|
Culicosis bullosa =داء لدغ البعوض الفقاعي |
 |
 |
 |
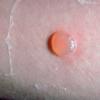 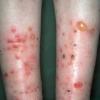 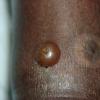 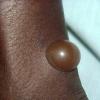 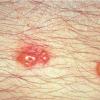 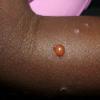 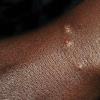 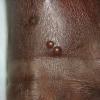  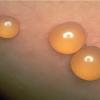
Insect Bites
Insects are arthropods of the class Insecta. Insects have an adult stage characterized by a hard exoskeleton, 3 pairs of jointed legs, and a body segmented into head, thorax, and abdomen. Insects comprise the most diverse and numerous class of the animal kingdom and include numerous species of praying mantis, dragonflies, grasshoppers, true bugs, flies, fleas, bees, wasps, ants, lice, butterflies, moths, and beetles. The number of species is estimated at between 6 and 10 million, with more than a million species already described. Insects represent more than half of all known living organisms and potentially represent more than 90% of the differing life forms on Earth. Hence, human contact with insects is unavoidable. Exposure to biting or stinging insects or to their remains can range in severity from benign or barely noticeable to life threatening.
A stinging apparatus is usually a sharp organ of offense or defense, especially when connected with a venom gland, and adapted to inflict a wound by piercing, as the caudal sting of a scorpion. The stinger is typically located at the rear of the animal. Animals with a stinger include bees, wasps, hornets, and scorpions. Most stinging insects are of the order Hymenoptera, which includes ants, bees, and wasps. Hymenoptera stings result in more fatalities than stings or bites from any other arthropod. Wasps can bite and sting at the same time (See Wasp Stings).
Since their introduction into the southern United States in the 1920s, imported fire ants anchor themselves with their mandibles and subsequently inflict a sting. Fire ants often pivot or re-anchor themselves only to sting again and again resulting in a sensation of fire at the site. When fire ants swarm, they often position themselves on their victim and sting simultaneously in response to an alarm pheromone released by one or several individuals. Immobilized or elderly patients can become rapidly covered by swarms of these ants, resulting in severe stings and even death (See Fire Ant Bites).
Bites by classes Insecta
This article is limited to bites by insects and not arachnids. Stings by members of the order Hymenoptera and order Scorpionida are discussed in other articles, as are bites of venomous arachnids in the class Arachnida (spiders) and bites of the order Acarina (mites and ticks).
Injuries from exposure to millipedes (class Diplopoda), centipedes (class Chilopoda), and caterpillars (order Lepidoptera) also are discussed in other articles (see Differentials); however, many of the principles that guide diagnosis and treatment of insect bites also apply to bites and stings of these other organisms.
Exotic insects
While illness related to insect exposure in a particular locale may be easily recognizable, the emergency physician must also be aware of more exotic insect-related diseases as humans travel to more remote areas of the country and the world. Additionally, exotic insects are often kept as pets (sometimes illegally) or can be encountered in shipments of foreign origin.
Anaphylactic shock
Anaphylactic shock is the most notable immediate risk associated with insect exposures. Hypersensitivity to otherwise harmless insect saliva, venom, body parts, excretions, or secretions can cause systemic responses in some individuals. Diagnosing the early phases of a systemic allergic reaction preceding anaphylactic shock is of paramount importance in treating any patient in whom insect exposure is suspected. Severe anaphylaxis can be fatal in as little as 10 minutes.
The reoccurrence rate is 40-60% for insect stings. Hence, the patient should be instructed on how to avoid future exposure to the causative agent, if possible. A prescription and clear instructions on the use of an epinephrine autoinjector should be provided to patients when the risk of another reaction is judged to be substantial.1
Diseases transmitted by insect bites
The need to be aware of diseases transmitted by insect bites is crucial; Lyme disease, transmitted by ticks, and malaria, transmitted by mosquitoes, are discussed in other articles (see Tick-borne Diseases, Lyme; Malaria).
