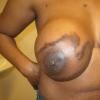
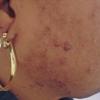
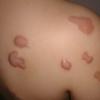
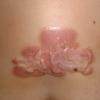
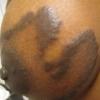
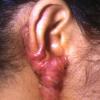
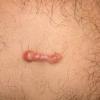
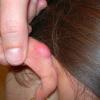
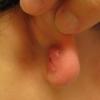
Keloids are the result of an overgrowth of dense fibrous tissue that usually develops after healing of a skin injury. The tissue extends beyond the borders of the original wound, does not usually regress spontaneously, and tends to recur after excision. The first description of keloids (recorded on papyrus) concerned surgical techniques used in Egypt in 1700 BCE. Subsequently, in 1806, Alibert used the term cheloide, derived from the Greek chele, or crab's claw, to describe the lateral growth of tissue into unaffected skin
In contrast, hypertrophic scars are characterized by erythematous, pruritic, raised fibrous lesions that typically do not expand beyond the boundaries of the initial injury and may undergo partial spontaneous resolution. Hypertrophic scars are common after thermal injuries and other injuries that involve the deep dermis.
Hypertrophic scars and keloids can be described as variations of typical wound healing. In a typical wound, anabolic and catabolic processes achieve equilibrium approximately 6-8 weeks after the original injury. At this stage, the strength of the wound is approximately 30-40% that of healthy skin. As the scar matures, the tensile strength of the scar improves as a result of progressive cross-linking of collagen fibers. At this point, the scar is usually hyperemic and it may be thickened, but it tends to subside gradually over months until a flat, white, pliable, possibly stretched, mature scar has developed. When an imbalance occurs between the anabolic and catabolic phases of the healing process, more collagen is produced than is degraded, and the scar grows in all directions. The scar is elevated above the skin and remains hyperemic. Excessive fibrous tissue is classified as either a keloid or a hypertrophic scar.
Kischer and Brody declared the collagen nodule to be the identifying structural unit of hypertrophic scars and keloids.1 The nodule, which is absent from mature scars, contains a high density of fibroblasts and unidirectional collagen fibrils in a highly organized and distinct orientation. In addition, keloids and hypertrophic scars differ from healthy skin by a rich vasculature, high mesenchymal cell density, and thickened epidermal cell layer. Attempts to clinically differentiate keloids from hypertrophic scars have proved to be difficult in the early phases of formation. Clinical differences become more apparent as lesions mature. The most consistent histologic difference is the presence of broad, dull, pink bundles of collagen in keloids, which are not present in hypertrophic scars.
Keloids manifest as exaggerated growths of scar tissue, usually in areas of previous trauma. Keloids extend past the areas of trauma, projecting above the level of the surrounding skin, but they rarely extend into underlying subcutaneous tissue.
Hypertrophic scars remain limited to the traumatized area and regress spontaneously within 12-24 months, although regression may not necessarily be complete.
Once lesions occur, the clinical course varies. Most lesions continue to grow for weeks to months and others grow for years. Growth is usually slow, but keloids occasionally enlarge rapidly, tripling in size within months. Once they stop growing, keloids do not usually cause symptoms and remain stable or involute slightly.
Keloids on the ears, neck, and abdomen tend to be pedunculated. Keloids on the central chest and extremities are usually raised with a flat surface, and the base is often wider than the top.
Most keloids are round, oval, or oblong with regular margins; however, some have clawlike configurations with irregular borders. Keloids overlying a joint can contract and restrict movement.
Most patients present with 1 or 2 keloids; however, a few patients, especially patients with spontaneous keloids, have multiple lesions, as do patients who develop keloids as a consequence of acne or chickenpox
Medical Care
No single therapeutic modality is best for all keloids. The location, size, and depth of the lesion; the age of the patient; and the past response to treatment determine the type of therapy used.
Prevention is key, but therapeutic treatment of hypertrophic scars and keloids includes occlusive dressings, compression therapy, intralesional corticosteroid injections, cryosurgery, excision, radiation therapy, laser therapy, interferon (IFN) therapy, 5-fluorouracil (5-FU), doxorubicin, bleomycin, verapamil, retinoic acid, imiquimod 5% cream, tamoxifen, tacrolimus, botulinum toxin, and over-the-counter treatments (eg, onion extract; combination of hydrocortisone, silicon, and vitamin E).
Other promising therapies include antiangiogenic factors, including vascular endothelial growth factor (VEGF) inhibitors (eg, bevacizumab), phototherapy (photodynamic therapy [PDT], UVA-1 therapy, narrowband UVB therapy), transforming growth factor (TGF)–beta3, tumor necrosis factor (TNF)-alpha inhibitors (etanercept), and recombinant human interleukin (rhIL-10), which are directed at decreasing collagen synthesis
.
Standard Treatments
These include occlusive dressings, compression therapy, and intralesional corticosteroid injections.
Occlusive dressings
Occlusive dressings include silicone gel sheets and dressings, nonsilicone occlusive sheets, and Cordran tape. These measures have been used with varied success. Antikeloidal effects appear to result from a combination of occlusion and hydration, rather than from an effect of the silicone.
Previous studies have shown that in patients treated with silicone occlusive sheeting with pressure worn 24 h/d for up to 12 months, 34% showed excellent improvement, 37.5% showed moderate improvement, and 28% demonstrated no or slight improvement.
Of patients treated with semipermeable, semiocclusive, nonsilicone-based dressings for 8 weeks, 60% experienced flattening of keloids, 71% had reduced pain, 78% had reduced tenderness, 80% had reduced pruritus, 87.5% had reduced erythema, and 90% were satisfied with the treatment.
Cordran tape is a clear surgical tape that contains flurandrenolide, a steroid that is uniformly distributed on each square centimeter of the tape, and it has been shown to soften and flatten keloids over time.
Compression therapy
Compression therapy involves pressure, which has long been known to have thinning effects on skin. Reduction in the cohesiveness of collagen fibers in pressure-treated hypertrophic scars has been demonstrated by electron microscopy.
Compression treatments include button compression, pressure earrings, ACE bandages, elastic adhesive bandages, compression wraps, spandex or elastane (Lycra) bandages, and support bandages. In one study, button compression (2 buttons sandwiching the earlobe applied after keloid excision) prevented recurrence during 8 months to 4 years of follow-up observation.
