
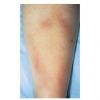
ERYTHEMA MIGRANS
Clinical Features.
In early case reports, EM lesions were reported in 50 percent to 80 percent of patients with Lyme disease. More recent studies have shown lower rates of EM, likely due to improved patient education. Definite history of tick bite at the site of the lesion is obtained in only a small proportion of patients. The lesion itself is believed to be the result of the direct presence of the spirochete, corroborated by reports showing aspiration and cultivation of the organism from the lesion. EM lesions develop within 3 to 30 days of the tick bite (median, 7 days).
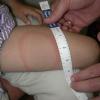
EM may be seen anywhere on the body but is most common on the lower extremities, inguinal and axillary regions of adults and on the face in children (“slapped cheek” appearance) reflecting sites of predilection of the tick. Although no definite sex predilection has been noted in the United States, women are reported to be more commonly affected in European studies.
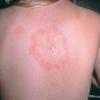
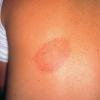
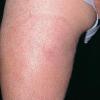
The skin lesion has a characteristic and pathognomonic appearance) of an expanding erythema encircling
the bite site, with the transition between the central zone and periphery being less well demarcated than between that of the periphery and adjacent skin. The border is usually confluent and not patchy. Cases in which the erythema appears stationary or even linear are reported. Typically described as round, the lesion in reality is more oval with the “long line of the oval parallel to the lines of least skin tension” (Langer lines) As migration of the lesion proceeds, distortion of this configuration occurs. The center fades after a few weeks leaving only the annular border erythematous . In very large lesions, only a portion of the erythematous border can be seen Uncommon presentations include the entire lesion being homogenously erythematous (“solidly erythematous”) (10 percent), forms with marked central necrosis, minimal size EM (size of the ring less than 5 cm at initial presentation) (2 percent), and the vesicular variant (5 percent).
The lesion in itself is usually asymptomatic, but 50 percent of patients report mild tingling or itching. Systemic manifestations, reported in approximately 50 percent of patients, may appear before, during, or after the classic rash.
EM has an excellent prognosis, attributable in part to the activation of pro-inflammatory cytokines such as interferon-γ. EM usually heals spontaneously, but may persist for as long as 6 to 12 months; median duration of the rash in the United States is approximately 4 weeks and in Europe is approximately 10 weeks.
Multiple EM-like lesions occur in between 1 percent and 17 percent of patients. The reported prevalence of multiple lesions is believed to be higher in the United States (25 percent to 48 percent) than in Europe (8 percent or less). The spatial relationship of multiple lesions to the initial lesion indicates that they may be the consequence of hematogenous dissemination. Secondary EM lesions number from 2 to more than 80, usually occur away from the original lesion, and are usually smaller and less migratory (occur in “crops” of similar size, color, and shape) in comparison to classic EM. Lesions are usually asymptomatic and if untreated spontaneously resolve over weeks to months. Like the primary lesion, secondary EM expands over days to weeks resulting in both solid and annular erythema. Primary EM may still may be present but more often a primary lesion is not found. Constitutional symptoms are usually more severe than those associated with classic EM.
Histopathologic Features.
Histopathologic findings vary with the biopsy site and age of the lesion. Biopsies of early lesions show papillary dermal edema and a mixed infiltrate of lymphocytes, neutrophils, a few plasma cells, and a few eosinophils . Biopsies of older lesions display a variably dense perivascular and interstitial infiltrate of lymphocytes and plasma cells . Helpful, albeit non-specific, clues include the presence of plasma cells and mast cells in the infiltrate. The presence of plasma cells and eosinophils in the same specimen is reported to be much less common than the presence of either alone.
Immunohistochemical studies indicate the infiltrate to be composed of CD4+ T
lymphocytes with the exception of those seen in association with HIV infection in which the infiltrate is mainly CD8+ T lymphocytes, reflective of the CD4 lymphopenia of HIV
infection.
Histopathologic features of multiple lesions of EM are identical to primary EM.
Diagnosis.
The diagnosis of EM is typically made on clinical appearance in patients in an endemic area. From biopsy specimens, spirochetes are best located in the papillary dermis and may be short or elongate at this stage of the disease . Direct detection of the spirochete from biopsy specimens by culture or by polymerase chain reaction (PCR) typically has good sensitivity but is usually unnecessary.
Diagnosis and Differential Diagnosis.
Atypical lesions exist and broaden the clinical differential diagnosis to include cellulitis, tinea, contact dermatitis, or a fixed drug reaction . The differential diagnosis of vesicular EM includes poison ivy, contact dermatitis, cellulitis, herpes simplex, and impetigo.