Chagas disease, increasingly found in the desert southwest and in persons residing in or traveling to Central America or South America, should be considered, particularly when the bite site is on the soft skin of the periorbita or lips.2 Because this infection may produce an acute and chronic illness with notable morbidity and mortality, especially in pediatric patients, clinicians should maintain a high index of suspicion (see Trypanosomiasis).
Mosquito and tick-borne encephalitides such as those produced by the eastern equine virus or the West Nile virus also should be considered in patients presenting with meningismus (see Encephalitis).
Of note, some illnesses transmitted by insects do not produce symptoms until long after the infecting bite. In South America and parts of Africa, blackflies (Simuliidae) are responsible for transmission of onchocerciasis. This illness is also known as river blindness and eventually can produce blindness years after the initial infection. This disease is extremely rare in the United States. Chagas disease, a leading cause of cardiomyopathy in the world, may present latently as well. Obtaining a history of international travel is important because this information can lead to a diagnosis that would otherwise be overlooked. Determining the destination, time of year, length of stay, and time since travel are all important pieces of history to obtain.
Exposure to arthropods may produce dermatitis, cellulitis, urticaria, or blistering unrelated to biting or stinging. Some species of moths, caterpillars, centipedes, beetles, and spiders have urticating hairs or secretions that can cause cutaneous irritation. For further information, please refer to the respective articles on these exposures (see Differentials).
An uncommon occurrence in North America is myiasis by fly larvae. Fly larvae enter the host through varying mechanisms ranging from oviposition of live, burrowing larvae on the host, on or near open wounds, to attachment to other bloodsucking insects. While not generally the result of an insect bite, myiasis can produce pustules and lesions similar to insect bites. These lesions generally contain one or more developing fly larvae. Severe cases of myiasis can cause seizures.
While plant-eating phytophagous insects can bite in self-defense, their bites generally are not purposeful. This article is limited to discussion of organisms that bite to feed on blood or to catch prey.
Relatively harmless insects
Cockroaches have been reported to bite humans, but their bite generally is harmless. Continued repeated exposure to their remains and feces poses a greater health threat, such as increased incidence of asthma, especially in inner cities, and their remains and feces are possible vectors for transmission of viral and bacterial diseases.
Earwigs generally are harmless insects that have earned an unpleasant reputation. This may be because of their depiction in popular culture, such as in the television series, "The Night Gallery." Although they appear to have a large pincer on the posterior abdomen, it is not capable of rendering anything more serious than a mild pinch. Additionally, and contrary to popular belief, they do not routinely enter the human ear canal and parasitize humans. Cockroaches are much more likely to be found lodged in a patient's auditory passage.
Pathophysiology
Mouthparts of biting insects can be classified into 3 broad groups: piercing, sponging, and biting. Tremendous diversity exists in the morphology of these groups. Insects discussed in this article generally are nonvenomous, yet many species inject saliva while biting. Their saliva may aid in digestion, inhibit coagulation, increase blood flow to the bite, or anesthetize the bite locus. Most lesions are the result of the victim's immune response to these insect secretions. In the case of Chagas disease, the infective organism is transmitted via the feces of a reduviid bug, which enters through the bite site when the wound becomes pruritic and is scratched. Most insect bites are minor and can result in superficial puncture wounds to the skin. Horseflies feed with a large scissorlike proboscis that can cause a relatively deep and painful wound.
Differentiating between insect bites and stings
Many patients confuse an insect bite with a sting and may use the terms interchangeably. A bite is usually from mouth parts and occurs when an insect is agitated to defend itself or when an insect seeks to feed. Bites from mosquitoes, fleas, bed bugs, and mites are more likely to cause itching than pain.
Most patients are aware of insect bites when they occur or shortly thereafter, but because it is such a common occurrence, the exposure is typically dismissed unless a severe or systemic reaction occurs.
- Reactions to bites may be delayed due to the host being asleep or because the saliva of some micropredators may contain an anesthetic secreted to allow uninterrupted blood-feeding.
- Patients who present with a history of homelessness or of staying in homeless shelters may have an exposure to organisms such as bedbugs.5,6,7 Alternatively, patients with impairment from mental illness may also be susceptible to infestation with insect parasites.
