Cow Pox
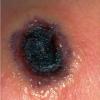
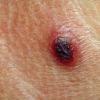
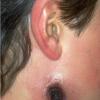
More than 200 years ago, in one of the first demonstrations of vaccination, Edward Jenner inoculated a young English boy with cowpox material from a dairymaid and showed that the boy became resistant to smallpox. Today, cowpox is a rare disease, largely confined to small mammals on the European continent and in Great Britain, with occasional transmission to humans. Most cases present with a small number of vesicopustular lesions on the hands or face that subsequently ulcerate and develop a black eschar before spontaneously resolving. Rarely, cutaneous dissemination and even death may occur.
Pathophysiology
Cowpox is caused by the cowpox or catpox virus, a member of the orthopoxvirus family, which also includes smallpox and vaccinia.1 The virus is believed to be acquired by direct contact with an infected animal, most often a cat in the case of humans, with lesions occurring where the virus gains access through broken skin.2 Infection generally remains localized at the initial site of inoculation, although lymphatic spread in a sporotrichoid pattern and generalized skin infection have been reported.3,4,5 Human-to-human transmission of cowpox has never been reported.
As a member of the Orthopoxvirus family, cowpox is a large double-stranded DNA virus that replicates in cell cytoplasm. Viral particles bind to plasma membrane receptors on host cells and then enter into the cytoplasm, where the viral genome is replicated and viral progeny are assembled. After new viral particles are assembled, the host cell lyses, releasing infectious virus, which can enter surrounding cells. Cowpox virus has no latent stage and does not integrate its DNA into the host genome.
Poxviruses use numerous strategies to evade the host immune system. These include production of homologues of mammalian tumor necrosis factor receptor, interleukin-1beta receptor, interleukin 18–binding protein, interferon-alpha/beta receptor, and interferon-gamma receptor, as well as a complement-binding protein and a caspase inhibitor.6 These proteins are thought to neutralize the host's antiviral response by binding to cytokines and complement proteins and inhibiting their function. In addition, cowpox virus has been shown to inhibit intracellular transport of major histocompatibility class I molecules, allowing it to evade cytotoxic T cells.7,8
History
- Generally, patients are young; 50% of patients are younger than 18 years.
- Most cases occur in late summer to fall.
- Cases present in endemic areas of Europe.
- Contact with rodents, cats, or cows is reported in 50% of cases.11,12,13,14,15 One case was reported in an animal keeper who was exposed to an infected circus elephant.16
- Usually, only 1 or a small number of lesions occur on the hands (48%) and face (33%).
- Patients may report having a flat red lesion that became raised and then blistered over a period of 2 weeks. The blister subsequently became crusted, with the surrounding skin becoming red and swollen. The lesions are characteristically described as quite painful.
- Patients may have eye complaints.
- Patients may report fever, malaise, lethargy, vomiting, and sore throat, which usually lasts 3-10 days but resolves during the eschar stage of cutaneous lesions.
Physical
- Physical findings generally are limited to the skin, eyes, and lymph nodes.
- Cutaneous findings develop as follows:
- Days 1-6 (after inoculation): An inflamed macule appears at the site of contact with the infected animal and at any secondary sites of accidental transfer.
- Days 7-12: The inflamed lesion becomes papular, then vesicular.
- Days 13-20: The vesicle becomes hemorrhagic, then pustular, and has a tendency to ulcerate, with surrounding edema and induration. Secondary lesions may form nearby.
- Weeks 3-6: The vesicopustule progresses to a deep-seated, hard, black eschar, often surrounded by edema, induration, and erythema. Most patients present at this stage, which may appear similar to cutaneous anthrax.17,18
- Weeks 6-12: The eschar sloughs, and the lesion heals, usually with scarring
- Rarely, the cutaneous lesions may become generalized before resolving.
- Ocular findings include conjunctivitis, periorbital edema, and corneal involvement.
- Enlarged painful local lymph nodes often are observed. Necrotizing lymphadenitis has been reported.19
Causes
The natural reservoir of cowpox virus is believed to be small woodland mammals, such as bank voles and wood mice, with humans, cows, and cats being only accidental hosts.
- Risk factors for infection with cowpox include exposure to potentially infected animals (eg, cats, cows, rodents) in an endemic area.
