Aplasia cutis congenita
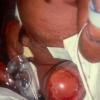
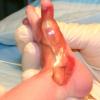
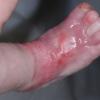
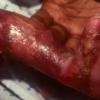
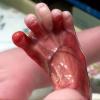
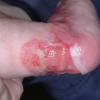
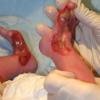
Aplasia cutis congenita (ACC) is part of a heterogenous group of disorders first reported by Cordon in 1767 and is characterized by the absence of a portion of skin in a localized or widespread area at birth. It most commonly (70%) manifests as a solitary defect on the scalp
The lesions are noninflammatory and well demarcated, and they range in size from 0.5-10 cm. Aplasia cutis congenita may be circular, oval, linear, or stellate in configuration. At birth, the lesions may have already healed with scarring or may remain superficially eroded to deeply ulcerated, occasionally involving the dura or the meninges.
Defects in the skin that form early in gestation may heal before delivery and appear as an atrophic, membranous,4 bullous,5 or parchmentlike scar with associated alopecia, whereas less mature defects present as ulcerations. Most lesions occur on the scalp vertex just lateral to the midline, but defects may also occur on the face, the trunk, or the limbs, sometimes symmetrically. The depth may involve only the epidermis and the upper dermis, resulting in minimal alopecic scarring, or the defect may extend to the deep dermis, the subcutaneous tissue, or rarely the periosteum, the skull, and the dura.
Aplasia cutis congenita is most often a benign isolated defect, but it can be associated with other physical anomalies or malformation syndromes.
Frieden1 created a classification system for aplasia cutis congenita (outlined below) consisting of 9 groups based on the number and location of the lesions and the presence or absence of associated malformations.
- Group 1: This is scalp aplasia cutis congenita without multiple anomalies.6 Nearly 86% of all solitary lesions occur on the scalp. A collar of hair is often seen around the defect. It can be autosomal dominant7 or sporadic.8
- Group 2: This is scalp involvement with limb anomalies.9 Adams-Oliver syndrome10,11,12,13,14 is a distinct subtype in which distal limb reduction abnormalities are found in association with solitary midline scalp defects. More than 15 such cases have been reported, usually with an autosomal dominant inheritance pattern and variable genetic expression. The scalp lesions tend to be large. The most common limb malformation is hypoplastic or absent distal phalanges. Other anomalies may include cutis marmorata telangiectatica congenita, hemangiomas, cranial arteriovenous malformation, skin tags, supernumerary nipples, and woolly hair.
- Group 3: This is scalp aplasia cutis congenita with epidermal and sebaceous (organoid) nevi,15,16 which also involve the scalp, usually adjacent to the cutis aplasia. Some patients have also had ophthalmic and neurologic findings typical of epidermal nevus syndrome, including seizures, mental retardation, corneal opacities, and eyelid colobomas. Inheritance is sporadic.
- Group 4: This is aplasia cutis congenita often with a hair collar overlying deeper embryologic malformations.17,18,19,20 Examples include meningomyelocele, porencephaly, leptomeningeal angiomatosis, cranial stenosis, spinal dysraphism, gastroschisis, and omphalocele. The inheritance pattern in this group varies with the associated underlying condition.
- Group 5: This is aplasia cutis congenita associated with fetus papyraceous or placental infarct.21,22,23,24,25 Extensive truncal and limb aplasia cutis congenita in a linear or stellate configuration is associated with the presence of fetus papyraceous. Fetus papyraceous is found at the time of delivery and results from the death of a twin fetus early in the second trimester. The surviving fetus is affected with aplasia cutis congenita and usually is otherwise normal.
- Group 6: This is aplasia cutis congenita associated with simplex, junctional, or dystrophic types of epidermolysis bullosa (EB).26,27,28 Many reports describe aplasia cutis congenita, usually occurring on the lower extremities, in patients eventually diagnosed with EB. Initially described as Bart syndrome, this type of presentation represents a variant of dystrophic EB. A subgroup includes the association of pyloric or duodenal atresia, ureteral stenosis, renal abnormalities, craniofacial abnormalities, nail dystrophy, and aplasia cutis congenita.
