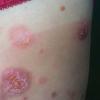 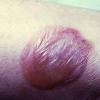
VESICLE AND BULLA
A vesicle is a fluid-filled cavity or elevation smaller than or equal to 0.5 cm, whereas a bulla (blister) measures larger than 0.5 cm. The fluid in the cavity exerts equal pressure in all directions to give rise to a spherical shape. Vesicles may be non-palpable in areas of thicker stratum corneum such as the palm, where their presence may be suggested by a circumscribed translucency or a residual collarette of scale left behind after rupture. Mucosal vesicles rupture easily and may only be noted as an erosion or white thin plaque. Vesicles and bullae arise from cleavage at various levels of the epidermis (intraepidermal) or of the dermal-epidermal interface (sub-epidermal). The amount of pressure required to collapse the lesion may help predict whether the bulla is intraepidermal or sub-epidermal. Reliable differentiation, however, requires histopathologic examination of the blister cavity edge. Cleavage just beneath the stratum corneum produces a subcorneal vesicle or bulla. Intraepidermal vesiculation may result from spongiosis (widened intercellular spaces due to edema) or acantholysis (loss of cohesion between keratinocytes due to the loss of intercellular attachments). “Ballooning degeneration” (cytoplasmic swelling with loss of keratinocyte attachments) of epidermal cells noted in viral infections also results in epidermal vesiculation.
Because of their size, bullae are easily identifiable as tense or flaccid weepy blisters. Once collapsed or torn, blisters may leave behind erosions. The cavity wall is often thin and translucent enough to allow the visualization of contents, which may be clear, serous, hemorrhagic, or pus filled. Cleavage in tense bullae are commonly located at the dermal-epidermal junction. Sub-epidermal blisters are usually a result of mechanical fragility, or autoimmunity to or genetic alteration of a component of the basement membrane zone. A clinical example of vesicle is toxin-producing staphylococcal impetigo
|