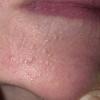
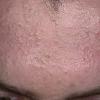
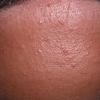
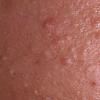
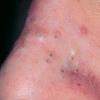
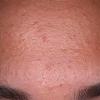
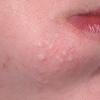
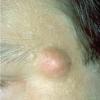


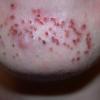

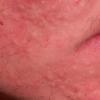
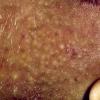
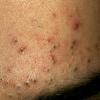





Acne vulgaris
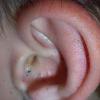
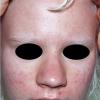
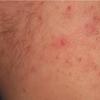
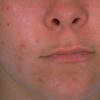
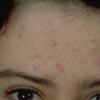
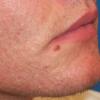
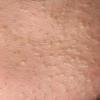
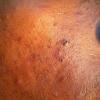
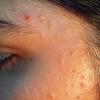
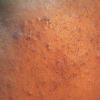
Acne vulgaris is a common skin disease that affects 60-70% of Americans at some time during their lives. Twenty percent will have severe acne, which results in permanent physical and mental scarring. Acne vulgaris is American's most common disease and is characterized by noninflammatory, open or closed comedones and by inflammatory papules, pustules, and nodules. Acne vulgaris affects the areas of skin with the densest population of sebaceous follicles; these areas include the face, the upper part of the chest, and the back.
Other eMedicine articles on acne include Acne Conglobata, Acne Fulminans, Acne Keloidalis Nuchae, and Acneiform Eruptions. Also see the Medscape Acne Resource Center.
Pathophysiology
The pathogenesis of acne vulgaris is multifactorial. The key factor is genetics.1 If both parents had acne, 3 of 4 children will have acne. If 1 parent had acne, then 1 of 4 of the children will have acne. However, similar to other genetic conditions, not every family will have the same pattern, with acne vulgaris sometimes skipping generations. What is inherited is the propensity for follicular epidermal hyperproliferation with subsequent plugging of the follicle. Additional aggravating factors include excess sebum, the presence and activity of Propionibacterium acnes, and inflammation.
Retention hyperkeratosis is the first recognized event in the development of acne vulgaris.2 The exact underlying cause of this hyperproliferation is not known. Currently, 3 leading hypotheses have been proposed to explain why the follicular epithelium produces cells at a rapid rate that are retained in individuals with acne.
History
Local symptoms of acne vulgaris may include pain or tenderness.
Systemic symptoms are most often absent in acne vulgaris. Severe acne with associated systemic signs and symptoms such as fever is referred to as acne fulminans. Additionally, acne vulgaris may have a psychological impact on any patient, regardless of the severity or the grade of the disease.16
Physical
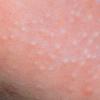
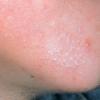
Acne vulgaris is characterized by comedones, papules, pustules, and nodules in a sebaceous gland distribution. A comedone is a whitehead (closed comedone) or a blackhead (open comedone) without any clinical signs of inflammation. Papules and pustules are raised bumps with obvious inflammation. The face may be the only involved skin surface, but the chest, back, and upper arms are often involved.
In comedonal acne, no inflammatory lesions are present. Comedonal lesions are the earliest lesions of acne, and closed comedones are the precursor lesion of inflammatory lesions
First, androgen hormones have been implicated as the initial trigger.3 Comedones, the clinical lesion that results from follicular plugging, begin to appear around adrenarche in persons with acne in the T-zone area. Furthermore, the degree of comedonal acne in prepubertal girls correlates with circulating levels of the adrenal androgen dehydroepiandrosterone sulfate (DHEA-S).4 Additionally, androgen hormone receptors are present in sebaceous glands; individuals with malfunctioning androgen receptors do not develop acne.5
Excess sebum is another key factor in the development of acne vulgaris. Sebum production and excretion are regulated by a number of different hormones and mediators. In particular, androgen hormones promote sebum production and release.6 Still, most men and women with acne have normal circulating levels of androgen hormones. An end-organ hyperresponsiveness to androgen hormones has been hypothesized. Androgen hormones are not the only regulators of the human sebaceous gland. Numerous other agents, including growth hormone and insulinlike growth factor, also regulate the sebaceous gland and may contribute to the development of acne.
