






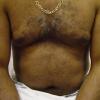
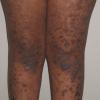
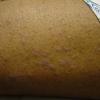
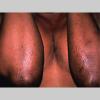
Lichen planus
Lichen planus (LP) is a pruritic, papular eruption characterized by its violaceous color; polygonal shape; and, sometimes, fine scale. Lichen planus is most commonly found on the flexor surfaces of the upper extremities, on the genitalia, and on the mucous membranes. Lichen planus is most likely an immunologically mediated reaction. See Oral Lichen Planus for more information on this variant of lichen planus.
Pathophysiology
Lichen planus is a cell-mediated immune response of unknown origin. Lichen planus may be found with other diseases of altered immunity; these conditions include ulcerative colitis, alopecia areata, vitiligo, dermatomyositis, morphea, lichen sclerosis, and myasthenia gravis.
An association is noted between lichen planus and hepatitis C virus infection,1,2,3,4 chronic active hepatitis, and primary biliary cirrhosis.5 In a meta-analysis, 16% of patients with lichen planus had hepatitis-C infection.2 The association of lichen planus and hepatitis C exists in all regions of the world, including North America.3 Hepatitis should be considered in patients with widespread or unusual presentations of lichen planus. Onset or exacerbation of lichen planus has been linked to stressful events.6
History
Most cases of lichen planus (LP) are insidious.
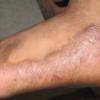
- The initial lichen planus lesion is usually located on the flexor surface of the limbs, such as the wrists . After a week or more, a generalized eruption develops with maximal spreading within 2-16 weeks
Pruritus is common in lichen planus but varies in severity depending on the type of lesion and the extent of involvement. Hypertrophic lesions are extremely pruritic.
Oral lesions may be asymptomatic or have a burning sensation, or they may even be painful if erosions are present.
In more than 50% of patients with cutaneous disease, the lesions resolve within 6 months, and 85% of cases subside within 18 months. On the other hand, oral lichen planus had been reported to have a mean duration of 5 years. Large, annular, hypertrophic lesions and mucous membrane involvement are more likely to become chronic.
Physical
In addition to the cutaneous eruption, lichen planus (LP) can involve the mucous membranes, the genitalia, the nails, and the scalp. The clinical presentation of lichen planus has several forms: actinic, annular, atrophic, erosive, follicular, hypertrophic, linear, pigmented, and vesicular/bullous. The papules are violaceous, shiny, and polygonal; varying in size from 1 mm to greater than 1 cm in diameter . They can be discrete or arranged in groups of lines or circles. Characteristic fine, white lines, called Wickham stria, are often found on the papules
Mucous membrane involvement is common and may be found without skin involvement. Lesions are most commonly found on the tongue and the buccal mucosa; they are characterized by white or gray streaks forming a linear or reticular pattern on a violaceous background . Oral lesions are classified as reticular, plaquelike, atrophic, papular, erosive, and bullous. Ulcerated oral lesions may have a higher incidence of malignant transformation in men, but this observation may be confounded by other factors, such as smoking and chewing tobacco. Lesions may also be found on the conjunctivae, the larynx, the esophagus, the tonsils, the bladder, the vulva, and the vaginal vault; throughout the gastrointestinal tract; and around the anus.
Genital involvement is common in men with cutaneous lichen planus. Typically, an annular configuration of papules is seen on the glans. Less commonly, linear white striae, similar to the lesions on the vulva and the vagina, can be seen on male genitalia. Vulvar involvement can range from reticulate papules to severe erosions. Dyspareunia, a burning sensation, and pruritus are common. Vulvar and urethral stenosis can also be present. Two reports documented that more than 50% women with oral lichen planus had undiagnosed vulvar lichen planus.10,
In 10% of lichen planus patients, ungual findings are present. Most commonly, nail plate thinning causes longitudinal grooving and ridging. Hyperpigmentation, subungual hyperkeratosis, onycholysis, and longitudinal melanonychia can result from lichen planus. Rarely, the matrix can be permanently destroyed with prominent pterygium formation. Lichen planus has been linked to childhood idiopathic nail atrophy and may overlap with twenty-nail dystrophy of childhood.
