
Chronic venous insufficiency
Chronic venous insufficiency (CVI) is a common condition affecting 2-5% of Americans. Historically, CVI was known as postphlebitic syndrome and postthrombotic syndrome, both of which refer to the etiology of most cases. However, these names have been abandoned because they fail to recognize another common cause of the disease, the congenital absence of venous valves.
In 1914, Homans postulated that the relative hypoxia of static venous blood decreases the amount of oxygen reaching the skin, causing skin changes and ulcers characteristic of CVI.1
In 1930, Landis et al demonstrated the direct relationship between venous hypertension in the legs and increased capillary intraluminal pressures.
In 1953, Piulacks et al theorized that arteriovenous fistulas in the skin of the lower extremities cause hypoxia, resulting in changes to the skin and tissues.2
In 1982, Burnand et al presented the fibrin cuff hypothesis, which describes the primary problem as venous hypertension in the lower extremities causing leakage of plasma proteins, particularly fibrinogen.3 A fibrin cuff encircles affected capillaries, decreasing oxygen diffusion to surrounding tissues.
In 1988, Coleridge-Smith et al described the white-cell trapping theory, which hypothesizes that venous hypertension and resultant increased capillary pressures trap white blood cells in the capillaries, where they become activated and damage capillary beds.4 Increased capillary permeability allows seepage of plasma proteins and fibrinogen into the interstitium, where a fibrin cuff forms, thus decreasing oxygen diffusion to surrounding tissues.
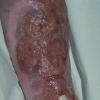
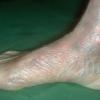
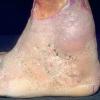
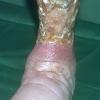
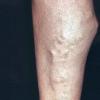
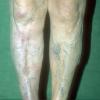
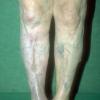
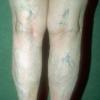
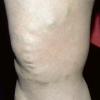
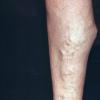
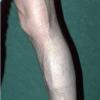
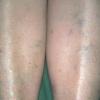
In addition to poor cosmesis, CVI can lead to chronic life-threatening infections of the lower extremities. Pain, especially after ambulating, is a hallmark of the disease. CVI causes characteristic changes, called lipodermatosclerosis, to the skin of the lower extremities, which lead to eventual skin ulceration
Risk factors associated with chronic venous insufficiency
- Age: Incidence of CVI rises substantially with age.
- Family history: History of deep vein thrombosis (DVT), which renders venous valves incompetent, causing backflow and increased venous pressure, is a risk factor.
- Lifestyle: A sedentary lifestyle minimizes the pump action of calf muscles on venous return, causing higher venous pressure. CVI occurs more frequently in women who are obese. Vocations that involve standing for long periods predispose individuals to increased venous pressure in dependent lower extremities. A higher incidence of CVI is observed in men who smoke.
-
Two major mechanisms in the body prevent venous hypertension. First, bicuspid valves in the veins prevent backflow and venous pooling. DVTs commonly occur at these valves, causing irreversible damage to the valve. Second, during normal ambulation, calf muscles decrease venous pressures by approximately 70% in the lower extremities. With rest, pressures return to normal in approximately 30 seconds. In diseased veins, ambulation decreases venous pressures by only 20%. When ambulation is stopped, pressure in the vein lumen increases slowly, returning to normal over a period of minutes,
Venous hypertension in diseased veins is thought to cause CVI by the following sequence of events. Increased venous pressure transcends the venules to the capillaries, impeding flow. Low-flow states within the capillaries cause leukocyte trapping. Trapped leukocytes release proteolytic enzymes and oxygen free radicals, which damage capillary basement membranes. Plasma proteins, such as fibrinogen, leak into the surrounding tissues, forming a fibrin cuff. Interstitial fibrin and resultant edema decrease oxygen delivery to the tissues, resulting in local hypoxia. Inflammation and tissue loss result.
Leg discomfort: Venous hypertension in muscles and fascial compartments of the lower leg from exercise and prolonged standing results in the characteristic ache of CVI. The discomfort is described as pain, pressure, burning, itching, dull ache, or heaviness in affected calves or legs.
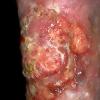
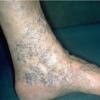
Nonhealing ulcers: Typically, these lesions occur around the medial malleolus, where venous pressure is maximal due to the presence of large perforating veins
Leg edema: Damage done to capillary basement membranes by white blood cells results in leg edema.
Lipodermatosclerosis: These characteristic skin changes in the lower extremities include capillary proliferation, fat necrosis, and fibrosis of skin and subcutaneous tissues. Skin becomes reddish or brown because of the deposition of hemosiderin from red blood cells
Surgical treatment is reserved for those with discomfort or ulcers refractory to medical management.
Indications for vein ligation: This technique is reserved for cases of CVI that include reflux in the saphenous system causing severe symptoms.10 For this reason, a diagnosis of reflux must be established preoperatively, usually with photoplethysmography or duplex imaging.