- Exposure to feral animals or even to domesticated animals, such as livestock or house pets, may predispose patients to exposure to biting insects such as fleas, bedbugs,8,6,7 or lice.
- Types of reactions
- In a local reaction, the patient may complain of discomfort, itching, moderate or severe pain, erythema, tenderness, warmth, and edema of tissues surrounding the site. Although it may involve neighboring joints, local reactions cause no systemic symptoms.
- In a severe local reaction, complaints include generalized erythema, urticaria, and pruritic edema. Severe local reactions increase the likelihood of serious systemic reactions if the patient is exposed again at a later time.
- In a systemic or anaphylactic reaction, the patient may complain of localized symptoms as well as symptoms not contiguous with the bite location. Symptoms can range from mild to fatal. Early complaints typically include generalized rash, urticaria, pruritus, and angioedema. These symptoms may progress, and the patient may develop anxiety, disorientation, weakness, gastrointestinal disturbances (eg, cramping, diarrhea, vomiting), uterine cramping in women, urinary or fecal incontinence, dizziness, syncope, hypotension, stridor, dyspnea, or cough. As the reaction progresses, patients may experience respiratory failure and cardiovascular collapse.
- Delayed reactions may appear 10-14 days after a sting. Symptoms of delayed reactions resemble serum sickness and include fever, malaise, headache, urticaria, lymphadenopathy, and polyarthritis.
Physical
- Without a clear patient history, diagnosis of an insect bite can be difficult since the initial response may be limited to erythema, local pain, pruritus, or edema.
- Wheals and urticaria are common initial signs and generally appear within a few minutes of the bite. Unfortunately, many dermatologic conditions also produce similar cutaneous signs and may confound the diagnosis.
- Identification of the insect responsible for the bite may be possible by examining the location, number, pattern, and sequelae of the bite(s).
Physical examination elements indicating a systemic reaction include the following:
- Cardiovascular - Hypotension, orthostasis
- Cutaneous - Urticaria, wheals, angioedema, blood at bite site, pruritus
- Respiratory - Tachypnea, stridor, wheezing, bronchospasm
- Gastrointestinal - Hyperactive bowel sounds
- Laboratory studies are seldom necessary. Appropriate laboratory studies should be ordered if the patient is compromised severely and requires hospital admission or end-organ failure is suspected, or for evaluation of secondary complications such as cellulitis.
- Biopsy of lesions generally is nondeterminant and is impractical in the ED.
- Microscopic examination of skin scrapings can be useful in the diagnosis of scabies or mite infestations but are not useful for most insect bites.
- Serology studies may be useful in determining infection due to an insect vector, but these are not available in the ED and may take weeks to obtain a result
Prehospital Care
- If the bee stinger is present in the wound, it should be removed. Although conventional teaching suggested scraping the stinger out to avoid squeezing remaining venom from the retained venom gland into the victim, involuntary muscle contraction of the gland continues after evisceration and the venom contents are quickly exhausted. Immediate removal is the important principle and the method of removal is irrelevant.
- Most insect bites may be treated acutely with a compress after routine wound cleaning with soap and water to minimize the possibility of infection.
- For a large local reaction, ice packs may minimize swelling. Apply ice for no more than 15 minutes at a time using a cloth barrier between ice and skin to prevent direct thermal injury to the skin.
- Epinephrine is the mainstay of prehospital treatment of a systemic reaction; the route of administration (subcutaneous, intramuscular, intravenous [IV], endotracheal) depends on the patient's condition and the expertise of the prehospital provider. Systemic antihistamines and corticosteroids, if available, help manage systemic reactions. Many patients who are allergic to stings carry commercially available bee sting kits containing an autoinjector of epinephrine. Refer to Hymenoptera Stings.
- Topical antihistamines should not be applied over large surface areas, and they should not be used concurrently with systemic H1 antihistamines. Systemic anticholinergic toxicity may result from misuse of these medications.
- Use of H2-blocking drugs (usually used to reduce gastric acid secretion) may be used concurrently with H1-blocking antihistamines.