Other pressure devices include pressure earrings and pressure-gradient garments made of lightweight porous Dacron, spandex (also known as elastane), bobbinet fabric (usually worn 12-24 h/d), and zinc oxide adhesive plaster. Overall, 60% of patients treated with these devices showed 75-100% improvement.
Corticosteroids
Corticosteroids, specifically intralesional corticosteroid injections, have been the mainstay of treatment. Corticosteroids reduce excessive scarring by reducing collagen synthesis, altering glucosaminoglycan synthesis, and reducing production of inflammatory mediators and fibroblast proliferation during wound healing. The most commonly used corticosteroid is triamcinolone acetonide (TAC) in concentrations of 10-40 mg/mL administered intralesionally with a 25- to 27-gauge needle at 4- to 6-week intervals.
Intralesional steroid therapy as a single modality and as an adjunct to excision has been shown to be efficacious in various studies. Response rates varied from 50-100%, with recurrence rates of 9-50% in completely resolved scars. When combined with excision, postoperative intralesional TAC injections yielded a recurrence rate of 0-100%, with most studies citing a rate of less than 50%. Complications of repeated corticosteroid injections include atrophy, telangiectasia formation, and pigmentary alteration.
Recent Innovations
New treatments for keloids and hypertrophic scars include intralesional IFN; 5-FU; doxorubicin; bleomycin; verapamil; retinoic acid; imiquimod 5% cream; tacrolimus; tamoxifen; botulinum toxin; TGF-beta3; rhIL-10; VEGF inhibitors; etanercept; mannose-6-phosphate inhibitors (M6P); etanercept; onion extract; the combination of hydrocortisone, silicon, and vitamin E; PDT; intense pulsed light (IPL); UVA-1; and narrowband UVB.
IFN therapy
IFN therapy, including IFN alfa, IFN beta, and IFN gamma, has been demonstrated in in vitro studies to reduce keloidal fibroblast production of collagen types I, III, and VI mRNA.
IFN alfa and IFN beta also reduce fibroblast production of glycosaminoglycans (GAGs), which form the scaffolding for the deposition of dermal collagen. IFN gamma enhances GAG production.
IFN alfa, IFN beta, and IFN gamma have been shown to increase collagenase activity. Studies have shown that IFN gamma modulates a p53 apoptotic pathway by inducing apoptosis-related genes. p53 is a protein synthesized following DNA damage. Once damage is repaired, p53 is degraded. Mutations of this protein are believed to predispose cells to hyperproliferation, possibly resulting in keloid formation. In addition, p53 is a potent suppressor of interleukin (IL)–6, a cytokine implicated in hyperproliferative and fibrotic conditions.
IFN injected into the suture line of keloid excision sites may be prophylactic for reducing recurrences. Berman and Flores reported statistically significant fewer keloid recurrences in a study of 124 keloid lesions after postoperative IFN alfa-2b injection treatment (5 million U, 1 million U injected per cm of scar) into keloid excision sites (18%) versus excision alone (51.1%) and TAC treatment (58.4%).2
Tredget et al showed a significant increase in the rate of scar improvement compared with the control period of time (P = .004) after injecting 9 patients with hypertrophic scars with 1 X 106 units of human recombinant IFN alfa-2b subcutaneously, daily for 7 days, and then 2 X 106 units administered 3 times per week for 24 weeks in total.3 Scar assessment (P <.05) and scar volume (P <.05) also improved after 3 months of treatment. No recurrences were reported after stopping IFN therapy.
Conejo-Mir et al reported that 66% of keloids (n = 20) did not recur after 3 years of follow-up after treating 30 keloids with ultrapulse carbon dioxide laser ablation followed by sublesional and perilesional injections of 3 million IU of IFN alfa-2b 3 times per week.4
In a 2008 prospective study, Lee et al reported decreases in depth (81.6%, P = .005) and volume (86.6%, P = .002) treating 20 keloids with a combination of intralesional TAC and IFN alfa-2b compared with only a nonsignificant improvement (P = .281 and P = .245, respectively) obtained in 20 keloids treated with TAC alone.5
Notably, however, several studies have failed to demonstrate the efficacy of IFN alfa-2b for the treatment of keloids and hypertrophic scars, including a case series of 5 patients treated by Wong et al,6 a case series by al-Khawajah of 22 patients with keloids using lower doses of IFN alfa-2b than in prior studies,7 and a prospective randomized clinical trial by Davison et al in which 50 patients with keloids received intraoperative intradermal injections of IFN alfa-2b at 10 million U/mL or TAC at 40 mg/mL, both receiving an extra injection 1 week later.8
Hypertrophic scar intralesional injections of human recombinant IFN gamma at 200 mcg (6 X 106 U) per injection for 4 weeks have been reported by Pittet et al to be effective for relieving the symptoms in 6 of 7 patients and decreases in redness, swelling, firmness, and lesion area in 7 of 7 patients.9 At week 16, the reappearance of symptoms was minimal in only 2 of 7 patients and a small increase in the lesion area occurred in 4 of 7 patients, although these lesions remained smaller than the original area.
5-Fluorouracil
5-FU, a pyrimidine analogue with antimetabolite activity, inhibits fibroblastic proliferation in tissue culture and is believed to reduce postoperative scarring by decreasing fibroblast proliferation. Its efficacy and safety have been reported when used as a monotherapy or when used in combination with other drugs (eg TAC) for the treatment of other fibrosing conditions, including infantile digital fibromatosis, knuckle pads, rheumatoid nodules, and adverse foreign body reaction and sarcoidal granulomatous complications after soft tissue filler injection. Some data suggest that 5-FU is effective in the treatment of hypertrophic scars and is somewhat effective in small keloids. Several studies have shown the effectiveness of 5-FU.
In a retrospective study of 1000 patients with hypertrophic scars and keloids over a 9-year period, the most effective regimen was found to be 0.1 mL of TAC (10 mg/mL) and 0.9 mL of 5-FU (50 mg/mL) up to 3 times a week.