The venous network in the lower extremities commonly affected by CVI is divided into 3 systems. The first is superficial veins, which include the lesser and greater saphenous veins and their tributaries, as depicted in the 1st image below. The second is deep veins, which include the anterior tibial, posterior tibial, peroneal, popliteal, deep femoral, superficial femoral, and iliac veins. The third is perforating or communicating veins
Medical Therapy
Nonsurgical treatments for CVI include the following:
Leg elevation
By keeping the legs elevated, venous flow is augmented by gravity, lowering venous pressures and ameliorating edema. While sitting, the legs should be above the thighs. Supine, the legs should be above the level of the heart.
Compression stockings
First described by Jobst in 1940, compression stockings produce graded pressures from the foot to the knee or thigh to decrease edema and minimize venous hypertension. For two clinical studies of compression therapy, see Vanscheidt et al.11
Unna boots
First described by Unna in 1854, the Unna boot now is the mainstay of treatment for people with venous ulcers. Unna boots are rolled bandages that contain a combination of calamine lotion, glycerin, zinc oxide, and gelatin.
Injection sclerotherapy
Injection of sclerosing agent directly into veins usually is reserved for telangiectatic lesions rather than CVI.
Phlebotonics have not been proven to be beneficial for CVI.12
Surgical Therapy
Approximately 8% of patients require surgical intervention for CVI. Surgical treatment is reserved for those with discomfort or ulcers refractory to medical management. Below are several conditions and the surgical options considered appropriate for each.
Chronic venous insufficiency resulting from superficial vein disorders
Vein ligation is the treatment of choice for superficial vein disorders. Historically, the entire greater saphenous vein system was removed; this has been replaced by the stab evulsion technique.
Several 2- to 3-mm incisions are made overlying the greater saphenous at various levels. The vein is dissected from the underlying tissues and any perforators are ligated. A small hook or blunt needle is used to extract as much of the vein as possible.
Typically, stab evulsion is limited to areas above the knee in the greater saphenous system to avoid damage to the saphenous nerve or sural nerve. This technique is reserved for CVI in which reflux in the saphenous system occurs and causes severe symptoms. For this reason, a diagnosis (usually accomplished with photoplethysmography or duplex imaging of reflux) must be established preoperatively. Hematoma, sural or saphenous nerve damage, and infection are possible complications of vein ligation.
Chronic venous insufficiency resulting from deep vein disorders
The decision to operate on a patient with venous obstruction in the deep veins should be made only after a careful assessment of symptom severity and direct measurement of both arm and foot venous pressures. Venography alone is not sufficient because many patients with occlusive disease have extensive collateral circulation, rendering them less symptomatic. Clot lysis (eg, tissue plasminogen activator [TPA], urokinase) and thrombectomy have been tried but have largely been abandoned owing to extremely high recurrence rates.
For iliofemoral disease, the operation of choice is a saphenous vein crossover graft. In the procedure, the contralateral saphenous vein is mobilized and divided at its distal end. It then is tunneled suprapubically and anastomosed to the femoral vein on the diseased side. The result is the diversion of venous blood through the graft and into the intact contralateral venous system
Because of a relatively high failure rate of 20%, ringed polytetrafluoroethylene (PTFE) grafts are used. The long-term patency is unknown.
Superficial femoral vein occlusion
Described by Warren in 1954 and Husni in 1983,13 the Husni bypass (as it has come to be called) is used to treat occlusion of the superficial femoral vein. The ipsilateral greater saphenous vein is harvested and used as an in situ popliteal-femoral vein bypass. This surgery is performed infrequently due to the high failure rate (approximately 40%). For a minimally invasive technique using stents, see Raju and Neglén.14
Deep vein incompetence
Valvuloplasty is reserved for patients with a congenital absence of functional valves. A venotomy is performed, and the valve cusps are plicated. To ensure an adequate result, plicating 20-25% of each cusp is recommended. The addition of a PTFE sleeve around the operative site is used routinely to maintain valve integrity. When combined with the ligation of perforating veins, valvuloplasty has a superior outcome in 80% of cases after 5 years.
With vein segment transposition, a vein with normal function in close proximity to the diseased vessel is identified. The incompetent vein then is dissected, mobilized, and transposed on to the normal vein distal to a functional valve.
With vein valve transplantation, a valve-containing segment of a competent axillary or brachial vein is mobilized and inserted into either the popliteal or the femoral systems. The incompetent segment of the leg vein is excised and replaced with the transplant segment. Allograft or cadaveric vein transplants are being tested, with long-term results pending.
Both invasive and noninvasive studies are conducted.
Invasive studies
Contrast venography is the criterion standard for assessing venous reflux, vein abnormalities, and the presence of valves. Ambulatory venous pressure is measured by placing a catheter in a vein on the dorsum of the foot during exercise.
Noninvasive studies
Commonly, both Doppler bidirectional-flow studies and Doppler color-flow studies are used to assess venous flow, its direction, and the presence of thrombus.
Photoplethysmography uses infrared light to assess capillary filling during exercise. Increased capillary filling is indicative of venous reflux and, consequently, incompetent veins.
Outflow plethysmography involves placing and subsequently releasing a tourniquet on the lower extremity; the veins should quickly return to baseline pressures, and failure to do so indicates reflux