- Group 7: This is aplasia cutis congenita localized to the extremities without EB.29,30,31 At least 2 families have been reported in which multiple members have had extensive aplasia cutis congenita on the pretibial lower extremities and the dorsal aspects of the hands and the feet.
- Group 8: This is aplasia cutis congenita due to teratogens. A few cases of aplasia cutis congenita have been linked to intrauterine infection with herpes simplex virus or varicella-zoster virus or to exposure to methimazole32,33,34,35 in the treatment of maternal thyrotoxicosis during pregnancy. Imperforate anus has been associated with methimazole or carbimazole exposure during gestation.
- Group 9: This is aplasia cutis congenita associated with malformation syndromes.36,37 Aplasia cutis congenita has been reported as a characteristic in many syndromes and more will be reported. Various syndromes38,39,40,41 and dysplasias include trisomy 13 (Patau syndrome) with large membranous scalp defects, 4p- (Wolf-Hirschhorn) syndrome with midline scalp defects, Setleis syndrome with bitemporal aplasia cutis congenita and abnormal eyelashes, Johanson-Blizzard syndrome with stellate scalp defects, focal dermal hypoplasia (Goltz syndrome), amniotic band disruption complex, oculocerebrocutaneous (Delleman) syndrome, scalp-ear-nipple syndrome (Finlay-Mark syndrome), Kabuki syndrome,42 and 46XY gonadal dysgenesis. Reticulolinear aplasia cutis congenita on the face and the neck is a distinctive cutaneous manifestation in several syndromes linked to Xp22.
Pathophysiology
The skin and occasionally the underlying structures are affected in aplasia cutis congenita. Lesions are clean, sharply demarcated, and noninflammatory in appearance.
History
- History should include a review of maternal medications taken during the pregnancy and evidence of infections such with varicella or herpes viruses. Because many forms of aplasia cutis congenita are inherited, a thorough family history is important.
Physical
- Aplasia cutis congenita diagnosis is made on the basis of physical findings indicative of an in utero disruption of skin development. Most lesions occur on the scalp lateral to the midline, but they may also occur on the face, the trunk, or the limbs, sometimes symmetrically.
- The lesions are noninflammatory and well demarcated. The appearance of the lesions varies, depending on when they occur during intrauterine development. Lesions that form early in gestation may heal before delivery and appear as an atrophic, membranous, parchmentlike or fibrotic alopecic scar, whereas less mature defects may present as an ulceration of variable depth. With only the epidermis and the upper dermis involved, minimal alopecic scarring may result, but deeper defects may extend through the dermis, the subcutaneous tissue, and rarely the periosteum, the skull, or the dura. Distorted hair growth around a scalp lesion, known as the hair collar sign, is a marker for underlying defects
Causes
- No unifying theory can account for all lesions of aplasia cutis congenita. Because this condition is the phenotypic result of more than one disease process, it is likely that more than one mechanism is involved. Mechanisms include genetic factors, teratogens (eg, methimazole, carbimazole, misoprostol, valproic acid), compromised vasculature to the skin, and trauma. Of particular note is the association of fetus papyraceous with bilaterally symmetric aplasia cutis congenita.
- The proximity of scalp aplasia cutis congenita to the scalp hair whorl, which is thought to be the point of maximum tensile force during rapid brain growth, has led to the hypothesis that tension-induced disruption of the overlying skin occurs at 10-15 weeks of gestation when hair direction, patterning, and rapid brain growth occur.
- Early rupture of the amniotic membranes, forming amniotic bands, has appeared to be the cause of aplasia cutis congenita in several cases.
- The bullous variant of aplasia cutis congenita reveals a distinct histologic pattern identical to those in encephaloceles and meningoceles. This supports a hypothesis that this variant of aplasia cutis may represent the form fruste of a neural tube closure defect.
Other Problems to Be Considered
Few other conditions present with ulcerations or scars in the newborn period. Aplasia cutis congenita (ACC) must be differentiated from the erosions of epidermolysis bullosa (EB); this differentiation is especially important because aplasia cutis congenita may be diagnosed alone before new lesions from EB become apparent.
