
Lymphogranuloma Venereum
EPIDEMIOLOGY
Lymphogranuloma venereum (LGV) is a rare sexually transmitted disease due to specific Chlamydia variants. It is endemic in East and West Africa, India, Southeast Asia, South and Central America, and some Caribbean islands; and accounts for 2 percent to 10 percent of genital ulcer diseases in areas of Africa and India. The peak incidence occurs in persons 15 to 40 years old, in urban areas, and in individuals of lower socioeconomic status. Men are six times more likely than women to manifest clinical infection. The incidence of LGV is low in the developed world where cases are usually limited to travelers or military personnel returning from endemic areas. Since 2003, however, outbreaks of LGV have appeared in Europe and North America, particularly in the form of proctitis, among human immunodeficiency virus (HIV)-positive men who have sex with men.
LGV is contracted by direct contact with infectious secretions. Transmission efficiency is unknown. Conjugal transmission has been reported. Sexual practices such as fisting and sex-toyssharing may be other routes of transmission. An epidemic of LGV has been reported recently among “crack” cocaine users in the Bahamas.
Due to underdiagnosis and underreporting, the epidemiology of LGV remains poorly understood. Common diagnostic laboratory methods are nonspecific and not readily available in endemic areas. Even in industrialized countries, only a few laboratories offer specific assays to LGV serovars. Without such assays, many LGV cases are misdiagnosed as common chlamydial urogenital infection. Underdiagnosis of LGV is also largely due to the presence of an asymptomatic carrier state.14 Women, in particular, may harbor asymptomatic persistent infection in the cervical epithelium, thus serving as reservoirs of the infection as they do for other urogenital chlamydial infections and gonorrhea. In contrast, infectivity in men ceases after healing of the primary mucosal lesion. Interestingly, most of the detected cases in the recent outbreaks are in men who practice receptive anal sex, suggesting that a high proportion of men who practice insertive anal sex are mis- or undiagnosed. The reasons behind this are unclear but may be organism-related, host-related (sexual practices such as fisting and the use of sex toys, intravenous drug use, HIV-status, etc.) or physician-related (failure to diagnose genital LGV). The resurgence of LGV as a health problem may simply reflect increased awareness rather than increased incidence.
▪ ETIOLOGY AND PATHOGENESIS
LGV (tropical or climatic bubo, lymphopathia venerea, Nicolas-Favre disease) is caused by C. trachomatis serovars L1, L2, and L3. Most of the recent outbreaks are caused by a number of strains of C. trachomatis L2 serovar (L2b), suggesting that these outbreaks most likely represent increased awareness of a slowly evolving endemic.
Chlamydiae are obligate intracellular bacteria characterized by two distinct morphologic forms: the small metabolically inactive and infectious elementary body, and the larger metabolically active and non-infectious reticulate body. In contrast to the A-K serovars that remain confined to the mucosa, LGV serovars have a high affinity for macrophages. After being inoculated onto the mucosal surface, the organisms replicate within macrophages, and find their way to the draining lymph nodes (LNs), and cause lymphadenitis. Entry of the LGV strains into host cells involves cholesterol-rich membrane domains.17 Infection with serovar L2 has been shown to cause caspase-independent apoptosis of host cells.18 Variable expression of members of the polymorphic membrane protein genes (pmpA to pmpI) has been suggested to play a role in the pathogenesis.19
CLINICAL FINDINGS
Cutaneous Lesions and Related Physical Findings
Clinical manifestations are protean, depending on the sex of the patient, acquisition mode, and the disease stage.
PRIMARY STAGE
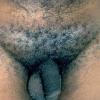
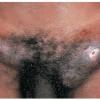
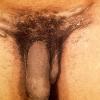
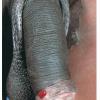
Three to 30 days after infection, 5- to 8-mm painless erythematous papule(s) or small herpetiform ulcers appear at the site of inoculation . Painful ulcerations and non-specific urethritis21 are less common. In males, the lesion is usually found on the coronal sulcus, prepuce, or glans penis; and in females on the posterior
wall of the vagina, vulva, or, occasionally, the cervix. Inoculation may also be rectal or pharyngeal. The primary lesion is transient, often heals within a few days, and may go unnoticed. Other cutaneous manifestations include erythema nodosum, erythema multiforme, urticaria, and scarlatiniform exanthem.