Lichen planus patients with a cutaneous eruption may also have follicular and perifollicular violaceous, scaly, pruritic papules on the scalp. These lesions can progress to atrophic cicatricial alopecia that can appear many weeks after the skin lesions have disappeared. Pseudopelade can be a final endpoint.
Variations in lichen planus include the following:
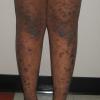
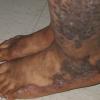
- Hypertrophic lichen planus: These extremely pruritic lesions are most often found on the extensor surfaces of the lower extremities, especially around the ankles. Hypertrophic lesions are often chronic; residual pigmentation and scarring can occur when the lesions eventually clear.
- Atrophic lichen planus: Atrophic lichen planus is characterized by a few lesions, which are often the resolution of annular or hypertrophic lesions.
- Erosive/ulcerative lichen planus: These lesions are found on the mucosal surfaces and evolve from sites of previous lichen planus involvement.
- Follicular lichen planus: Lichen planopilaris is characterized by keratotic papules that may coalesce into plaques. This condition is more common in women than in men, and ungual and erosive mucosal involvement is more likely to be present. A scarring alopecia may result.
- Annular lichen planus: Lichen planus papules that are purely annular are rare. Annular lesions with an atrophic center can be found on the buccal mucosa and the male genitalia.
- Linear lichen planus: Isolated linear lesions may form a zosteriform lesion, or they may develop as a Köbner effect.
- Vesicular and bullous lichen planus: Most commonly, these lesions develop on the lower limbs or in the mouth from preexisting lichen planus lesions. A rare condition, lichen planus pemphigoides, is a combination of both lichen planus and bullous pemphigoid.
- Actinic lichen planus: Subtropic or actinic lichen planus occurs in regions, such as Africa, the Middle East, and India. This mildly pruritic eruption usually spares the nails, the scalp, the mucous membranes, and covered areas. Lesions are characterized by nummular patches with a hypopigmented zone surrounding a hyperpigmented center.
- Lichen planus pigmentosus: This is a rare variant of lichen planus but can be more common in persons with darker-pigmented skin, such as Latinos or Asians. It usually appears on face and neck. Some believe it is similar to or the same as erythema dyschromicum perstans (ie, ashy dermatosis).
- Lichen planus pemphigoides: This is a rare form of lichen planus. Blisters subsequently develop on lichen planus lesions. Clinically, histopathologically and immunopathologically, it has features of lichen planus and bullous pemphigoid, it but carries a better prognosis than pemphigoid.
Causes
The exact cause of lichen planus (LP) is not known. The pathogenesis of lichen planus is immunologically mediated. Whether the foreign antigen is a virus or a drug is not known. Langerhans cells process antigens, which are then presented to T lymphocytes. This stimulated lymphocytic infiltrate is epidermotropic and attacks keratinocytes. During this lymphocytotoxic process, the keratinocytes release cytokines that attract more lymphocytes. This process has been referred to as the lichenoid tissue reaction. In addition, recent studies reveal a disruption in the epithelial anchoring system.
Some patients with lichen planus have a positive family history. It has been noted that affected families have an increased frequency of human leukocyte antigen B7 (HLA-B7). Others have found an association between idiopathic lichen planus and human leukocyte antigen DR1 (HLA-DR1) and human leukocyte antigen DR10 (HLA-DR10); thus, lichen planus may be influenced by a genetic predisposition.
Laboratory Studies
Direct immunofluorescence study in lichen planus (LP) reveals globular deposits of immunoglobulin M (IgM) and complement mixed with apoptotic keratinocytes.
Imaging Studies
No imaging studies are necessary for lichen planus.
Histologic Findings
The histopathologic features distinguish lichen planus based on the presence of irregular acanthosis and colloid bodies in the epidermis with destruction of the basal layer. The upper dermis has a bandlike infiltrate of lymphocytes and histiocytes.
