|
Carcinoma erysipelatoides= كارسينوما حمرانية |
 |
 |
 |
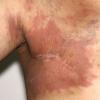 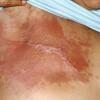   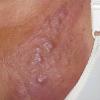 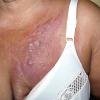 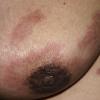 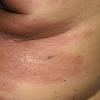 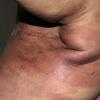 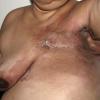 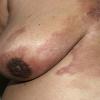 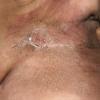 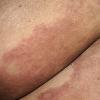 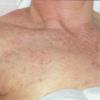 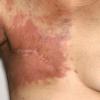
Carcinoma erysipeloides
Carcinoma erysipeloides (CE), which clinically resembles erysipelas, is an uncommon, but distinctive form of cutaneous metastasis. It has been termed inflammatory metastatic carcinoma. It classically presents as a rapidly evolving unilateral chest wall erythema, which may extend to the back, proximal part of the arm and even across the midline
|
Cancer metastasis represents the most devastating aspect of malignancy since mortality of tumor patients is mainly related to the metastatic behavior of the primary neoplasm. Excluding melanoma, the most common tumor to metastasize to the skin is breast cancer. Materials and Methods. We examined retrospectively the clinical, histopathologic and immunohistochemical features of 164 cases of skin metastases from breast carcinoma.
Results. Clinical features included papules and/or nodules in 131 patients (80%), telangiectatic carcinoma in 19 (11.2%), erysipeloid carcinoma in 5 (3%), "en cuirasse" carcinoma in 5 (3%), alopecia neoplastica in 3 (2%) and a zosteriform pattern in 1 patient (0.8%). Sites of cutaneous metastases were the trunk (145), head and neck (14) and extremities (5). Histopathologic features of adenocarcinoma with varying degrees of cell differentiation were observed although distinctive findings were associated with each clinical pattern. Immunohistochemical studies showed a positive staining with anti-cytokeratin and anti-EMA antibodies whereas reactivity with anti-CEA was detected in 110 of 164 cases (67%).
Conclusion. In conclusions, cutaneous metastatic breast carcinoma is characterized in most cases by suggestive clinical and histopathologic features and is usually associated with late stages of the disease.
|
|
|
|
Introduction
Cancer metastasis represents the most devastating aspect of malignancy since mortality of tumor patients is mainly related to the metastatic behavior of the primary neoplasm. The process of metastasis development involves a cascade of sequential steps, each of which has to be successfully completed in order to proceed to tumor progression. Malignant cells dissociate from the primary tumor, invade the surrounding extracellular matrix, attach to host cellular and extracellular determinants and promote enzymatic degradation of barriers, such as the basement membrane, to permit extravasation into the blood or lymphatic system. Furthermore, locomotion within the vessels followed by attachment to the target organs is an essential step in the development of metastasis. Nevertheless, tumor cells that eventually give rise to metastasis must evade des truction by host defenses, including specific and nonspecific immune responses (1-3).
Cutaneous metastases from visceral malignancies are relatively rare. The overall incidence is estimated to range from 0.7%-10.4% (4, 5). This discrepancy is likely due to the characteristics of the selected patients in each study, the types of tumor included in the statistics and the time of clinicopathological evaluation. In addition, the frequency of cutaneous metastases varies according to the incidence of the primary tumor. Excluding melanoma, the most common tumor to metastasize to the skin is breast cancer with an incidence of 23.9% and this correlates well with the frequency of occurrence of the primary tumor itself in women.
In this study, we examined retrospectively the clinical, histopathologic and immunohistochemical features of cutaneous metastatic breast carcinoma.
