|
Ochronosis--usually a symptom of alkaptonuria or phenol poisoning = التمعر |
 |
 |
 |
|
There are two types of ochronosis: endogenous ochronosis (alkaptonuria), which is inherited as an autosomal recessive trait, and localized exogenous ochronosis, which is prototypically caused by the topical application of a hydroquinone cream to exposed parts of the skin in order to lighten the color of dark skin.
|
|
As the result of the lack of homogentisic acid oxidase in endogenous ochronosis, homogentisic acid accumulates over the course of years in many tissues-especially in the cartilages of the joints, the ears, and the nose; in ligaments and tendons; and in the sclerae. This results in osteoarthritis; in blackening of cartilages, ligaments, and tendons; and in patchy pigmentation of the sclerae. In one unusual case, the presenting complaint was
|
|
pigmentation of the palms and soles with overlying hyperkeratosis and pitting . Intervertebral calcification is a characteristic x-ray finding . In the course of time, homogentisic acid accumulates in the dermis in sufficient amounts to cause patchy brown pigmentation of the skin. The gene for homogentisic acid oxidase maps to chromosome 3q .
|
|
In localized exogenous ochronosis, there is a macular blue-black hyperpigmentation of portions of the face to which the hydroquinone cream or other responsible agent was applied . In more severely involved areas, blue-black papules, milia, and nodules can occur. A condition termed pseudo-ochronosis has been recently described as a histopathologic finding in localized argyria occurring primarily in jewelry workers. Clinically, these patients present with blue-black macules ("blue nevus-like") typically on the upper extremities .
|
|
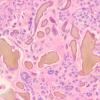
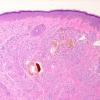
Histopathology. Involvement of the skin is essentially identical in endogenous and exogenous ochronosis, although it is often more pronounced in exogenous ochronosis . The ochronotic pigment, as seen in sections of the dermis stained
|
|
with H&E, has a yellow-brown or ochre color; thus, the name ochronosis.
|
|
The skin shows ochronotic pigment as fine granules free in the tissue and in the endothelial cells of blood vessels, in the basement membrane and the secretory cells of sweat glands, and within scattered macrophages . The most striking finding, however, is the ochronotic pigment within collagen bundles, causing homogenization and swelling of the bundles. Some collagen bundles assume a bizarre shape; they appear rigid and tend to fracture transversely with jagged or pointed ends . As the result of the breaking up of degenerated collagen bundles, irregular, homogeneous, light brown clumps lie free in the tissue. The altered dermal connective tissue does not stain with silver nitrate as melanin does but becomes black when stained with cresyl violet or methylene blue . In addition, ochronotic pigment can be found within elastic fibers . In nodular ochronosis, a granulomatous response surrounds this material . Transfollicular elimination of ochronotic fibers may occur in patients with severe disease .
|
|
In pseudo-ochronosis, features similar to ochronosis are present in the form of prominent collagen bundles that
|
|
are yellow-brown in color. In addition, most cases have shown "ellipsoid black globules" of silver within the dermis .
|
|
Pathogenesis. In endogenous ochronosis, because of an inborn lack of homogentisic acid oxidase, the two amino acids tyrosine and phenylalanine cannot be catabolized beyond homogentisic acid. Most of the homogentisic acid is excreted in the urine. The urine, on standing or after the addition of sodium hydroxide, turns black (alkaptonuria) because, through oxidation and polymerization, homogentisic acid is converted into a dark-colored insoluble product. However, some of the homogentisic acid gradually accumulates in certain tissues. It is bound irreversibly to collagen fibers as a polymer after oxidation to benzoquinone-acetic acid .
|
|
In exogenous ochronosis, a topical agent such as hydroquinone, resorcinol, phenol, mercury, picric acid or benzene, or a systemic medication such as quinine or antimalarials inhibits the activity of homogentisic acid oxidase in the skin, resulting in the local accumulation of homogentisic acid, which polymerizes to form ochronotic pigment . In effect, this process mimics the cutaneous manifestation of endogenous ochronosis .
Pseudo-ochronosis appears to be due to deposits of traumatically implanted silver onto collagen bundles .
|
|
On electron microscopic examination of early lesions, deposition of amorphous, electron-dense ochronotic pigment around individual collagen fibrils within collagen fibers is observed . This causes the collagen fibrils to lose their periodicity and to degenerate. Gradually, the collagen fibrils disappear as they are replaced by ochronotic pigment. Ultimately, the ochronotic pigment occupies entire collagen fibers and, by fusion, entire collagen bundles . Cross-sections of the bundles then reveal a large, homogeneous, electron-dense aggregate that in some instances shows remnants of collagen fibrils at its periphery as well as macrophages containing particles of ochronotic pigment . Particles of ochronotic pigment can also be found in elastic fibers . In pseudo-ochronosis, scanning electron microscopy demonstrates silver deposited on collagen fibers .
|
|
|
|
|