P acnes is an anaerobic organism present in acne lesions. The presence of P acnes promotes inflammation through a variety of mechanisms. P acnes stimulates inflammation by producing proinflammatory mediators that diffuse through the follicle wall. Studies have shown that P acnes activates the toll-like receptor 2 on monocytes and neutrophils.7 Activation of the toll-like receptor 2 then leads to the production of multiple proinflammatory cytokines, including interleukins 12 and 8 and tumor necrosis factor. Hypersensitivity to P acnes may also explain why some individuals develop inflammatory acne vulgaris while others do not.8
Inflammation may be a primary phenomenon or a secondary phenomenon. Most of the evidence to date suggests a secondary inflammatory response to P acnes. However, interleukin 1-alpha expression has been identified in microcomedones, and it may play a role in the development of acne.9
Causes
The main underlying cause of acne is a genetic predisposition. The condition is inherited in an autosomal dominant pattern with incomplete penetrance. For example, acne vulgaris may skip a generation. The following aggravating factors are recognized:
- Cosmetic agents and hair pomades may worsen acne.
- Medications that can promote acne development include steroids, lithium, some antiepileptics, and iodides.
- Congenital adrenal hyperplasia, polycystic ovary syndrome, and other endocrinological disorders associated with excess androgens may trigger the development of acne vulgaris. Even pregnancy may cause a flare-up.17
- Mechanical occlusion with headbands, shoulder pads, back packs, or under-wire bras can be aggravating factors
- Excessive sunlight may either improve or flare acne. In any case, the ultraviolet exposure ages the skin.
Laboratory Studies
The diagnosis of acne vulgaris is clinical. Note the following:
- In a female patient with dysmenorrhea or hirsutism, a hormonal evaluation should be considered. Patients with evidence of virilization must have their total testosterone levels measured. Many authorities also measure free testosterone, DHEA-S, leuteinizing hormone, and follicle-stimulating hormone levels.
- Skin lesion cultures to rule out gram-negative folliculitis are warranted if the patient does not respond to treatment or improvement is not maintained.
- Also see the Medscape Acne Resource Center.
Histologic Findings
The microcomedo is characterized by a dilated follicle with a plug of dense keratin. With progression of the disease, the follicular opening becomes dilated, and an open comedo results. The follicular wall thins, and it may rupture. Inflammation and bacteria may be evident, with or without follicular rupture. Follicular rupture is accompanied by dense inflammatory infiltrate throughout the dermis. Later, extensive fibrosis and scarring may develop.
Medical Care
Treatment should be directed toward the known pathogenic factors involved in acne. These include follicular hyperproliferation, excess sebum, P acnes, and inflammation. The grade and severity of the acne help in determining which of the following treatments, alone or in combination, is most appropriate. When a topical or systemic antibiotic is used, it should be used in conjunction with benzoyl peroxide to reduce the emergence of resistance.
Topical treatments
Topical retinoids are comedolytic and anti-inflammatory. They normalize follicular hyperproliferation and hyperkeratinization. Topical retinoids reduce the numbers of microcomedones, comedones, and inflammatory lesions. They may be used alone or in combination with other acne medications. The most commonly prescribed topical retinoids for acne vulgaris include adapalene, tazarotene, and tretinoin. These retinoids should be applied once daily to clean, dry skin, but they may need to be applied less frequently if irritation occurs. Skin irritation with peeling and redness may be associated with the early use of topical retinoids. The use of mild, nondrying cleansers and noncomedogenic moisturizers may help reduce this irritation. Alternate-day dosing may be used if irritation persists. Topical retinoids thin the stratum corneum, and they have been associated with sun sensitivity. Instruct patients about sun protection. Also see Sunscreens and Photoprotection.
Topical antibiotics are mainly used for their role against Propionibacterium acnes. They may also have anti-inflammatory properties. Topical antibiotics are not comedolytic, and bacterial resistance may develop to any of these agents. The development of resistance is lessened if topical antibiotics are used in combination with benzoyl peroxide.18 Commonly prescribed topical antibiotics for acne vulgaris include erythromycin and clindamycin alone or in combination with benzoyl peroxide. Clindamycin and erythromycin are available in a variety of topical agents. They may be applied once or twice a day. Gels and solutions may be more irritating than creams or lotions. Clindamycin has maintained better efficacy than erythromycin.