A total of 85% of keloids showed more than 50% improvement in an open study by Kontochristopoulos et al in which 20 keloids were treated once weekly with intralesional 5-FU (50 mg/mL) for an average of 7 treatments, with a recurrence rate of 47% within 1 year of the treatment. The Ki-67 proliferative index was significantly reduced (P = .0001) after treatment.10
Nanda and Reddy treated 28 patients with multiple keloids in a prospective, randomized, uncontrolled clinical trial with weekly intralesional injections of 5-FU at 50 mg/mL and reported almost 80% of the patients showing more than 50% improvement. Regression from the periphery and flattening occurred in all patients. In 22 of 28 patients, the symptoms completely disappeared, while the rest showed a good response. Decrease in size was reported in 70% of the patients.11
5-FU in combination with other therapies significantly increases the efficacy over single modalities. In a randomized clinical trial by Asilian et al, 69 patients with keloids and hypertrophic scars were treated with a combination of 5-FU (50 mg/mL), TAC (40 mg/mL), and a 585-nm flashlamp-pumped pulsed-dye laser (PDL) at 5-7.5 J/cm2), showing that it was more effective than the TAC and TAC plus 5-FU.12 At week 12, a statistically significant reduction in length, height, and width was observed in all groups compared with baseline (P <.05). In a randomized clinical trial, Manuskiatti and Fitzpatrick found a statistically significant clinical improvement in keloidal and hypertrophic sternotomy scars using these 3 modalities separately and a combination of TAC and 5-FU compared with baseline. No difference was found between the 4 treatment modalities.13
5-FU was used to treat a patient with keloids and hypertrophic scars post facial dermabrasion. The patient received 6 intralesional injections of 5-FU with silicone sheets applied afterwards over a 3-month span. During 7 months of follow up, a significant improvement in the size, color, and texture of the scars was noticed. In addition, the pain and itching had fully resolved.1
Doxorubicin (Adriamycin)
Doxorubicin (Adriamycin) is a commonly used chemotherapeutic agent that irreversibly inactivates prolyl 4-hydroxylase in human skin fibroblasts and has been shown to inhibit collagen alpha-chain assembly.
Sasaki et al showed through sodium dodecyl sulfate-polyacrylamide gel electrophoresis (SDS-PAGE) analysis that doxorubicin, at a clinically therapeutic concentration of 12.5 µm, inhibits the assembly of collagen triple-helical molecules.15 SDS-PAGE analysis of control cultures showed a large fraction of [3H]proline-labeled procollagen polypeptides in triple-helical conformation; however, after the addition of doxorubicin at 12.5 µm, a very small amount of intact alpha-chains were found. These results suggest that the impaired wound healing observed in cancer patients who receive doxorubicin may result from the inhibition of prolyl 4-hydroxylase.
Another mechanism of doxorubicin-induced inhibition of collagen synthesis includes the inhibition of the enzyme prolidase, which is key in the process of collagen resynthesis, cleaving imidodipeptides containing C-terminal, and making proline available for its recycling and further generation of new collagen. Muszynska et al demonstrated this process in cultured human skin fibroblasts, also suggesting that this inhibition is a posttranslational event.16,17
Other agents such as doxycycline, other nonsteroidal anti-inflammatory drugs (ie, acetylsalicylic acid, sodium salicylate, phenylbutazone, indomethacin), daunorubicin, gentamicin, netilmicin, anthracycline)18 are also capable of inhibiting prolidase in cultured human skin fibroblasts. Further studies are warranted to determine if doxorubicin or any of the above-mentioned agents can be useful to treat patients with excessive scarring.
Bleomycin
Bleomycin injections cause necrosis of keratinocytes with a mixed inflammatory infiltrate. Several studies have demonstrated that bleomycin can be used effectively to treat keloids and hypertrophic scars.
Bleomycin was given at a concentration of 1.5 IU/mL to 13 patients using the multiple-puncture method. Bleomycin was dripped onto the lesion, and then multiple punctures were made on the lesions using a syringe. Seven patients had complete flattening, 5 patients had highly significant flattening, and 1 patient had significant flattening. Likewise, Espana et al also reported complete flattening in 6 of 13 patients, highly significant flattening in 6 of 13 patients, and significant flattening in a single patient. Two patients presented a recurrence as a small nodule 10 and 12 months after the last infiltration.19
In another study of 31 keloids, patients were treated with 3-5 infiltrates of bleomycin within a 1-month period. Total regression occurred in 84% of the keloids, and both keloid volume and functional impairment were reduced.
Bodokh and Brun reported complete flattening in 69.4% of 36 patients with keloids and hypertrophic scars.20 Saray et al obtained complete flattening in 73.3%, highly significant flattening in 6.7%, and moderate flattening in 6.7% of lesions after the administration of jet intralesional injections of bleomycin in 15 patients.21
In the only randomized clinical trial using the tattooing technique, with which smaller amounts of the drug are absorbed, thus minimizing systemic adverse effects, Naeini et al reported significantly better results with intralesional bleomycin compared with the control group (ie, combination of cryotherapy and TAC) in lesions larger than 100 mm2 (P = .03).22 Local complications, such as hyperpigmentation, were observed in 75% of the patients.
Fifty patients with keloids and hypertrophic scars were treated with intralesional bleomycin. Three applications were given at 15-day intervals, and a fourth and final application was given 2 months after the third application. Complete flattening was observed in 44%, significant flattening in 22%, adequate flattening in 14%, and no flattening in 20%. Pruritus was relieved completely in 89% of patients.23
Verapamil
Verapamil is a calcium channel blocker that blocks the synthesis and secretion of extracellular matrix molecules (eg, collagen, GAGs, fibronectin) and increases fibrinase.
In a study of 22 patients with keloids, patients were treated with surgical excision and 5 treatments of verapamil at 2.5 mg/mL (varying doses from 0.5-5 mL, depending on keloid size) over a 2-month period and were evaluated at 2-year follow-up. Two patients had keloids that decreased in size from the original lesion, 2 patients had hypertrophic scars, 4 patients had pruritus, and 1 patient had a keloid on the donor site. The case series reported an average of 6.4 in patient satisfaction on a scale from 1 to 10.24
D’Andrea et al, from a case-control comparative study, reported resolution in 54% of the patients who had their keloids treated by a combination of surgical excision, silicon sheeting, and intralesional verapamil versus 18% in the control group without intralesional verapamil.25 The recurrence rate was 36% in the active group after 18 months of follow up.