LYMPHOGRANULOMA VENEREUM AT A GLANCE
- · Rare systemic sexually transmitted disease caused by L serovars of Chlamydia trachomatis
- · Endemic in Africa, Southeast Asia, and South and Central America
- · Outbreaks among men who have sex with men in Europe and North America
- · Clinically manifest as inguinal and anorectal syndromes, in three stages
- · Hematogenous spread with manifestations of systemic infection
- · Diagnosis by identification of organism and by serology or genotyping
- · Doxycycline or erythromycin treatment curative if given early
SECONDARY STAGE
A few weeks after the primary lesion appears, marked LN involvement and hematogenous dissemination occur, manifest by variable signs and symptoms, including fever, myalgia, decreased appetite, and vomiting. Photosensitivity may develop in up to 35 percent of the cases, often 1 to 2 months after bubo formation. Less commonly, patients may develop meningoencephalitis, hepatosplenomegaly, arthralgia, and iritis. The lymphadenitis episodes often resolve spontaneously in 8 to 12 weeks. Depending on the mode of transmission, two major syndromes are distinguished:
The acute genital syndrome (GS) or inguinal syndrome is characterized by inguinal and/or femoral LN involvement and is the major presentation in men. Initially, the skin overlying the affected LN is erythematous and indurated. Over the subsequent 1 to 2 weeks, the LN enlarge and coalesce to form a firm and tender immovable mass , which may rupture and drain through the skin, forming sinus tracts. Bilateral involvement occurs in one-third of the cases . Nodal enlargement on either side of the inguinal ligament, the “groove sign,” is pathognomonic of LGV, but only present in 10 percent to 20 percent of cases, and is rarely bilateral. In women, inguinal lymphadenitis is unusual because the lymphatic drainage of the vagina and cervix is to the deep pelvic/retroperitoneal LN. When these nodes are involved, low abdominal/back pain that exacerbates upon lying supine and pelvic adhesions may ensue.
The acute anorectal syndrome (ArS) is characterized by peri-rectal nodal involvement, acute hemorrhagic proctitis, and pronounced systemic symptoms. It is the most common presentation in women and in homosexual men who practice anal sex. The major source of rectal spread in women is the internal lymphatic drainage of the lower two-thirds of the vagina. Patients may complain of anal pruritus, bloody rectal discharge, tenesmus, diarrhea, constipation and lower abdominal pain.
TERTIARY STAGE
This stage is more seen in women with untreated ArS, and includes rectal strictures (most common) and abscesses, perineal sinuses, rectovaginal fistulae (leading to “watering can perineum”), and “lymphorrhoids” (perianal outgrowths of lymphatic tissue). Late sequelae of the GS are less common and include urethral strictures and genital elephantiasis with ulcers and fistulas (in 4 percent of cases).29 Esthiomene (Greek, “eating away”) is a rare primary infection of the external genitalia (mostly in women), leading to progressive lymphangitis and genital destruction. Infertility and “frozen pelvis” are potential sequelae of ruptured deep pelvic nodes in women.
Other Unusual Manifestations
Extragenito-anal inoculation of LGV is rare. Oropharyngeal infection may manifest initially as pinhead-sized vesicles on the lip, and later on as cervical lymphadenopathy with constitutional symptoms, closely mimicking lymphoma. Supraclavicular and mediastinal lymphadenopathy and pericarditis rarely occur.30-33 Ocular autoinoculation of infected discharges may lead to conjunctivitis with marginal corneal perforation, often with preauricular lymphadenopathy.34 Inhalation of LGV serovars L1 and L2 may accidentally occur in laboratory workers and lead to pneumonitis with mediastinal and supraclavicular lymphadenopathy.
LABORATORY TESTS
Diagnosis of LGV may be difficult, but LGV should be suspected in any patient with infected sexual contacts, genital ulcer, perianal fistula, or bubo. The accuracy of clinical diagnosis may, however, be as low as 20 percent. Laboratory tests are important to establish the diagnosis and are usually divided into two broad categories: non-specific tests that do not distinguish between LGV and non-LGV serovars, and specific LGV tests. In practice, positive test on LN aspirate is considered diagnostic of LGV, in contrast to a positive test on primary genital lesion where further specific testing is required to rule out common chlamydial urogenital infections.
Non-Specific Chlamydial Tests
Frei test, an intradermal skin test assessing delayed hypersensitivity to chlamydial antigens, lacks sensitivity and specificity and is no longer used.
Serology assays are sensitive but nonspecific due to cross-reactivity with other chlamydial infections. In addition, they do not differentiate current from prior infection. The complement fixation test is most commonly used. Titers greater than 1:256 are highly suggestive of LGV and titers below 1:32 exclude the diagnosis unless the disease is in its early stages. The microimmunofluorescence test is more specific but less readily available. Commercially available enzyme immunoassays lack data regarding their sensitivity and specificity for LGV serovars.
Culture studies do not distinguish between LGV and non-LGV serovars; however, a positive culture without centrifugation is highly suggestive of LGV.
Direct fluorescent microscopy uses conjugated monoclonal antibody against C. trachomatis on smears from bubo material or genital swab.
Nucleic acid amplification testing (including polymerase chain reaction) may be performed on almost all specimens; however, its sensitivity and specificity in detecting LGV serovars remain unknown.
Specific Tests for Lymphogranuloma Venereum
Only the Centers for Disease Control and Prevention and a few U.S. laboratories have the capacity to sequence DNA to identify L serovars.7 Recently, a technique combining polymerase chain reaction and restriction fragment length polymorphism has been reported to have adequate specificity in identifying LGV serovars.20 Other newly introduced biomolecular techniques exploring immunemediated lysis, heparin sulfate lysis,40,41 use of pooled antibody,15 and structural genetic differences are promising.