- In many patients, transport to a hospital is not necessary. Those requiring transport include patients who develop signs or symptoms of a systemic response or individuals with a history of insect-related anaphylaxis. A phone call to the regional poison center may save a costly visit to the ED.
Emergency Department Care
- Endotracheal intubation and ventilatory support may be required for severe anaphylaxis or angioedema involving the airway.
- Treat emergent anaphylaxis in an atopic individual with an initial intramuscular injection of 0.3-0.5 mL of 1:1000 epinephrine. This may be repeated every 10 minutes as needed.
- A bolus of IV epinephrine (1:10,000) may be used cautiously in severe cases.
- Solution of 1:10,000 typically is found in 10-mL vials. Repeated 1-mL doses are a reasonable initial approach in a critically ill patient with anaphylaxis.
- Once a positive response is achieved, these boluses can be followed by a carefully monitored, continuous epinephrine infusion.
- Use extra care in monitoring formulation, concentration, and dose when administering IV epinephrine to avoid inadvertent overdose.
- Severely hypotensive patients may require a large volume of IV fluids. Monitor for angioedema and pulmonary edema.
- Antihistamines, both H1 and H2 blockers, are useful in treating systemic reactions. Corticosteroids also are indicated routinely in such patients.
- Refer to Anaphylaxis and Serum Sickness for further guidance.
- Ensure appropriate tetanus prophylaxis.
- Undefined erythema and swelling seen may be difficult to distinguish from cellulitis. As a general rule, infection is present in a minority of cases and antibiotic prophylaxis is not recommended.
- Related diagnostic and treatment guidelines are available on anaphylaxis, travel medicine, and referral guidelines (also see Further Reading).9,10,11
Consultations
- In cases in which determining the insect species is important, a health department, agriculture extension, or university entomologist may be useful.
- In cases of potential vector-borne disease transmission, an infectious disease specialist may be of help.
- If the potential infection is associated with travel to a tropical region, consider contacting a tropical medicine specialist or the Centers for Disease Control and Prevention (CDC) at 1-877-394-8747 (Traveler's Health Hotline).
- A regional poison center may be of assistance in difficult or complicated cases or for general information.
Medication
Goals of therapy are to treat anaphylaxis and prevent complications.
Cardiovascular agents
Act to decrease the muscle tone in the small and large pulmonary airways and increase vascular tone.
Epinephrine (Adrenalin, Bronitin, EpiPen)
Drug of choice for shock, angioedema, airway obstruction, bronchospasm, and urticaria in severe anaphylactic reactions. Administer IM; administer IV to patients in extremis; may be administered SL or ET when no IV access available. Continuous infusion may be given in cases of refractory shock.
Adult
1 mL 1:10,000 solution slow IV; repeat prn
0.1-1 mcg/kg/min IV infusion
0.3-0.5 mL 1:1000 solution IM/SL/SQ q10-15min
1 mL 1:1000 solution in 10 mL NS ET
Pediatric
0.01 mL/kg (min 0.1 mL) 1:10,000 solution IV prn
0.1-1 mcg/kg/min IV infusion
0.01 mL/kg (min 0.1 mL) 1:1000 solution IM/SL/SQ q15min
0.01 mL/kg (min 0.1 mL) 1:1000 solution in 1-3 mL NS ET
Epinephrine coadministered with other sympathomimetics may have additive effects; beta-blockers antagonize therapeutic effects of epinephrine; digitalis may potentiate proarrhythmic effects of epinephrine; TCAs and MAOIs potentiate cardiovascular effects of epinephrine; phenothiazines may decrease BP when coadministered with epinephrine
In a life-threatening anaphylactic reaction, epinephrine may be given with appropriate caution when any of the following relative contraindications are present: coronary artery disease; uncontrolled hypertension; serious ventricular dysrhythmias; second stage of labor
Pregnancy
B - Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
Caution in elderly patients and those with prostatic hypertrophy, hypertension, cardiovascular disease, diabetes mellitus, hyperthyroidism, and cerebrovascular insufficiency; rapid IV infusions may cause death from cerebrovascular hemorrhage or cardiac dysrhythmias
Bronchodilators
Through activation of cyclic AMP, beta agonists stimulate the ATPase pump, thereby shifting potassium into the intracellular compartment and stimulating an adrenergic response.