Benzoyl peroxide products are also effective against P acnes, and bacterial resistance to benzoyl peroxide has not been reported.19 Benzoyl peroxide products are available over the counter and by prescription in a variety of topical forms, including soaps, washes, lotions, creams, and gels. Benzoyl peroxide products may be used once or twice a day. These agents may occasionally cause a true allergic contact dermatitis. More often, an irritant contact dermatitis develops, especially if used with tretinoin or when accompanied by aggressive washing methods. If intensive erythema and pruritus develop, a patch test with benzoyl peroxide is indicated to rule out allergic contact dermatitis.
Systemic treatments
Systemic antibiotics are a mainstay in the treatment of acne vulgaris. These agents have anti-inflammatory properties, and they are effective against P acnes. The tetracycline group of antibiotics is commonly prescribed for acne. The more lipophilic antibiotics, such as doxycycline and minocycline, are generally more effective than tetracycline. Greater efficacy may also be due to less P acnes resistance to minocycline. However, P acnes resistance is becoming more common with all classes of antibiotics currently used to treat acne vulgaris.20 P acnes resistance to erythromycin has greatly reduced its usefulness in the treatment of acne. Subantimicrobial therapy or concurrent treatment with topical benzoyl peroxide may reduce the emergence of resistant strains.
Other antibiotics, including trimethoprim alone or in combination with sulfamethoxazole, and azithromycin, reportedly are helpful.21,22
Some hormonal therapies may be effective in the treatment of acne vulgaris. Oral contraceptives increase sex hormone–binding globulin, resulting in an overall decrease in circulating free testosterone. Combination birth control pills have shown efficacy in the treatment of acne vulgaris.23,24,25,26
Spironolactone may also be used in the treatment of acne vulgaris.27 Spironolactone binds the androgen receptor and reduces androgen production. Adverse effects include dizziness, breast tenderness, and dysmenorrhea. Dysmenorrhea may be lessened by coadministration with an oral contraceptive. Periodic evaluation of blood pressure and potassium levels is appropriate. Pregnancy must be avoided while taking spironolactone because of the risk of feminization of the male fetus.
Isotretinoin is a systemic retinoid that is highly effective in the treatment of severe, recalcitrant acne vulgaris. Isotretinoin causes normalization of epidermal differentiation, depresses sebum excretion by 70%, is anti-inflammatory, and even reduces the presence of P acnes. Isotretinoin therapy should be initiated at a dose of 0.5 mg/kg/d for 4 weeks and increased as tolerated until a cumulative dose of 120-150 mg/kg is achieved. Coadministration with steroids at the onset of therapy may be useful in severe cases to prevent initial worsening. Some patients may respond to doses lower than the standard recommendation dosages. A lower dose (0.25-0.4 mg/kg/d) may be as effective as the higher dose given for the same time period and with greater patient satisfaction. Lower intermittant dosing schedules (1 week out of each month) are not as effective.28
Isotretinoin is a teratogen, and pregnancy must be avoided. Contraception counseling is mandatory, and 2 negative pregnancy test results are required prior to the initiation of therapy in women of childbearing potential. The baseline laboratory examination should also include cholesterol and triglyceride assessment, hepatic transaminase levels, and a CBC count. Pregnancy tests and laboratory examinations should be repeated monthly during treatment.
Associated mood changes and depression have been reported during treatment. Although a cause-and-effect relationship has not been established, patients should be informed of this potential effect and must sign a consent form acknowledging they are aware of this potential risk.29,30
A US Food and Drug Administration–mandated registry is now in place for all individuals prescribing, dispensing, or taking isotretinoin. For more information on this registry, see iPLEDGE. This registry aims to further decrease the risk of pregnancy and other unwanted and potentially dangerous adverse effects during a course of isotretinoin therapy.
While using isotretinoin, the patient is considered at high risk for abnormal healing and the development of excessive granulation tissue following procedures. Many dermatologists delay elective procedures, such as dermabrasion or laser resurfacing (eg, with carbon dioxide laser or erbium:YAG laser), for up to 1 year after completion of therapy. Other procedures to be avoided during therapy include tattoos, piercings, leg waxing, and other epilation procedures.
Surgical Care
Procedural treatments include manual extraction of comedones and intralesional steroid injections. Additionally, some patients may benefit from superficial peels that use glycolic or salicylic acid. Phototherapy using red light or blue light and photodynamic therapy are being assessed as potential treatments for acne.32,33 The usefulness of some fractional laser treatments in the management of acne is also being evaluated.
Consultations
If the patient is feeling depressed while taking isotretinoin, refer him or her to a specialist for help.