In a case series, Skaria reported complete resolution of 4 of 6 keloids and 1 of 2 hypertrophic scars at 1-year follow-up after surgical removal of the scar and further intralesional injection of verapamil at doses of 2.5 mg/mL.26
Lawrence reported 55% cured earlobe keloids in 52% of the patients after the combination of surgical excision, intralesional verapamil, and pressure earrings after an average of 28 months of follow-up.27
In a randomized clinical trial, Margaret Shanthi et al compared intralesional verapamil and intralesional TAC for the treatment of keloids and hypertrophic scars, reporting a reduction in vascularity, pliability, height, and width in both groups after 3 weeks of treatment. This result was maintained at 1 year after stopping the treatment. Although the rate of improvement was faster in the TAC group, overall, no difference was noted between the 2 groups.28
Retinoic acid
Retinoic acid decreases normal tonofilament and keratohyalin synthesis, increases the production of mucoid substances and the epidermal cell growth rate, and inhibits DNA synthesis in vitro.
In a clinical trial involving 21 patients with 28 keloids and hypertrophic scars, topical retinoic acid was applied for at least 3 months twice daily and showed favorable results in 77-79% of the lesions. This includes a decrease in the size and symptoms of the scar.29
In addition, because retinoids affect collagen metabolism, another study involving 9 females and 2 males with keloids treated with 0.05% tretinoin topically for 12 weeks showed a significant decrease in weight (P <.04) and size (P <.01) of the keloids when comparing the status of the lesions at the beginning of the study and at week 12.30
In vitro studies have demonstrated that retinoids can modulate collagen production and the proliferation of normal and keloidal fibroblasts. In vivo applications of 0.05% topical retinoic acid can lead to a reduction of hypertrophic scars in 50-100% of patients and of keloids in less than 20% of patients. The most common adverse effects reported have been photosensitivity, irritant contact dermatitis, and skin atrophy.
Imiquimod
Imiquimod (1-[2-methylpropyl]-1H-imidazo[4,5-c]quinolin-4-amin) belongs to the family of imidazoquinolines. Imiquimod induces TNF-alpha, IFN-alpha and IFN-gamma, IL-1, IL-4, IL-5, IL-6, IL-8, and IL-12 and alters the expression of markers for apoptosis.
In one study, 13 keloids were treated with excision in combination with nightly applications of imiquimod 5% cream for 8 weeks. Ten patients with 11 keloids completed the 6-month study, and no keloids recurred after 6 months. Mild irritation was experienced with the application of imiquimod, and some patients needed a vacation period from the medication. Hyperpigmentation was experienced by more than half of the patients in the study.
In 2 different pilot studies, imiquimod 5% cream was applied on postshaved or totally excised earlobe keloids. It was demonstrated that the recurrence rate on postshaved keloids was 0% after 12 months of follow-up and 75% recurrence-free after 24 weeks of parallel keloid excision. Although the presence of local adverse events did not affect the treatment, a resting period was needed.31,32
In a different study, 15 patients with hypertrophic scars 2 months after breast surgery were treated with either petrolatum or imiquimod 5% cream. At 24 weeks, almost all the scars treated with imiquimod scored better after assessment with standardized scales. The results demonstrated that imiquimod treatment improved scar quality and color match after surgery.
More recently, in study by Chuangsuwanich et al, 45 patients with excised keloids were treated with imiquimod 5% cream 2 weeks after the operation, on alternate nights, for 8 weeks.33 After a follow-up period of 6-9 months, 10 of the keloids recurred (28.6% overall recurrence rate), with adverse effects found in 13 patients (37.1%). Interestingly, the keloids localized on the pinna had the lowest recurrence rate (2.9%) compared with those at the chest wall or neck (83.3% and 14.3%, respectively).
Tacrolimus
Tacrolimus is an immunomodulator that inhibits TNF-alpha. Gli -1, an oncogene, has been found to be overexpressed in fibroblasts of keloids. Inhibition of this oncogene may restore the natural apoptosis process and decrease proliferation of the ECM protein.34 Rapamycin, a close analogue of tacrolimus, was used in an in vitro study and was found to inhibit the gli -1 oncogene, thus giving a rationale to initiate clinical trials of topical tacrolimus and rapamycin.
In an open-label pilot study, 11 patients used tacrolimus 0.1% ointment twice daily for 12 weeks on their keloids. Although the results were not statistically significant, the study showed a decrease in induration, tenderness, erythema, and pruritus for most patients.
Kim et al observed the resolution of a keloid in a patient during a course of topical tacrolimus for atopic dermatitis.34
Sirolimus
Sirolimus is an inhibitor of the mammalian target of rapamycin (mTOR), a serine/threonine kinase that regulates collagen expression. By inhibiting mTOR, sirolimus blocks the response to IL-2 and decreases ECM deposition.35 Similar to rapamycin, sirolimus inhibits Gli -1 signal transduction.
A higher concentration of VEGF and higher blood vessel density has been found in the basal layer of the epidermis of keloidal tissue in comparison to normal skin. In co-cultured keloid keratinocytes and fibroblasts exposed to sirolimus, VEGF expression has shown to be down-regulated in a dose-dependent manner. Through inhibition of VEGF, sirolimus may control the expression profile of underlying dermal fibroblasts.
Tamoxifen
Tamoxifen, a synthetic nonsteroidal antiestrogen used to treat breast cancer, has been shown to inhibit proliferation of keloid fibroblasts and their collagen synthesis in monolayer cultures. Hu et al demonstrated that tamoxifen exhibits a dose-dependent and reversible inhibition of contraction of adult human dermal fibroblast in vitro.36
Tamoxifen has also been shown to reduce TGF-alpha, and its isoform TGF-alpha1, production by keloid fibroblasts in vitro. Mikulec et al have shown that keloid fibroblasts have significantly lower TGF-alpha1 production when exposed to 16 µmol/L of tamoxifen at day 2 of culture when compared with control keloid fibroblasts (P = .05).37
Botulinum toxin A
Botulinum toxin A (BTA) is a neurotoxin that causes a flaccid paralysis of the local musculature and reduces skin tension. This reduction in the skin tensile force during the course of wound healing may represent a novel therapeutic target for treating keloids.
In an in vitro study, 64% of cultured fibroblasts were found to be in the G0-G1 phase of the cell cycle when exposed to BTA, while 35.4% were in the proliferative phases (ie, G2, M, S). In comparison, cultured fibroblasts that were not exposed to BTA had the following distribution: 36% (G0-G1) and 64% (proliferative phases).38 The effect of BTA on the cell cycle distribution of fibroblasts may indicate that BTA can improve the eventual appearance of and inhibit the growth of hypertrophic scars and keloids.