Neonatal herpes may present with an erosion, often on the scalp, but rarely at delivery. Some lesions have been attributed to fetal varicella.
Lesions are sometimes mistakenly attributed to birth trauma secondary to vacuum extraction, forceps, or fetal scalp monitor electrodes.
Setleis syndrome includes bitemporal aplasia cutis congenita with other facial cutaneous abnormalities and has been termed congenital ectodermal dysplasia of the face.
Transient bullous dermolysis of the newborn is a rare, benign, blistering disease evident at birth or shortly thereafter; this condition resolves during the first months of life leaving no dystrophic scars.
Laboratory Studies
- No specific laboratory abnormalities are consistently found in this condition. Abnormalities due to associated conditions may be present. Chromosome analysis may be indicated if a pattern of abnormalities suggests a genetic disorder.
Imaging Studies
- Imaging studies are seldom required for small circular or oval aplasia cutis congenita of the scalp with no apparent associated anomalies.
- Atypical or very large scalp defects should be imaged for possible underlying bone or soft tissue defects. In one neonate, a ventricular diverticulum of the posterior horn of the lateral ventricle was associated with aplasia cutis congenita of the scalp. It manifested as an expanding bulge of the subdural space.
- Distal radial epiphyseal dysplasia associated with aplasia cutis congenita over the dorsum of the distal forearm has been reported. The cutis aplasia was diagnosed at birth but the radial dysplasia was not recognized until presentation to an orthopedist at age 5-10 years. Radiographs of the involved extremity should be performed in cases of aplasia cutis congenita involving the distal forearm.
Other Tests
- Other tests may be indicated for evaluation of associated conditions.
Histologic Findings
The histologic features of the skin vary according to the depth of the aplasia and its duration. At birth, ulcerated lesions may show a complete absence of skin. After healing, the epidermis may appear flattened with a proliferation of fibroblasts within the connective-tissue stroma and an absence of adnexal structures. Bullous aplasia cutis congenita is a rare clinical subtype of aplasia cutis congenita with distinctive histologic findings. Histologic evaluation of such lesions reveals a distinct pattern containing fibrovascular stromas, edematous stroma, or both. Identical histologic findings are found in encephaloceles and meningoceles.
Medical Care
The decision to use medical, surgical, or both forms of therapy in aplasia cutis congenita (ACC) depends primarily on the size, depth, and location of the cutaneous defect and therapy of associated defects as indicated.43,44,45,46,47,48,49,50,51
- Local therapy includes gentle cleansing and the application of bland ointment or silver sulfadiazine ointment to prevent desiccation of the defect.
- Antibiotics are only indicated if overt signs of infection are noted.
- Other treatment is rarely necessary because the erosions and the ulcerations almost always heal spontaneously.
- A variety of specialized dressing materials have been used.52,53
Surgical Care
- Surgical repair is not usually indicated if the defect is small. Recovery is uneventful, with gradual epithelialization and formation of a hairless, atrophic scar over several weeks. Small underlying bony defects usually close spontaneously during the first year of life.
- Surgical repair of large or multiple scalp defects may require excision with primary closure, if feasible, or the use of tissue expanders and rotation of a flap to fill the defect. Skin and bone grafts may also be required. Occasionally, skin grafting may be required.
- Patients with large, full-thickness scalp defects may face a treatment dilemma: conservative versus surgical therapy of the defect. Complete osseous regeneration of a large skull defect associated with aplasia cutis congenita has been obtained with a conservative approach of skin care and silver sulfadiazine dressings. No surgical treatment of bone or soft tissue reconstruction was necessary. On the other hand, aplasia cutis congenita of the scalp may be complicated by sagittal sinus hemorrhage or thrombosis, and primary closure with scalp flaps may prevent a potentially fatal outcome.
- Truncal and limb defects, despite their large size, usually epithelialize and form atrophic scars, which can later be revised if necessary.
- Patients should be evaluated for evidence of epidermolysis bullosa (EB) before a surgical endeavor is undertaken.
Consultations
- Genetic counseling should be considered if associated anomalies are noted.
- Consultations based on other findings are appropriate to evaluate these conditions.
|

