MALIGNANT FIBROUS
HISTIOCYTOMA
Epidemiology
In the recent past, MFH has been considered to be the most common malignant soft tissue tumor. Reclassification of soft tissue sarcomas by the World Health Organization in 2002 has mandated identification of cell line origin in the classification of tumors. Thus, MFH as previously considered, is merely a morphologic pattern rather than a defined pathologic entity. In most cases, careful immunohistochemical and ultrastructural examination permits probable or definite classification into defined histogenetic sub-types of sarcoma. Currently, MFH remains in the soft-tissue sarcoma nomenclature as a synonym for undifferentiated pleomorphic sarcoma, not otherwise specified. In future reclassification schema, the term MFH may become obsolete.
Keeping the more current classification system in mind, two tumors are more likely to have a cutaneous presentation. The undifferentiated pleomorphic sarcoma, (former pleomorphic and storiform MFH) and the myxofibrosarcoma (former myxoid MFH). Both of these tumors tend to occur on the limbs of elderly patients. Myxofibrosarcoma now represents one of the most common soft tissue sarcoma of the elderly.
Etiology and Pathogenesis
The pathogenesis of soft-tissue sarcomas has not been well defined. Depending on the cell of origin, various genetic, physical, chemical, and viral etiologies have been suggested.
Clinical Findings
HISTORY
Both the undifferentiated pleomorphic sarcoma and the myxofibrosarcoma may present as a subcutaneous mass, most commonly on the limb (or limb girdle in the case of myxofibrosarcoma). Both can be progressively enlarging.
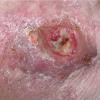
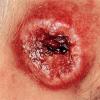
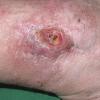
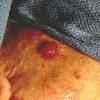
CUTANEOUS LESIONS
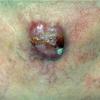
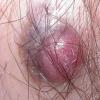
When presenting as cutaneous lesions, these tumors are usually skin-colored subcutaneous nodules, varying from elastic to firm in texture. At times, growth of the tumor may be rapid. It is usually solitary but can be multinodular and may be 5 to 10 cm at the time of initial diagnosis. The more superficial MFH tumors are usually smaller. The extremities are the most common site of involvement, with the lower extremities affected more commonly than the upper extremities. Any area of the body may be involved, and approximately 10 percent to 15 percent of MFH tumors are on the head and neck region.
Laboratory Tests
HISTOPATHOLOGY
The most common appearance is of spindle cells in a storiform pattern. The stroma may be finely fibrillary, myxoid, or densely collagenous. Bizarre epithelioid and giant cells may be present and may contain small amounts of lipid. Many mitotic figures, bizarre giant cells, and necrosis are common. Ultrastructurally, the neoplastic cells have features consistent with fibroblastic, myofibroblastic, and histiocytic differentiation.
SPECIAL TESTS
Immunohistochemistry using a broad antibody panel is required to rule out metastatic carcinoma, lymphoma, leiomyosarcoma, melanoma, and similar lesions.
Prognosis and Clinical Course
Up to 50 percent of patients presenting with an undifferentiated pleomorphic sarcoma may have distant metastases (lung most likely). Recurrence is common, and may result in up to a 30 percent to 35 percent metastatic rate. Low-grade variants, including superficial cutaneous tumors are much less likely to metastasize.
Treatment
Complete surgical resection at presentation offers the best chance for survival. Radiation therapy plays an important role in combination with surgery for better local control, particularly in high-grade lesions and in patients with positive surgical margins after wide complete gross excision. Special note should be made of angiomatoid fibrous histiocytoma (AFH) that occurs primarily in children and young adults. AFH was mistakenly classified as a sub-type of MFH/AFH. Based on AFH's benign behavior and rare ability to metastasize, it is now considered to be a benign tumor of uncertain differentiation. This tumor has four key morphologic features: (1) multinodular proliferation of eosinophilic, histiocytoid, or myoid cells; (2) pseudoangiomatoid spaces; (3) thick fibrous pseudocapsule; and (4) pericapsular lymphoplasmacytic infiltrate. Immunohistochemical studies demonstrate scattered desmin, variable epithelial membrane antigen, and variable CD68+ cells. Laminin and collagen IV are
expressed in this tumor. Ultrastructure demonstrates a pericytic differentiation. The use of reverse transcriptase-polymerase chain reaction for the detection of fusion transcripts (FUS-ATF1 and EWSR1-ATF1) may be helpful in the distinction between AFH and other soft tissue tumors. Some AFH tumors have 11q24 deletions. These tumors require local excision and have an indolent behavior. Recurrence occurs in 2 percent to 10 percent of cases and rarely have metastases been reported (less than 1 percent of cases).