In a prospective, uncontrolled study evaluating the effects of BTA in the treatment of keloids, 12 keloids were injected intralesionally at a concentration of 35 U/mL, with the total dose varying from 70-140 U per session. Injections were given at 3-month intervals for a maximum of 9 months. At 1-year of follow up, the therapeutic outcomes were excellent (n = 3), good (n = 5), and fair (n = 4), with no patients failing therapy or showing signs of recurrence.39
Nineteen patients with hypertrophic scars received intralesional injections of BTA (2.5 U/mL at 1-mo intervals) for 3 months. All patients showed acceptable improvement of the scars at 6 months of follow up. The erythema, pruritus, and pliability scores were significantly lower post-BTA injections compared with baseline.40
Intramuscular injections of BTA along with scar revision techniques on the face may help to reduce the development of a wider scar.41
Larger, randomized, controlled studies are warranted to determine the role of BTA in the treatment of keloids and hypertrophic scars.
TGF-beta and isomers
TGF-beta and its isomers have been shown to play a central role in fibrotic disorders characterized by excessive accumulation of interstitial matrix material in the lungs, kidneys, liver, and other organs. TGF-beta1 and TGF-beta2 have been shown to stimulate fibroblasts to produce collagen and have a direct and independent effect on the contraction of fibroblasts in vitro. However, TGF-beta3 may prevent scarring.
A study by Shah et al demonstrated that exogenous addition of TGF-beta3 reduces fibronectin and collagen types I and III deposition in the early stages of cutaneous rat wound healing and in overall wound scarring.42
A new antifibrotic product, avotermin (Juvista, Renovo; Manchester, United Kingdom), will be released in the future. Avotermin is derived from human recombinant TGF-beta3. This new medication has shown promise in a phase I trial and 2 phase II trials completed in the United Kingdom. In these studies, wounds treated with avotermin showed a statistically significant improvement in scar appearance, with a response rate of greater than 70%. After analyzing safety data on more than 1500 human subjects, avotermin does not seem to have safety or tolerability issues for use in the prevention or reduction of scarring.
In a randomized, double-blind, placebo-controlled, within-patient, phase II trial to investigate the safety and efficacy of 200 ng per 100 μL per linear cm of wound margin of avotermin when administered twice following scar revision surgery, the overall analysis showed that the primary endpoint (ie, photographic evaluation by a lay panel over a period from week 6 to month 7 postsurgery using a visual analogue scale) was met (P = .038). Investigator assessment at 7 months postsurgery using a visual analogue scale also obtained statistical significance (P = .036). Approximately 75% of the 7-month scars assessed from avotermin-treated wounds were considered to have a structure more like normal skin compared with the placebo in the histopathological analysis.43
Currently, several clinical trials are being conducted or are in development, including phase I, II, and III trials, to further investigate the efficacy and safety of avotermin for the treatment and prevention of keloids and hypertrophic scars. Results are expected from 2009 to 2012
Interleukins
ILs also regulate fibroblast differentiation and proliferation, and IL-10 has been shown to induce scarless healing when overexpressed in adult mouse wounds. Renovo (Manchester, United Kingdom) has developed Prevascar, a human recombinant IL-10 formulation. Preclinical experiments have demonstrated that application of Prevascar to the margins of acute incisional wounds by intradermal injection decreases subsequent scarring. In a phase II, double-blinded, placebo-controlled, randomized clinical trial to evaluate the antiscarring efficacy of varying doses of Prevascar in 175 subjects (1400 wounds), Renovo reported statistically significant efficacy data for the reduction of scarring in the skin.
Onion extract
Onion extract, that is, extract of Allium cepa, and specifically its derivative quercetin, is a bioflavonoid with antibacterial, fibrinolytic, antihistamine-releasing, and antiproliferative effects on both normal and malignant cells that can be found in onions and apples, red wine, and black tea.
Additional biological activities described include inhibition of the Na+ K+ ATPase, protein kinase C, tyrosine kinase, HIV reverse transcriptase, and pp60src kinase. It inhibits enzymes involved in the proliferation of signaling pathways (eg, phosphatidylinositol 3-kinase [PI-3K], 1-phosphatidylinositol 4-kinase), and it causes cell cycle arrest and apoptosis. In vitro studies have demonstrated that quercetin inhibited keloid fibroblast proliferation, collagen synthesis, basal expression, and activation of several key proteins in the insulinlike growth factor (IGF)-I, which is a potent mitogen and inhibitor of apoptosis that stimulates fibroblast proliferation and enhances collagen synthesis.
Several prospective, randomized clinical trials have reported the efficacy of onion extract either for the prevention of keloid and hypertrophic scar development after surgery or for the management of these preexisting hyperplastic scars.
- Chung et al reported no significant difference comparing onion extract with petrolatum, but none of the scars became keloidal or hypertrophic at least 11 months after the surgery.49
- Draelos applied onion extract to postshaving wounds and reported significant differences in several parameters, including softness, redness, texture, and overall appearance compared with no treatment (P <.001).50
- Ho et al treated wounds of patients who underwent laser removal of tattoos with a combination of 10% aqueous onion extract, 50 U heparin per gram of gel, and 1% allantoin, reporting that only 11.5% of wounds developed scarring, compared 23.5% in the control group (P <.05).51
For the treatment of preexisting scars, the combination of onion extract with other agents seems to generate better results than onion extract alone.
- Koc et al reported that both a combination of onion extract and TAC and TAC alone significantly improved all parameters measured compared with baseline (P <.05, and P <.05 respectively); however, the combination was more effective than TAC for pain, sensitiveness, itching, and elevation.52
- Hosnuter et al reported significant improvement of several clinical parameters with onion extract, including erythema (P <.05) and color of the scar (P <.01), compared with silicon sheet; however, a combination of onion extract and silicon sheet resulted in better results than with onion extract alone and silicon sheet alone.53
- Comparing onion extract and a combination of 0.5% hydrocortisone, silicone, and vitamin E versus placebo, Perez et al reported significant improvement in more parameters generated by the combination (7 of 12) than the onion extract (4 of 12) and placebo (2 of 12) compared with baseline. A trend towards greater satisfaction was reported by patients in the onion extract group compared with the combination group and both treatments compared with the placebo group.54
Combination of therapeutic agents
A combination of therapeutic agents, created in theory to obtain a beneficial synergistic effect in the treatment of keloids and hypertrophic scars, has been developed that contains 0.5% hydrocortisone, 0.5% vitamin E, and 12% silicone. Each of the 3 components has been demonstrated, in varying degrees, to be effective for the treatment of keloids and hypertrophic scars.