Albuterol (Ventolin)
Beta agonist useful in treating bronchospasms refractory to epinephrine. Relaxes bronchial smooth muscle by action on beta2 receptors and has little effect on cardiac muscle contractility. Numerous inhaled beta agonists are used for treatment of bronchospasm; albuterol is used most commonly.
Adult
0.5 mL 0.5% solution in 2.5 mL NS nebulized q15min
Pediatric
0.03-0.05 mL/kg 0.5% solution in 2.5 mL NS via nebulizer q15min
Increases toxicity of beta-blocking and alpha-blocking agents and halogenated inhalational anesthetics
May be given in a life-threatening anaphylactic reaction, even when the following relative contraindications are present: severe coronary insufficiency; uncontrolled severe hypertension
Pregnancy
B - Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
Caution in elderly patients and those with prostatic hypertrophy, hypertension, cardiovascular disease, diabetes mellitus, hyperthyroidism, and cerebrovascular insufficiency; rapid IV infusions may cause death from cerebrovascular hemorrhage or cardiac dysrhythmias
Antihistamines
Prevent histamine response in sensory nerve endings and blood vessels; more effective in preventing histamine response than in reversing it. H2 antihistamines are useful in treatment of anaphylactic reactions when used concomitantly with H1 antagonists. Many H2 blockers are available. Cimetidine is the prototype drug.
Diphenhydramine (Benadryl)
Used for symptomatic relief of allergic symptoms caused by histamines released in response to allergens; many effective H1 blockers; diphenhydramine is effective and widely available.
Adult
50 mg PO q4-6h
25-50 mg IV/IM q4-6h
Pediatric
5 mg/kg/d PO divided q6h-8h
Severe cases: 1-2 mg/kg IV q6h; alternatively, 1-2 mg/kg IM q6h
Potentiates effect of CNS depressants; due to alcohol content, do not give syr dosage form to patient taking medications that can cause disulfiramlike reactions
Documented hypersensitivity; MAOIs
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
May exacerbate angle-closure glaucoma, hyperthyroidism, peptic ulcer, and urinary tract obstruction
Cimetidine (Tagamet)
An H2 antagonist that, when combined with H1 type, may be useful to treat itching and flushing in anaphylaxis, pruritus, urticaria, and contact dermatitis that do not respond to H1 antagonists alone. Use in addition to H1 antihistamines.
Adult
300 mg PO/IV/IM q6h
Pediatric
5-10 mg/kg PO/IV/IM q6h
Can increase blood levels of theophylline, warfarin, TCAs, triamterene, phenytoin, quinidine, propranolol, metronidazole, procainamide, and lidocaine
Documented hypersensitivity
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Elderly patients may experience confusional states; may cause impotence and gynecomastia in young males; may increase levels of many drugs; adjust dose or discontinue treatment if changes in renal function occur
Corticosteroid, Systemic
Have anti-inflammatory properties and cause profound and varied metabolic effects. In addition, these agents modify the body's immune response to diverse stimuli. Prednisone and methylprednisolone are typical drugs of this class. Oral bioavailability is generally similar to parenteral; administer oral prednisone when indicated if a patient is not in extremis and can comfortably take PO; administer parenteral steroid when indicated for a patient in more severe circumstances.
Prednisone
Believed to ameliorate delayed effects of anaphylactic reactions and may limit biphasic anaphylaxis. Doses below are general guidelines for usage; dosing is highly individualized.
Adult
40-60 mg/d PO qd or divided bid/qid; no taper required if used for 5-7 d.
Pediatric
1-2 mg/kg PO qd or divided bid/qid; no taper required if used for 5-7 d.