Other Non-Specific Laboratory Findings
Mild leukocytosis, false-positive VDRL, cryoprecipitins, rheumatoid factor, and high serum levels of immunoglobulin A and immunoglobulin G may be present.
DIAGNOSTIC PROCEDURES
Bubo aspiration to obtain material for culture and direct microscopy should be performed through a lateral approach, and may require injection of 2 to 5 mL of sterile saline before the aspiration due to the paucity of milky fluid.39 Proctoscopic examination reveals, in the setting of the ArS, multiple discrete and irregular superficial ulcerations and friable granulation tissue, usually confined to the distal 10 cm of the anorectal canal.
HISTOPATHOLOGIC EXAMINATION
Primary lesions reveal non-specific ulceration with granulation tissue, and endothelial swelling. Organisms are rarely demonstrated using Giemsa stain. Biopsy of affected LN reveals suppurative granulomatous inflammation. Necrotic foci may enlarge into stellate abscesses which, in turn, may coalesce into discharging sinuses. These findings are not specific to LGV and can be found in chancroid, cat-scratch disease, and tularemia, and in some deep fungal infections. The pathology of LGV-proctocolitis is similar to that of Crohn disease and includes crypt distortion, submucosal fibrosis, and follicular inflammation with occasional granuloma formation.
DIFFERENTIAL DIAGNOSIS
In contrast to LGV primary stage, chancroid ulcers are usually larger and more painful, and granuloma inguinale ulcers have abundant friable granulation tissue without associated lymphadenitis. Acute GS may be hard to differentiate from chancroid. Buboes containing little or no pus are, however, more likely to be caused by LGV.39 Suspecting LGV proctitis in HIV-positive men who have had sex with men with signs and symptoms of Crohn disease is important, even in the absence of LGV pathognomonic findings. Both conditions have similar proctoscopic findings; however, Crohn disease is more proximally localized.
COMPLICATIONS
In addition to the complications seen in the tertiary stage, the ulcerative nature of LGV may facilitate the acquisition and transmission of blood-borne pathogens such as HIV. LGV may also lead to immune disturbances ranging from mild gammaglobulinemia to rare but fatal immunoblastic lymphoma.
PROGNOSIS AND CLINICAL COURSE
Antibiotic treatment, if given early, is curative, with the acute ArS responding more dramatically than the acute GS.
Differential Diagnosis of Lymphogranuloma Venereum (Stage-Specific)
- o Ulcerogenital diseases (herpes simplex virus, chancre, chancroid, granuloma inguinale)
- o Neisseria gonorrhoeae and/or common chlamydial urogenital infection
- o Non-infectious causes: Trauma, Zoon balanitis, fixed drug eruption
- o Acute genital syndrome
- § Ulcerogenital diseases with lymphadenopathy (syphilis, chancroid, herpes simplex virus)
- § Incarcerated inguinal hernia
- § Reactive inguinal lymphadenitis to a lower extremity focus of infection
- § Bubonic plague (in endemic areas)
- § Acquired immunodeficiency syndrome
- § Kaposi sarcoma
- o Acute anorectal syndrome
- o Inflammatory bowel disease
- o Oropharyngeal lymphogranuloma venereum
- § Lymphoma
- § Infectious mononucleosis
- § Cat-scratch disease
- · Tertiary stage
- o Malignancy
- o Filariasis and other parasitic infections
- o Pseudoelephantiasis (no lymphadenitis) of tuberculosis and granuloma inguinale
- o Deep fungal infection
- o Hidradenitis suppurativa
- o Trauma
TREATMENT
Oral doxycycline, 100 mg twice daily for 3 weeks, is the treatment of choice. When contraindicated, oral erythromycin base, at a dose of 500 mg four times a day for 3 weeks, may be given. Treatment with azithromycin (1 g once weekly for 3 weeks or in a single dose50) is likely curative but still lacks data regarding its efficacy and safety in pregnancy. Therapy may be prolonged in HIV-positive patients and, in general, should not be stopped until the complete resolution of all signs and symptoms (Box 203-2).
Surgery is often required in late stages and includes lateral aspiration of buboes through intact skin (direct incision has a high risk of fistula formation), rectal stricture dilatation, abscess drainage, rectovaginal fistula repair, genital reconstruction, and colostomy. Avoidance of
sexual activity until complete resolution of signs and symptoms is important.51
Treatment of Lymphogranuloma Venereum
|
First line
|
Oral doxycycline
|
100 mg bid
|
3 wk
|
|
Second line
|
Oral erythromycin
|
500 mg qid
|
3 wk
|
|
Third line
|
Oral azithromycin
|
1 g/once weekly
|
3 wk
|
PREVENTION
Effective control should include periodic evaluation of high-risk individuals; reinforcement of health education aiming at early recognition, and counseling; improving community and clinician awareness of LGV; and increasing the availability of specific diagnostic tests. All sexual contacts should be traced and treated. LGV case reporting should be mandatory by law for more reliable monitoring of prevalence trends.