Corticosteroids inhibit collagen synthesis, stimulate collagenase activity, enhance collagen degradation, decrease the proliferation of inflammatory mediators in wounds, decrease fibroblast proliferation, and decrease GAG synthesis. Silicone provides occlusion and hydration to the wound surface. Occlusion decreases collagen formation, mitogenic activity, and capillary formation. In addition, silicone induces a negative ionic charge at the wound surface, inhibiting collagen formation. Vitamin E has been postulated to inhibit collagen synthesis, stimulate collagenase expression, decrease fibroblast proliferation, and reduce inflammation in the wound.
In a preliminary in vitro study, Scarguard applied to a full-thickness epidermal model resulted in an increase in procollagenase levels and collagenase activity, suggesting its potential clinical use.55
Eisen applied Scarguard to surgical wounds in patients with a history of developing keloids and hypertrophic scars in an open-label, pilot study, reporting better results in 9 of 12 patients for redness and overall appearance and better results in 6 of 12 patients for texture of the scars compared with the untreated control.56
In a previously mentioned study (regarding onion extract) by Perez et al, Scarguard improved more clinical parameters than onion extract and placebo when used to treat keloids and hypertrophic scars in a randomized clinical trial.54
Vitamin E
Vitamin E (tocopherol) is a lipid-soluble antioxidant with multiple biological effects, including the reduction of reactive oxygen species, which hamper healing and cause damage to the DNA molecule, cellular membranes, and lipids. In addition, vitamin E (tocopherol) also alters collagen and GAG production and inhibits the spread of peroxidation of lipids in cellular membranes, thus acting as a membrane-stabilizing agent. Only anecdotal reports have shown that vitamin E speeds wound healing and improves the cosmetic appearance of scars.
When vitamin E has been used in combination with other treatments for scars, such as silicone gel sheets, it has been demonstrated in a prospective randomized clinical trial to improve preexisting hypertrophic scars by 50% in 95% of the patients, compared with 50% improvement in 75% of the patients treated with silicon sheets alone after 2 months of treatment (P <.05).57 However, topical vitamin E has been consistently associated with the development of contact dermatitis.
In a prospective, double-blinded, randomized clinical trial Baumann and Spencer applied a combination of Aquaphor with the content of 2 d-alpha-tocopherol oral vitamin supplement capsules, added at a concentration of 320 IU/g, versus Aquaphor alone to postsurgical wounds and reported no benefit to the cosmetic outcome of scars treated with vitamin E. In addition, in 90% of the cases, vitamin E had either no effect on, or worsened, the appearance of the scars.58
In a prospective, double-blinded, randomized clinical trial Jenkins et al reported no beneficial effect of either vitamin E or topical steroids when both treatments were applied post grafting procedures for reconstruction for postburn contractures.59
Radiation Therapy
Using radiotherapy to treat keloids remains controversial. Although many studies have demonstrated efficacy and decreased recurrence rates, the safety of radiotherapy has been questioned.
In a retrospective study of superficial x-ray therapy of 24 excised keloids, the author reported a recurrence rate of 53%. Use of iridium Ir 192 interstitial irradiation after excisional surgery resulted in a 21% recurrence rate after 1 year. Excisional surgery and preoperative hyaluronidase solution (150 U/mL sodium chloride) followed by external radiation (7.2-10.8 Gy) had a 0% recurrence rate. Adjunctive high dose-rate brachytherapy (192 Ir) used after excision and closure resulted in a 12% reoccurrence rate after 26 months.60
When excisional surgery is followed by postoperative radiation therapy, the total fractionated dose should be a minimum of 12 Gy, according to a comparative study showing a higher recurrence rate for patients treated with total doses less than 12 Gy.
Other Potential Therapies
Additional potential therapeutic options for treating hypertrophic and keloidal scarring that have been shown in vitro to affect collagen synthesis include the use of proline-cis -hydroxyproline and azetidine carboxylic acid, tranilast (antiallergic drug shown to decrease collagen and GAG synthesis), and pentoxifylline (inhibits DNA replication). In addition, wounds treated with anti-TGF healed with minimal scar tissue formation and without affecting wound tensile strength. A possible candidate for affecting wounds via the neutralizing effect of TGF is the proteoglycan termed decorin.
Gentian violet
Gentian violet (GV) potentially may be useful. Multiple growth factors have been implicated in the pathogenesis of keloids, including TGF-beta, IGF, and, most recently, the proangiogenic cytokine, VEGF.61
In a study by Gira et al, keloids were characterized as angiogenic lesions.62 Endothelial cell–specific signaling via the Tie2 receptor by its ligand angiopoietin-2 (ang-2) is crucial for angiogenesis, according to Lobov et al.63 They demonstrated that in the presence of VEGF-A, ang-2 promotes a rapid increase in capillary diameter, remodeling of the basal lamina, and proliferation and migration of endothelial cells and it stimulates sprouting of new blood vessels. Moreover, ang-2 promotes endothelial cell death and vessel regression if VEGF is inhibited.
Nicotinamide adenine dinucleotide phosphate (NADP) oxidase (Nox) genes have been linked to the angiogenic switch and regulate ang-2. Neutralization of ang-2 through Nox inhibition has been postulated as an effective therapy of hemangiomas of infancy.
GV, a triphenylmethane dye, has a chemical structure similar to diphenyl-iodonium (DIP), a specific Nox inhibitor. GV inhibits Nox2 and Nox4, expressed in endothelial cells. At high concentrations, GV effectively inhibited in vitro expression of ang-2 mRNA by 70-90%. In vivo, intralesional injections of GV into mice hemangiomas has resulted in a 92.6% decrease in tumor size and arrest of tumor progression compared with the control. No local or systemic toxicity was observed. Based on these results, GV may be considered in the future for the treatment of keloids, particularly if the keloids are definitively determined to be angiogenic lesions
.