- Risk factors for dissemination of infection include atopic dermatitis and use of systemic corticosteroids
Laboratory Studies
- Electron microscopy of vesicle fluid or scab extracts is the most rapid and useful technique to aid in diagnosis. Orthopoxviruses, including cowpox, have characteristic "mulberry" and "capsule" forms that allow them to be differentiated from parapoxviruses and herpes viruses. Electron microscopy does not distinguish between cowpox, smallpox, vaccinia, and molluscum viruses, so clinical information is critical.
- Virus may be grown from lesional skin in cell culture and then studied by electron microscopy. Growth on chick chorioallantoic membrane produces characteristic hemorrhagic pocks.
- Polymerase chain reaction may be performed on biopsy material or cell culture extracts to amplify the cowpox A36R, thymidine kinase, or hemagglutinin gene and identify it by sequencing or restriction fragment length polymorphism analysis.20
- Serologic tests to detect antibodies to cowpox virus are not routinely available in hospital laboratories but may be performed in research laboratories. Previous vaccination with vaccinia may cause false-positive results, but these can be eliminated by the use of specific immunoglobulin M tests.
Procedures
Skin biopsy for routine histology, electron microscopy, culture, or molecular detection methods may be performed.
Histologic Findings
Using routine light microscopy, characteristic cytoplasmic inclusions have been observed in biopsies from feline cowpox but not in human material. Immunohistochemistry detects cowpox antigens in feline cases. Using electron microscopy, biopsy material may reveal viral particles.
Medical Care
- Because cowpox is generally a self-limited disease, treatment is largely supportive.
- Patients often do not feel well and require bed rest or, occasionally, hospitalization.
- Antiviral medications are not routinely used in cases of human cowpox, nor are antibiotics given unless the patient has developed a secondary bacterial infection. However, studies in mice suggest a role for the viral DNA polymerase inhibitor cidofovir, given parenterally, topically, or in an aerosolized form, for disseminated cases of cowpox.21,22
- Patients should be made aware that their lesions are potentially infectious, but no person-to-person transmission has been reported. Occlusive bandages may be applied to avoid this risk.
- In severe cases, antivaccinia gammaglobulin may be given.
Surgical Care
- Standard wound dressings may be applied to lesions.
- Draining of pus or removal of eschars may actually prolong infection or spread it to other body sites and is therefore not recommended.
Consultations
- Consult infectious disease and/or dermatology specialists for help in making a diagnosis and in differentiating it from parapoxvirus infections and other entities.
Medication
Because most cases of cowpox are mild and self-limited, no treatment is usually required. However, for severe cases with widespread involvement, cidofovir or antivaccinia gammaglobulin may be considered.23
Immune globulins
The rationale for using antivaccinia gammaglobulin is the presumed cross-reactivity of antibodies to all viruses of the orthopoxvirus family. Antibodies to vaccinia are known to be protective against smallpox and also may be protective against cowpox.
Vaccinia immune globulin intravenous
Recommended only for severe cases with widespread involvement. This medication and advice on its use may be obtained from the Centers for Disease Control and Prevention Drug Services (404-639-3670).
Dose information is based on use of gammaglobulin for cases of vaccinia.
Adult
0.6 mL (600 IU)/kg deep IM injection in divided doses over 24-36 h; repeat in 2-3 d if no improvement
Pediatric
<1 year: 2 mL (2000 IU) IM
1-6 years: 4 mL (4000 IU) IM
7-14 years: 6 mL (6000 IU) IM
>15 years: 8 mL (8000 IU) IM
Increases toxicity of live virus vaccine (MMR); do not administer within 3 mo of vaccine
Documented hypersensitivity
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Check serum IgA; infusions may increase serum viscosity and thromboembolic events; infusions may increase risk of migraine attacks, aseptic meningitis (10%), urticaria, pruritus, or petechiae (2-5 d postinfusion to 30 d); increases risk of renal tubular necrosis in elderly and in those with diabetes, volume depletion, and preexisting kidney disease; laboratory result changes associated with infusions include elevated antiviral or antibacterial antibody titers for 1 mo, 6-fold increase in ESR for 2-3 wk, and apparent hyponatremia
|
|
|
|