Diet
Diet therapy has been suggested. Drs Kligman, Fulton, and Plewig performed a study on chocolate, having teenage patients with acne consume 1 bar of chocolate each day. Some of the patients improved and some worsened, but the vast majority were unchanged. This study helped decrease the emphasis on diet as a causal factor in acne vulgaris. However, investigators always returned to the diet question. Data suggest that the westernization of certain Native American populations and the consumption of unhealthy "junk" foods (eg, potato chips, soft drinks) has had a negative impact on general and skin health, resulting acne flares.
Investigators have also focused on a low-glycemic diet to avoid stress from high-carbohydrate diets and to reduce insulin levels. Studies have been encouraging,34 so the author recommends the "South Beach Diet"35 and provides patients with the glycemic index of foods. The author recommends that acne patients eat nothing higher than 70 on the glycemic index.
Medication
The goals of pharmacotherapy for acne vulgaris are to reduce morbidity and to prevent complications.
Retinoids
These agents decrease the cohesiveness of abnormal hyperproliferative keratinocytes, and they may reduce the potential for malignant degeneration. They also modulate keratinocyte differentiation.
Isotretinoin (Accutane)
Most effective oral medication. Oral agent that treats serious dermatologic conditions. Isotretinoin is synthetic 13-cis isomer of naturally occurring tretinoin (trans -retinoic acid). Both agents are structurally related to vitamin A. Decreases sebaceous gland size and sebum production. May inhibit sebaceous gland differentiation and abnormal keratinization.
An FDA-mandated registry is now in place for all individuals prescribing, dispensing, or taking isotretinoin. For more information on this registry, see iPLEDGE. This registry aims to further decrease the risk of pregnancy and other unwanted and potentially dangerous adverse effects during a course of isotretinoin therapy. Female patients must sign an informed consent that they will use contraceptives during the treatment course and for 30 d after discontinuing therapy.
Adult
Total cumulative dose of 120-150 mg/kg recommended; starting dose should be <0.5 mg/kg/d PO; dose may be increased to 1 mg/kg/d as tolerated
Pediatric
Not established
Toxicity may occur with vitamin A coadministration; pseudotumor cerebri or papilledema may occur when coadministered with tetracyclines; may reduce plasma levels of carbamazepine
Documented hypersensitivity
Pregnancy
X - Contraindicated; benefit does not outweigh risk
Precautions
Obtain 2 negative pregnancy test results in patients of childbearing potential prior to initiating therapy; pregnancy must be avoided during and for 1 mo after treatment, and monthly pregnancy test results must be documented; hyperlipidemia may develop; pseudotumor cerebri, vision impairment, headaches, myalgias, arthralgias, and depression have been reported; dry skin and cheilitis are nearly universal adverse effects
Tretinoin (Retin-A, Retin-A Micro, Avita)
Inhibits microcomedo formation. Normalizes follicular epidermal differentiation and exhibits anti-inflammatory properties. Available as 0.01% and 0.025% gels. Cream formulas are avoided with acne patients because some ingredients may be comedogenic.
Adult
Begin with lowest tretinoin formulation and increase as tolerated; apply hs or qod; lower frequency of application if irritation develops
Pediatric
<12 years: Not established
>12 years: Apply as in adults
Coadministration with benzoyl peroxide may increase irritation; begin with 2 therapies slowly, such as qod
Documented hypersensitivity
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Photosensitivity may occur with excessive sunlight exposure; erythema and peeling may occur (most prominent within first few wk of treatment)
Adapalene (Differin)
A naphthoic acid derivative that binds the retinoic acid receptor. Normalizes follicular epidermal differentiation and exhibits anti-inflammatory properties. Available in cream, gel, solution, and pledget formulations.
Adult
Apply a small amount to involved skin qd
Pediatric
Not established
Documented hypersensitivity
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Erythema and peeling may occur in some individuals; avoid contact with mucous membranes, eyes, mouth, and nostrils; avoid exposure to sunlight and sunlamps; dryness of skin, scaling, erythema, burning, and pruritus may occur
Tazarotene (Tazorac, AVAGE)
Retinoid prodrug whose active metabolite modulates differentiation and proliferation of epithelial tissue; may also have anti-inflammatory and immunomodulatory properties. Available in 0.05% and 0.1% cream and gel formulations.