Materials and methods
A series of 164 cases of skin metastases from breast carcinoma observed at the Departments of Dermatology of the Universities of L´Aquila, Italy, and Graz, Austria, were reviewed. Cutaneous metastases from breast carcinoma were defined as direct extension from the primary tumor or as non-continuing spread of tumor cells through lymphatic or blood vessels. All patients were women aged 37-87 y (mean age: 62 y). In each case, tissue sections were stained with hematoxylin and eosin for histopathologic examination. Immunohistochemical studies were performed on paraffin sections using a three-step immunoperoxidase technique with PKK-1, AE-1/AE-3, LU-5, CK, EMA and CEA monoclonal antibodies.
Results
Clinical features
Metastatic cutaneous lesions were located at the site of mastectomy in 50 patients and elsewhere on the anterior aspect of the chest in 75, axilla (8), back (8), scalp (5), periauricular area (5), supraclavicular area (4), face (2), neck (2), upper (3) and lower (2) extremities. In all patients, appearance of cutaneous lesions followed the diagnosis of breast carcinoma (range: 2 months-8 years; mean: 4.1 years). Cutaneous lesions did not occur as a first sign of the disease in any of the patients examined. Clinical features included papules and/or nodules in 131 patients (80%), telangiectatic carcinoma in 19 (11.2%), erysipeloid carcinoma in 5 (3%), "en cuirasse" carcinoma in 5 (3%), alopecia neoplastica in 3 (2%) and a zosterifom pattern in 1 (0.8%). Nodular carcinoma, which was the most frequent clinical presentation, appeared as cutaneous or subcutaneous, solitary or multiple, pink to reddish, firm, rarely ulcerated nodules. Lesions were mainly located over the chest wall although face, neck, upper and lower extremities were involved too (Fig. 1). Telangiectatic metastatic breast carcinoma was characterized by purpuric papules, nodules or plaques on the trunk usually located in continuity with the surgical scar (Fig. 2). Erysipeloides or inflammatory metastatic carcinoma presented as an erythematous, warm, tender patch or plaque with a raised well-defined margin affecting the breast and the surrounding skin. "En cuirasse" metastatic carcinoma appeared as an infiltrated and extensive plaque in the mammary region (Fig. 3). Metastatic lesions of the scalp were observed in 3 patients as asymptomatic, red to pink, well-demarcated nodules or plaques resulting in circumscribed areas of hair loss, also referred as alopecia neoplastica. A zosteriform distribution of papulovesicles over the right breast occurred in 1 patient. |
Histopathologic and immunohistochemical findings
In all skin biopsy specimens, histopathologic features of adenocarcinoma with varying degrees of cell differentiation were observed. The most frequent histopathologic findings were single or multiple nodules located in the dermis and subcutaneous tissue, com posed of small to large aggregates of tumor cells surrounded by fibrosis. Neoplastic cells were typically arranged in gland-like structures (Fig. 4) or in a linear distribution between collagen bundles in an "indian file" pattern. Telangiectatic carcinoma was characterized by aggregates of tumor cells and erythrocytes as well as dilated blood vessels in the papillary dermis. In erysipeloid carcinoma, histopathologic features were metastatic cells tightly packed within dilated superficial and deep lymphatic vessels and a slight perivascular infiltrate of lymphocytes and plasma cells. In carcinoma "en cuirasse", fibrosis with few neoplastic cells sometimes exhibiting a characteristic "indian file" pattern was detected. Histopathologic findings of nodular carcinoma or "en cuirasse" carcinoma associated with atrophy of the hair follicle as a result of fibrosis were observed in metastatic lesions of the scalp. Finally, an epidermotropic pattern characterized by neoplastic cells, single or in small nests, within the epidermis and dermal aggregates of neoplastic cells in a sclerotic stroma was identified in 7/164 patients (4%).
Immunohistochemical investigations showed in all patients a strong positivity of tumor cells for pan-cytokeratins (PKK1, AE1/AE3, LU5, CK) and epithelial membrane antigen (EMA) (Fig. 5). In addition, a positive reaction for carcinoembryonic antigen (CEA) was detected in 110/164 of the cases (67%).