The inflammatory reaction pattern is characteristic. The epidermis is hyperkeratotic with irregular acanthosis and focal thickening in the granular layer. Degenerative keratinocytes, known as colloid or Civatte bodies, are found in the lower epidermis. In addition to apoptotic keratinocytes, colloid bodies are composed of globular deposits of IgM (occasionally immunoglobulin G [IgG] or immunoglobulin A [IgA]) and complement. Linear or shaggy deposits of fibrin and fibrinogen are noted in the basement membrane zone.
The upper dermis has a bandlike infiltrate of lymphocytic (primarily helper T) and histiocytic cells with many Langerhans cells. The infiltrate is very close to the epidermis and often disrupts the dermal-epidermal junction
Medical Care
Lichen planus (LP) is a self-limited disease that usually resolves within 8-12 months. Mild cases can be treated with fluorinated topical steroids. More severe cases, especially those with scalp, nail, and mucous membrane involvement, may need more intensive therapy.
Consultations
Consult a dermatologist.
Medication
The first-line treatments of cutaneous lichen planus (LP) are topical steroids, particularly class I or II ointments. A second choice would be systemic steroids for symptom control and possibly more rapid resolution. Many practitioners prefer intramuscular triamcinolone 40-80 mg every 6-8 weeks. Oral acitretin has been shown to be effective in published studies.13 Many other treatments, including mycophenolate mofetil (CellCept) at 1-1.5 g twice daily, are of uncertain efficacy because of the lack of randomized controlled trials. In a randomized double-blinded study, sulfasalazine at up to 2.5 g/d for 6 weeks showed improvement in lesions (>80%) and pruritus (>90%) in patients with generalized lichen planus.14
For lichen planus of the oral mucosa, topical steroids are usually tried first. Topical and systemic cyclosporin have been tried with some success15 ; however, a randomized double-blind study indicated that topical cyclosporin was a less effective but much more costly regimen than clobetasol.16 Newer topical calcineurin inhibitors have replaced topical cyclosporin for the treatment of lichen planus. Other options include oral or topical retinoids. Even with these effective treatments, relapses are common.
Patients with widespread lichen planus may respond to narrow-band or broadband UV-B therapy.17 Psoralen with UV-A (PUVA) therapy for 8 weeks has been reported to be effective. Risks and benefits of this treatment should be considered. PUVA is carcinogenic. Long-term risks include dose-related actinic degeneration, squamous cell carcinoma, and cataracts. A phototoxic reaction with erythema, pruritus, phytophotodermatitis, and friction blisters could occur.
UV-A therapy combined with oral psoralen consists of oral psoralen (0.6 mg/kg), 1.5-2 hours before ultraviolet light, which usually starts at 0.5-1 J/cm2 and is increased by 0.5 J/cm2 per visit. Use of topical ointment at the time of receiving UV-A treatment may decrease the effectiveness of PUVA. Precaution should be taken for persons with a history of skin cancers or hepatic insufficiency.
Corticosteroids
These agents have anti-inflammatory properties and cause profound and varied metabolic effects. In addition, these agents modify the body's immune response to diverse stimuli. Topical steroids may be as effective as systemic steroids. Class I or II steroids in ointment form reduce pruritus in cutaneous lichen planus, but they have not been proven to induce remission.
Prednisone (Deltasone, Sterapred, Orasone)
May decrease inflammation by reversing increased capillary permeability and suppressing PMN activity.
Use with extreme caution in children. Pediatric dose is determined more by severity of condition than by age or weight.
