.
- Histologic features of bullosis diabeticorum are not entirely specific; consider direct immunofluorescence studies to exclude histologically similar entities (eg, noninflammatory bullous pemphigoid, epidermolysis bullosa acquisita, porphyria cutanea tarda). Include perilesional uninvolved skin in biopsy for direct immunofluorescence and submit it in special transport medium (eg, Michel).
Histologic Findings
Lesions of bullous disease of diabetes (bullosis diabeticorum) have a heterogeneous histologic presentation. The blister plane may appear in a subcorneal, intraepidermal, or subepidermal location. Histology of fresh blisters tends to show an epidermal-dermal separation (see image below).
Many of the reported cases describe a separation in the superficial epidermis, within the superficial part of the spinous layer. The variable blister plane may be related to the blister age because reepithelialization can occur within days of blister onset. The blister cavity contains sterile proteinaceous fluid; an inflammatory component is absent or insignificant.
Surrounding epidermis does not show significant change; however, rare reports describe associated spongiosis and degenerative keratinocytic pallor. Acantholysis is absent. Dermal changes (eg, capillary wall thickening, dermal sclerosis) may reflect the patient's underlying diabetes mellitus (see image below). Caterpillar bodies typical of porphyria have been reported in lesions of bullosis diabeticorum.
Electron microscopy of fresh blisters reveals separation in a subepidermal location, residing in the lamina lucida or the sublamina densa.10 Anchoring fibrils and hemidesmosomes are reported absent or decreased in early blisters
Medical Care
Specific treatment of bullous disease of diabetes (bullosis diabeticorum) is unnecessary because the condition is self-limiting. The blister should be left intact whenever possible to serve as a sterile dressing and to avoid secondary infection. Secondary staphylococcal infections may occur, requiring antibiotic therapy.
Helpful guidelines from the American Diabetes Association related to the management of diabetes are as follows:
- Nutrition recommendations and interventions for diabetes: a position statement of the American Diabetes Association11
- Standards of medical care in diabetes. I. Classification and diagnosis12
- Standards of medical care in diabetes. V. Diabetes care.13
Surgical Care
Aspiration of fluid from bullous disease of diabetes (bullosis diabeticorum) lesions with sterile technique using a small-bore needle may be beneficial to prevent accidental rupture. Immobilization may prevent damage to the blister. Secondary tissue necrosis may necessitate debridement and possible tissue grafting.
Aggressive wound healing intervention, as is enacted with diabetic ulcers, is critical, should the blister become unroofed.