Coadministration with estrogens may decrease clearance; concurrent use with digoxin may cause digitalis toxicity secondary to hypokalemia; phenobarbital, phenytoin, and rifampin may increase metabolism of glucocorticoids (consider increasing maintenance dose); monitor for hypokalemia with coadministration of diuretics
Documented hypersensitivity; viral infection, peptic ulcer disease, hepatic dysfunction, connective tissue infections, and fungal or tubercular skin infections; GI bleeding or ulceration
Pregnancy
B - Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
Abrupt discontinuation of glucocorticoids may cause adrenal crisis; hyperglycemia, edema, osteonecrosis, myopathy, peptic ulcer disease, hypokalemia, osteoporosis, euphoria, psychosis, myasthenia gravis, growth suppression, and infections may occur with glucocorticoid use
Methylprednisolone (Solu-Medrol, Depo-Medrol)
Useful to treat inflammatory and allergic reactions. By reversing increased capillary permeability and suppressing PMN activity, may decrease inflammation.
A multitude of corticosteroid preparations is available. Methylprednisolone is widely available in the ED due to other uses (ie, acute asthma, spinal cord injury) and is supplied in both parenteral and oral formulations.
Adult
2-60 mg PO qd
40-250 mg IV/IM q6h
Pediatric
1-2 mg/kg PO/IV/IM qd
NSAIDs may cause ulcers when taken concurrently; anticholinesterases may increase weakness in patients with myasthenia gravis when taken concurrently with steroids; risk exists of possible viral dissemination with live virus vaccines
Documented hypersensitivity; some evidence exists for fetal harm from corticosteroids (consider both benefits and risks of use during pregnancy); consider risks (eg, dissemination, activation, certain infections) when prescribing for immunosuppressed patients
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Short-term use of corticosteroids, even in large doses, has minimal harmful effects; long-term usage has multiple adverse effects; possible complications include hyperglycemia, edema, osteonecrosis, peptic ulcer disease, hypokalemia, osteoporosis, euphoria, psychosis, growth suppression, myopathy, or infections
Toxoids
For active immunity against tetanus.
Tetanus toxoid adsorbed or fluid
Used to induce active immunity against tetanus in selected patients. The immunizing agents of choice for most adults and children > 7 y are tetanus and diphtheria toxoids. Necessary to administer booster doses to maintain tetanus immunity throughout life.
Pregnant patients should receive only tetanus toxoid, not a diphtheria antigen-containing product.
In children and adults, may administer into deltoid or midlateral thigh muscles. In infants, preferred site of administration is mid thigh laterally.
Adult
Primary immunization: 0.5 mL IM; give 2 injections 4-8 wk apart and a third dose 6-12 mo after second injection
Booster dose: 0.5 mL q10y
Pediatric
Administer as in adults
Patients receiving immunosuppressants, including corticosteroids or radiation therapy, may remain susceptible despite immunization due to poor immune response; cimetidine may enhance or augment delayed-hypersensitivity responses to skin-test antigens; avoid concurrent use of medication with systemic chloramphenicol since it may impair amnestic response to tetanus toxoid; concurrent use of tetanus immune globulin may delay development of active immunity by several days (interaction is nevertheless clinically insignificant and does not preclude concurrent use)
Documented hypersensitivity; history of any type of neurologic symptoms or signs following administration of this product; FDA recommends that elective tetanus immunization be deferred during any outbreak of poliomyelitis because tetanus toxoid injections are an important cause of provocative poliomyelitis
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Do not use to treat actual tetanus infections or for immediate prophylaxis of unimmunized individuals (use instead tetanus antitoxin, preferably human tetanus immune globulin); diminished antibody response to active immunization may be seen in patients receiving immunosuppressive therapy; better to defer primary diphtheria immunization until immunosuppressive therapy discontinued; routine immunization of symptomatic and asymptomatic HIV-infected persons is recommended
Immunoglobulins
Consists of administration of immunoglobulins pooled from serum of immunized patients.
Tetanus immune globulin (TIG)
Used for passive immunization of any person with a wound that may be contaminated with tetanus spores.
Adult
Prophylaxis: 250-500 U IM in opposite extremity to tetanus toxoid lesion
Clinical tetanus: 3,000-10,000 U IM
Pediatric
For prophylaxis: 250 U IM in opposite extremity to tetanus toxoid
Clinical tetanus: 3,000-10,000 U IM
|
|
|
|