Adult
30-60 mg/d PO for 4-6 wk followed by gradual taper
Pediatric
4-5 mg/m2/d PO; alternatively, 0.05-2 mg/kg PO divided bid/qid; taper over 2 wk as symptoms resolve
Coadministration with estrogens may decrease clearance; when used with digoxin, digitalis toxicity secondary to hypokalemia may increase; phenobarbital, phenytoin, and rifampin may increase the metabolism of glucocorticoids (consider increasing maintenance dose); monitor for hypokalemia with coadministration of diuretics; coadministration with ritonavir may significantly increase serum concentrations of prednisone; concomitant therapy with montelukast may result in severe peripheral edema; clarithromycin may increase risk of psychotic symptoms
Postmarketing surveillance reports indicate that risk of tendon rupture may be increased in patients receiving concomitant fluoroquinolones and corticosteroids, especially elderly patients; administration of asparaginase concurrently with or before prednisone therapy may result in increased toxicity
Documented hypersensitivity; viral, fungal, tubercular skin, or connective tissue infections; peptic ulcer disease; hepatic dysfunction
Pregnancy
B - Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
May unmask hypertension or diabetes or exacerbate peptic ulcer disease and tuberculosis; long-term sequelae associated with long-term steroid use include osteoporosis, cataracts, and pituitary-hypothalamic axis suppression; with high doses, patients may develop a steroid psychosis and are at increased risk of infections, particularly when oral steroids are used in conjunction with other immunosuppressants; frequently monitor patient's blood glucose level, blood pressure, and weight; monitor for Cushing syndrome; oral candidiasis may develop in patients treated for oral erosive LP
Betamethasone topical (Diprolene, Betatrex)
For inflammatory dermatosis responsive to steroids. Decreases inflammation by suppressing migration of polymorphonuclear leukocytes and reversing capillary permeability. Use in pediatrics with extreme caution. Children have a larger skin surface area to body weight ratio and less developed, thinner skin, which may result in greater amounts of topical steroid being absorbed compared with adults. Use nonfluorinated topical corticosteroids.
Adult
Oral LP: Apply gel to affected area q4-6h for 2-3 mo
Pediatric
Apply as in adults
Documented hypersensitivity; paronychia; cellulitis; impetigo; angular cheilitis; erythrasma; erysipelas; rosacea; perioral dermatitis; acne
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
If treating large areas, systemic absorption may occur and produce reversible HPA-axis suppression with potential for glucocorticoid insufficiency after withdrawal of treatment; do not use in skin with decreased circulation; can cause atrophy of groin, face, and axillae; if infection develops and is not responsive to antibiotic treatment, discontinue until infection is under control
Triamcinolone (Aristocort)
For inflammatory dermatosis responsive to steroids. Decreases inflammation by suppressing migration of polymorphonuclear leukocytes and reversing capillary permeability. Local injections have been reported to be effective.
Adult
Hypertrophic lesions: 5 mg/mL (10 mg/mL formulation) injected into posterior nail fold q2-4wk for 3 treatments may improve ungual lesions; oral lesions can also be treated with intralesional injection of 5-10 mg/mL
Pediatric
2.5-15 mg (10 mg/mL or 40 mg/mL formulations intralesionally); repeat prn
Documented hypersensitivity; fungal, viral, and bacterial skin infections; hypertension; ocular herpes simplex (risk of corneal perforation); scleroderma; recent surgery; infection at treatment site
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
May cause skin atrophy and hypopigmentation; do not use in decreased skin circulation; prolonged use, applying over large areas, and using potent steroids and occlusive dressings may result in systemic absorption; systemic absorption may cause Cushing syndrome, reversible HPA-axis suppression, hyperglycemia, and glycosuria
Halobetasol (Ultravate) ointment, cream
For inflammatory dermatosis responsive to steroids. Decreases inflammation by suppressing migration of polymorphonuclear leukocytes and reversing capillary permeability. Use in pediatrics with extreme caution. Children have a larger ratio of skin surface area to body weight and less developed, thinner skin, which may result in greater amounts of topical steroid being absorbed compared with adults. Use nonfluorinated topical corticosteroids.
Adult
Apply to affected areas bid
Pediatric
Not recommended
Documented hypersensitivity; paronychia; cellulitis; impetigo; angular cheilitis; erythrasma; erysipelas; rosacea; perioral dermatitis; acne
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
If treating large areas, systemic absorption may occur and produce reversible HPA-axis suppression with potential for glucocorticoid insufficiency after withdrawal of treatment; do not use in skin with decreased circulation; can cause atrophy of groin, face, and axillae; if infection develops and is not responsive to antibiotic treatment, discontinue until infection is under control
Retinoids
These agents modulate cell proliferation.
Isotretinoin (Amnesteem, Roaccutane)
Oral agent that treats serious dermatologic conditions. Synthetic 13-cis isomer of the naturally occurring tretinoin (trans- retinoic acid). Both agents are structurally related to vitamin A. Decreases sebaceous gland size and sebum production. May inhibit sebaceous gland differentiation and abnormal keratinization.