Adult
Apply sparingly to affected area qd
Pediatric
Children: Not established
Adolescents: Administer as in adults
Use cautiously with dermatologic drugs or cosmetics that have a strong drying effect on the skin (eg, salicylic acid, benzoyl peroxide, astringents)
Documented hypersensitivity
Pregnancy
X - Contraindicated; benefit does not outweigh risk
Precautions
Erythema and peeling may occur at application site
Antibiotics
Topical and systemic antibiotics used in the treatment of acne vulgaris are directed at P acnes. They also have anti-inflammatory properties.
Minocycline (Dynacin, Minocin)
Treats infections caused by susceptible gram-negative and gram-positive organisms, in addition to infections caused by susceptible chlamydial, rickettsial, and mycoplasmal organisms. Available in 50-, 75-, and 100-mg preparations.
Adult
50-100 mg PO bid
Pediatric
<8 years: Not recommended
>8 years: 4 mg/kg PO initially, followed with 2 mg/kg q12h
Bioavailability decreases with antacids containing aluminum, calcium, magnesium, iron, or bismuth subsalicylate; can decrease effects of oral contraceptives, causing breakthrough bleeding and increased risk of pregnancy; tetracyclines can increase hypoprothrombinemic effects of anticoagulants
Documented hypersensitivity; severe hepatic dysfunction
Pregnancy
D - Fetal risk shown in humans; use only if benefits outweigh risk to fetus
Precautions
Photosensitivity may occur with prolonged exposure to sunlight or tanning equipment; reduce dose in renal impairment; consider drug serum level determinations in prolonged therapy; tetracycline use during tooth development (last half of pregnancy through age 8 y) can cause permanent discoloration of teeth; Fanconilike syndrome may occur with outdated tetracyclines; hepatitis or lupuslike syndromes may occur
Doxycycline (Bio-Tab, Doryx, Vibramycin)
Antibacterial agent effective against gram-positive and gram-negative organisms. Available in 20-, 50-, and 100-mg preparations.
Adult
100 mg PO bid
Pediatric
<8 years: Not recommended
>8 years: 2-5 mg/kg/d PO/IV in 1-2 divided doses; not to exceed 200 mg/d
Bioavailability decreases with antacids containing aluminum, calcium, magnesium, iron, or bismuth subsalicylate; tetracyclines can increase hypoprothrombinemic effects of anticoagulants; tetracyclines can decrease effects of oral contraceptives, causing breakthrough bleeding and increased risk of pregnancy
Documented hypersensitivity; severe hepatic dysfunction
Pregnancy
D - Fetal risk shown in humans; use only if benefits outweigh risk to fetus
Precautions
Photosensitivity may occur with prolonged exposure to sunlight or tanning equipment; reduce dose in renal impairment; consider drug serum level determinations in prolonged therapy; tetracycline use during tooth development (last half of pregnancy through age 8 y) can cause permanent discoloration of teeth; Fanconilike syndrome may occur with outdated tetracyclines
Tetracycline (Sumycin)
Antibacterial agent effective against gram-positive and gram-negative organisms.
Adult
250-500 mg PO q6h
Mild-to-moderate infections: 500 mg PO bid or 250 mg PO qid for 7-14 d
Pediatric
<8 years: Not recommended
>8 years: 25-50 mg/kg/d (10-20 mg/lb) PO divided qid
Bioavailability decreases with antacids containing aluminum, calcium, magnesium, iron, or bismuth subsalicylate; can decrease effects of oral contraceptives, causing breakthrough bleeding and increased risk of pregnancy; tetracyclines can increase hypoprothrombinemic effects of anticoagulants
Documented hypersensitivity
Pregnancy
D - Fetal risk shown in humans; use only if benefits outweigh risk to fetus
Precautions
Photosensitivity may occur with prolonged exposure to sunlight or tanning equipment; reduce dose in renal impairment; consider drug serum level determinations in prolonged therapy; tetracycline use during tooth development (last half of pregnancy through age 8 y) can cause permanent discoloration of teeth; Fanconilike syndrome may occur with outdated tetracyclines
Trimethoprim/sulfamethoxazole (Bactrim, Bactrim DS, Septra, Septra DS)
Antibiotic with activity against many gram-positive and gram-negative organisms. Inhibits bacterial growth by inhibiting synthesis of dihydrofolic acid. Available as 80 mg trimethoprim and 400 mg sulfamethoxazole or as 160 mg trimethoprim and 800 mg sulfamethoxazole (double strength).
Adult
160 mg TMP/800 mg SMZ PO q12h
Pediatric
8 mg/kg/d TMP/40 mg/kg/d SMZ PO/IV divided q12h