Vascular endothelial growth factor
VEGF promotes neovascularization and cell growth in both normal skin and scar tissue. It induces mitosis in endothelial cells, increases vascular permeability, and promotes deposition of extravascular fibrin matrix.64 VEGF has been found to be overexpressed in the underlying dermis, epidermal keratinocytes, capillary lining cells, and fibroblasts of keloids in comparison with normal skin.62,65,66,67,68 The use of short interfering RNA (siRNA) sequences has been shown to inhibit the expression of VEGF, representing a potential therapeutic strategy for keloids.68
Basic fibroblast growth factor
Basic fibroblast growth factor (bFGF) significantly inhibits the differentiation of mesodermal progenitor cells into myofibroblasts, which mediate tissue fibrosis and are primary producers of collagen.69 bFGF has both mitotic and angiogenic properties, and it influences tissue remodeling, neovascularization, wound healing, and tumor growth. Rabbit-ear model studies have shown that through regulation of extracellular matrix production and degradation, bFGF accelerates wound healing and improves scar quality.70
In 230 sutured wounds, bFGF was administered one time locally during the immediate postoperative period. Patients received a low-dose intradermal injection (0.1 µg /cm wound), a high-dose intradermal injection (1 µg /cm wound), a rinse with high-dose bFGF (1 µg/cm wound), or no treatment (control group). At 6-12 months postsurgery, the minimum scarring ratios of the treated groups were statistically significant higher than the control group (P <.001, P <.0001, and P <.0001), respectively. No serious adverse events were reported.71 These results suggest that bFGF may represent an important tool for the treatment of keloids and hypertrophic scars. Further studies are warranted.
Hepatocyte growth factor
Hepatocyte growth factor (HGF) is a cytokine that modifies the levels of other cytokines, including VEGF and TGF-beta1, promoting regeneration and angiogenesis, and decreasing apoptosis and fibrosis. It may contribute to the prevention of scar formation.72
Suppression of apoptosis and fibroblast proliferation was obtained after postincisional intradermal administration of the HGF gene in rats. Enhancement of the healing process and decreased scarring were also reported.73 Further clinical trials evaluating HGF’s potential for the treatment of keloids and hypertrophic scars are needed.
Mannose-6-phosphate
M6P was developed to compete with the latent form of TGF-beta1 (a M6P-containing molecule) for M6P receptors. These receptors are multifunctional transmembrane glycoproteins that are involved in the proteolytic activation of the latent precursor of TGF-beta.74 By binding these receptors (and preventing TGF-beta1 from binding), M6P prevents further activation of TGF-beta1 and TGF-beta2, which may lead to the reduction of fibrosis.75
In a phase I dose-escalation study, both topically and intradermally injected M6P were found to be safe and well tolerated and to significantly accelerate epithelialization.76 Current trials are further exploring the role of M6P in the acceleration of wound healing, at 2 dose levels and through 2 routes of administration (intradermal and topical).77
Prostaglandin E2
Prostaglandin E2 (PGE2) is a major eicosanoid product of fibroblasts, synthesized from arachidonic acid by cyclooxygenases and PGE2 synthases. Although its up-regulation is related to increased fibrosis and scar formation, it has also been shown to decrease fibroblast proliferation, migration, and contraction and to reduce collagen levels by inhibiting its synthesis and promoting its degradation. Furthermore, keloid-derived fibroblasts have a diminished capacity to produce PGE2 and express less of the PGE2-specific receptor, E prostanoid receptor 2.78 This suggests that PGE2 has a dual nature of profibrotic and antifibrotic action and that it is its deregulation that leads to abnormal scar formation.
Histamine H1 blockers
Histamine H1 blockers are anti-inflammatory and antiproliferative agents that suppress the release of TGF-beta1 from keloidal fibroblasts and inhibit collagen synthesis and deposition79,80,81 In an in vitro study,82 when exposed to histamine, 60% of cultured fibroblasts from normal human and keloidal skin showed elevated growth rates in a dose-dependent fashion. This rate was decreased in the presence of diphenhydramine hydrochloride in histamine-sensitive keloidal strains. After exposure to pheniramine maleate, fibroblasts cultured from abnormal scars showed a reduction in the proliferation rate (63%), in DNA synthesis (63%), and in the collagen synthesis rate (73%).83 Antihistamines also have been shown to reduce the burning sensation, pain, and pruritus associated with keloids.84,85
Pycnogenol
Pycnogenol, a pine bark extract from Pinus pinaster, is mainly composed by procyanidins (65-75%), including catechin and epicatechin, and other components such as flavonoid monomers and phenolic or cinnamic acids. It inhibits the release of reactive oxygen species (ROS) and reduces inflammatory responses through inhibition of COX-2 and 5-lipoxygenase (5-LOX) gene expression and phospholipase A2 (PLA2) activity. These effects are associated with a compensatory up-regulation of COX-1 gene expression. Pycnogenol has also been shown to inhibit matrix metalloproteinase (MMP)–1, MMP-2, and MMP-9.86,87,88,89
Pycnogenol supplementation led to a 3-fold increase in PGE2 release from activated human polymorphonuclear leukocytes (PMNLs).90 It inhibits the nuclear factor kappaB (NF-kappaB)–dependent gene expression and decreases the activity of proinflammatory mediators and adhesion molecules, including vascular cell adhesion molecule-1 (VCAM-1) and intercellular adhesion molecule-1 (ICAM-1).In LPS-stimulated monocytes, pycnogenol also inhibits NF-kappaB activation and decreases TNF-alpha secretion. It blocks activator protein-1 and inhibits the expression of proinflammatory cytokine IL-1.
Pycnogenol decreases the expression of mast cell–related tryptase and stem cell factor, which may decrease inflammation and fibrosis. Further studies are warranted to determine the role of pycnogenol for the treatment of keloids.89,90
Mitomycin C
Mitomycin C is an antibiotic with antineoplastic and antiproliferative effects on fibroblasts.91 It causes cross-linkage of DNA double-helix strands, leading to inhibition of DNA synthesis.92 During 3 weeks following in vitro fibroblast exposure to mitomycin C, a decrease in fibroblast density and DNA synthesis was seen. Three weeks following removal of mitomycin C exposure, DNA synthesis recovered and the cell count increased.93
Topical mitomycin C 1 mg/mL was applied to wound beds for 3 minutes after keloid resection and then repeated after 3 weeks. Six months post treatment, 4 in 10 patients were pleased with the treatment outcome, 1 in 10 was disappointed, and approximately 80% were satisfied.94
In another study in which mitomycin 0.4 mg/5 mL was applied for 4 minutes in 10 patients following surgical excision of head and neck keloids, 9 in 10 patients had no recurrence after up to 14 months (mean, 8 mo).92
Eight patients were treated with keloid excision followed by application of mitomycin C for 5 minutes. At 14 months’ follow-up, 100% of patients were satisfied with the results and 2 patients experienced complete remission of their keloid.95
In a study using patients as their own controls,96 in which topical mitomycin C was applied to excised keloids, no difference was seen in keloid recurrence.