Adult
40 mg/d PO for several mo
Pediatric
Not established
Toxicity may occur with vitamin A coadministration; pseudotumor cerebri or papilledema may occur when coadministered with tetracyclines; may reduce plasma levels of carbamazepine
Increases toxicity of methotrexate (avoid concomitant use); interferes with effects of microdose progestin minipill; coadministration with alcohol may result in formation of etretinate, which has much longer half-life than acitretin (>120 d); may increase toxicity of phenytoin
Documented hypersensitivity
Pregnancy
X - Contraindicated; benefit does not outweigh risk
Precautions
May decrease night vision; inflammatory bowel disease may occur; may be associated with development of hepatitis and pancreatitis; diabetes patients may experience problems in controlling blood glucose while on isotretinoin; avoid exposure to UV light or sunlight until tolerance achieved; discontinue treatment if rectal bleeding, abdominal pain, or severe diarrhea occurs; mood swings or depression may occur; caution in history of depression
Tretinoin topical (Retin-A, Avita, Renova, Atralin)
May be effective for oral LP but not for cutaneous disease. Inhibits microcomedo formation and eliminates existing lesions. Makes keratinocytes in sebaceous follicles less adherent and easier to remove. Available as 0.025%, 0.05%, and 0.1% creams. Also available as 0.01% and 0.025% gels.
Adult
Apply to affected area of mouth bid; begin with lowest tretinoin formulation and increase as tolerated; apply hs or qod; lower frequency of application if irritation develops
Pediatric
<12 years: Not established
>12 years: Apply as in adults
Other skin irritants (ie, astringents, benzoyl peroxide, salicylic acid, resorcinol, topical sulfur, other keratolytics, abrasives, astringents, spices, lime) may exacerbate irritation; coadministration with other drugs causing photosensitivity (eg, tetracycline, sulfonamides) may increase risk of sunburn
Documented hypersensitivity
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Photosensitivity may occur with excessive sunlight exposure; burning, stinging, peeling, pruritus, or erythema has been reported at site of application; caution with eczema (may cause severe irritation); avoid contact with mucous membranes, mouth, and angles of nose
Acitretin (Soriatane)
Retinoic acid analog, like etretinate and isotretinoin. Etretinate is main metabolite and has demonstrated clinical effects close to those seen with etretinate. Mechanism of action is unknown.
Adult
30 mg/d PO for 8 wk
Pediatric
Not established
Increases toxicity of methotrexate (avoid concomitant use); interferes with effects of microdosed progestin minipill; coadministration with alcohol may enhance synthesis of etretinate, which has much longer half-life than acitretin (>120 d); topical drying or peeling agents; tetracyclines or photosensitizing medications
Documented hypersensitivity; pregnancy
Pregnancy
X - Contraindicated; benefit does not outweigh risk
Precautions
Most common adverse effects include cheilitis and dry mouth; hair loss, xerosis, hypertriglyceridemia, and impaired wound healing may occur; for women, a contraceptive period of 3 y after last intake of acitretin is recommended; do not use in severe obesity; women of childbearing age must be capable of complying with effective contraceptive measures; perform AST, ALT, and LDH tests prior to initiation of acitretin therapy at 1- to 2-wk intervals until stable and thereafter at intervals as clinically indicated
Immunosuppressants
These agents modulate the immune system.
Cyclosporine (Sandimmune, Neoral)
Topical treatment under occlusion has been efficacious for genital lesions and may be beneficial in hypertrophic lesions. Mouthwash or oil-based solutions have been effective for oral LP but seem to be no better than corticosteroids. Systemic treatment has been used for severe resistant cutaneous disease, oral or ulcerative foot involvement, and lichen planopilaris of the scalp.
Pediatric population may require higher or more frequent dosing because of accelerated clearance; use with extreme caution.
Adult
1-2 mg/kg/d PO recommended starting dose; if no response, increase dose; usual dose is 5 mg/kg/d
Pediatric
Administer as in adults