Discussion
Cutaneous involvement from breast carcinoma preferentially occurs in the skin overlying or proximal to the area of the primary tumor by direct extension or through lymphatic vessels. Nodular carcinoma, inflammatory or erysipeloides carcinoma, telangiectatic and "en cuirasse" carcinoma are the typical clinical manifestations of the lymphatic dissemination to the skin. Inflammatory carcinoma occurs when neoplastic cells disseminate through the lymphatics of the entire thickness of the dermis and subcutaneous tissue. In contrast, telangiectatic carcinoma is characterized by dissemination through superficial lymphatics and blood vessels of the dermis. In nodular carcinoma and "en cuirasse" carcinoma, the tumor cells disseminate largely along tissue spaces and only to a minor degree through lymphatic vessels (6). Although the above mentioned clinical manifestations are highly suggestive of cutaneous metastatic breast carcinoma, they may mimic a variety of benign and malignant cutaneous disorders as well as occur with cancers of other organs. Inflammatory skin metastases may clinically resemble erysipelas but, in contrast to true infection, there is no fever, chills and leukocytosis, and bacterial cultures are negative (7-11). This clinical pattern may also develop with cancers from other sites such as pancreas, colon and rectum, lung, ovary, prostate and parotid gland. Telangiectatic lesions have also been reported in carcinoma of the uterine cervix and parotid gland, and "en cuirasse" metastatic carcinoma may rarely be seen in kidney, lung and gastrointestinal malignancies. Hematogenous spread of neoplastic cells is responsible for alopecia neoplastica, which may simulate alopecia areata, sebaceous cyst, scleroderma, morphea-like basal cell carcinoma and discoid lupus erythematosus
Unusual and nonspecific clinical appearances of cutaneous metastatic breast carcinoma have been described. A zosteriform eruption, as observed in one of our patients, has been rarely reported and most likely results from a perineural lymphatic metastatic dissemination (14,15). The dermatomal distribution of vesicular lesions may clinically resemble herpes zoster. However, the site of cutaneous lesions, the presence of malignant cells within the vesicles and a negative viral PCR or culture allow to establish the definite diagnosis of cutaneous metastasis. Metastatic breast carcinoma presenting as a reddish nodule on the tip of the nose has been described and defined "clown nose" for its peculiar clinical feature (16). In addition, breast cancer of the inframammary crease may appear, mainly in women with pendulous breast, as cutaneous exophytic nodules clinically suggestive of a primary cutaneous squamous or basal cell carcinoma (17). Finally, metastatic breast cancer in the eyelid has been reported as a painless swelling of the eyelid associated with induration or nodule formation. Histologically, it may show characteristics of ductal or pleomorphic carcinoma as well as a histioid appearance (18).
Immunohistochemical studies may be helpful to identify the site of the primary tumor. In our series and previous reports, cutaneous metastatic breast carcinoma stained positively with antibodies to keratin proteins, as well as with anti-CEA and anti-EMA antibodies (6,19). In addition to estrogen and progesterone receptors, the gross cystic disease fluid protein-15 (GCDFP-15), a monoclonal glycoprotein expressed in apocrine epithelial cells and metaplastic apocrine tissue, has been described as a useful diagnostic marker for identifying primary as well as metastatic breast carcinoma (20-22). Recently, Bayer-Garners and Smoller suggested that androgen receptors might serve as additional immunohistochemical markers to increase sensitivity for detecting breast cancer in skin metastasis (23).
The prognosis of patients with cutaneous metastasis depends on the type and biological behavior of the underlying primary tumor and on its response to treatment. Skin metastases from breast carcinoma are usually associated with advanced stages of the disease as observed in our study and, therefore, in most cases, they represent a poor prognostic sign.
Systemic chemotherapy is the most commonly used treatment whereas the specific protocol depends on the histopathologic type of the primary tumor and staging of the patient. Surgical excision, radiotherapy, intralesional chemotherapy or immunotherapy can be used when solitary lesions develop or in the late stages of the disease in order to improve the quality of life of the patient.
|
|
|
|