No adverse events to the mitomycin C have been reported.
AZX100
AZX100 is a synthetic peptide with a similar intracellular mechanism of action to the heat shock–related protein 20 (HSP20), which is part of the signaling pathways that, upon activation, lead to muscle relaxation. AZX100 is able to bypass the HSP20 signaling pathway, causing relaxation, particularly in myofibroblasts from wounds.97 In addition, AZX100 inhibits the production of connective-tissue growth factor (CTGF) by cultured fibroblasts exposed to TGF-beta1, resulting in excessive fibrosis.98 It has been demonstrated to be safe and well tolerated in phase I studies. It has shown a significant pharmacological effect and a trend toward significant efficacy in the reduction of scars.98 Ongoing phase II studies are evaluating the therapeutic effect of postexcisional intradermal application of AZX100 on keloids.99,100
Surgical Care
Surgical treatments include cryotherapy, excision, laser therapy, and other light therapies.
Cryotherapy
Cryosurgical media (eg, liquid nitrogen) affects the microvasculature and causes cell damage via intracellular crystals, leading to tissue anoxia. Generally, 1, 2, or 3 freeze-thaw cycles lasting 10-30 seconds each are used for the desired effect. Treatment may need to be repeated every 20-30 days. Take care to administer liquid nitrogen in short application periods because of the possibility of reversible hypopigmentation. Cryotherapy can cause pain and permanent depigmentation in selected patients. As a single modality, cryosurgery led to total resolution with no recurrences in 51-74% of patients after 30 months of follow-up observation.
Excision
Apply basic soft tissue handling techniques at primary wound repair sites. Carefully plan the closure with minimal tension, paralleling the relaxed skin tension lines. Use buried sutures, when necessary, for a layered closure and to reduce tension. Whenever feasible, apply pressure dressings and garments during the immediate postoperative period to wounds in patients in whom hypertrophic scars and keloid formation occur.
Decreased recurrence rates have been reported with excision in combination with other postoperative modalities, such as radiotherapy, injected IFN, or corticosteroid therapy. Excisional surgery alone has been shown to yield a 45-100% recurrence rate and should very rarely be used as a solitary modality, although excision in combination with adjunct measures can be curative. Most studies in which excisional surgery was combined with injected steroids reported a recurrence rate of less than 50%.
The authors have studied the effects of topically applied imiquimod 5% cream (Aldara) on the postexcision recurrence rates of 13 keloids excised surgically from 12 patients.101,102 Starting the night of surgery, imiquimod 5% cream was applied for 8 weeks. Patients were examined at weeks 4, 8, 16, and 24 for local erythema, edema, erosions, pigment alteration, and/or recurrence of the keloid. Of the 11 keloids evaluated at 24 weeks, none (0%) recurred. The rate of hyperpigmentation was 63.6%. Two cases of mild irritation and superficial erosion cleared with temporary discontinuation of imiquimod. Both patients completed the 8 weeks of topical therapy and the final 24-week assessment. At 24 weeks, the recurrence rate of excised keloids treated with postoperative imiquimod 5% cream was lower than recurrence rates previously reported in the literature.
Laser Therapy
Carbon dioxide, argon laser, and Nd:YAG laser (1064 nm)
Ablation of keloids and hypertrophic scars using a carbon dioxide laser (10,600 nm) can cut and cauterize the lesion, creating a dry surgical environment with minimal tissue trauma. When used as a single modality, the carbon dioxide laser was associated with recurrence rates of 39-92%, and when the carbon dioxide laser was combined with postoperative injected steroids, it was associated with recurrence rates of 25-74%.
Similarly to the carbon dioxide laser, the argon 488-nm laser can induce collagen shrinkage via generation of excessive localized heat. The argon laser has demonstrated recurrence rates of 45-93%.
The Nd:YAG laser (1064 nm) has demonstrated recurrence rates of 53-100%.
Pulsed-dye laser (585 nm)
The 585-nm PDL provides photothermolysis, resulting in microvascular thrombosis. Beginning in the 1980s, authors noted that scars became less erythematous, more pliable, and less hypertrophic after treatment with the 585-nm PDL. The findings were later confirmed using objective measurements of erythema by reflectance spectrometry readings, scar height, and pliability measurements. Because of its efficacy, safety, and relatively low cost, the PDL remains the laser treatment of choice for hypertrophic scars. Multiple publications have continued to confirm the role of the 585-nm PDL for the treatment of keloids and hypertrophic scars.
In a randomized clinical trial, Manuskiatti et al treated 10 keloidal or hypertrophic median sternotomy scars with a 585-nm flashlamp-pumped PDL at fluences of 3, 5, and 7 J/cm2, and one segment was left untreated as a control.13 They showed consistently better results in the treatment groups over the control. A trend was obtained towards lower fluences having more rapid onset of benefits and enhanced resolution of erythema, induration, and elevation of the scar. Multiple treatment sessions achieved greater clinical improvement.
Alster treated 44 bilateral, symmetric hypertrophic breast-reduction scars with a 585-nm PDL at 4.5-5.5 J/cm2 alone or in combination with intralesional TAC at 10-20 mg/mL injected immediately after the PDL irradiation.103 All scars showed clinical improvement. The average pliability scores decreased by 50% after 2 sessions in both groups. The concomitant use of TAC reduced symptom scores by 70% compared with PDL alone (50%).
In a prospective, randomized clinical trial, Nouri et al treated 11 patients with 12 postoperative scars with 585-nm PDL at 3.5 J/cm2 versus no treatment.104 The average overall improvement scores after one treatment was superior to the control (P = .0002). Vascularity improved 54% in treated halves, compared with 8% in controls. (P = .002). A total of 38% of halves returned to normal vascularity, compared with 0% in controls. Pliability improved 64% versus 1%, respectively (P = .002). A total of 62% of halves returned to normal pliability compared with 0% in control halves. The cosmetic appearance score was significantly better for the treated halves than for the untreated controls (7.3 vs 5.2; P = .016).
In contrast, Wittenberg et al found in a prospective, single-blinded, randomized, controlled study an overall reduction in blood flow (P = .001), volume (P = .02), and pruritus (P = .005) over time after a follow-up period of 4 months after treatment discontinuation, but no differences were noted among treatment and control groups treating hypertrophic scars with a 585-nm flashlamp-pumped PDL at 6.5-8 J/cm2 or silicone gel sheeting, or no treatment.105
4


