










TICKS
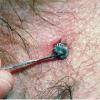
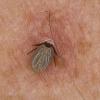
Ticks are divided into two families: Ixodidae (hard ticks) and Argasidae (soft ticks). Hard ticks are responsible for the majority of tick-related disease. Ticks pass through multiple stages during their life cycle, including egg, larva, nymph, and adult, and require blood meals for transition between the latter three stages. Ticks are distinguished from other mites by the presence of a barbed hypostome, which is inserted into the skin for feeding . Ticks ingest blood from a diversity of vertebrate hosts including birds, reptiles, and mammals. Adult hard ticks are capable of ingesting several hundred times their unfed body weight when taking a blood meal and may survive for months without feeding. When searching for a suitable host, hard ticks exhibit a unique behavior called “questing” during which the tick crawls to the edge of a leaf or blade of grass and holds its front pair of legs stretched out in order to grab onto a passing host. Humans often become infested by contact with tall grass or brush that harbors the unfed ticks or by their association with domestic animals like cats or dogs. Ticks are attracted to the smell of sweat, the color white, and body heat. Once on a host, a tick may spend up to 24
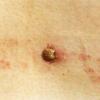
hours in search of a protected site to feed, such as a skin fold or the hairline. Tick feeding time ranges from 2 hours to 7 days, with the tick dropping off of the host once fully engorged.
Many different tick species are responsible for local tick bite reactions and transmission of disease in human hosts. In the United States, Ixodes scapularis (deer tick or black-legged tick), Dermacentor andersoni (American wood tick), D. variabilis (American dog tick), I. pacificus (Western black-legged tick), and Amblyomma americanum (Lone Star tick) are among the most common. In the Eastern Hemisphere, important tick species include I. ricinus (castor bean tick or sheep tick) and I. persulcatus (Taiga tick). Among the diseases transmitted by ticks are Lyme disease , ehrlichiosis, babesiosis, Rocky Mountain spotted fever , Colorado tick fever, Q fever, and tularemia .
Clinical Findings.
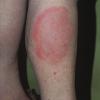
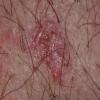
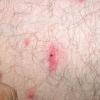
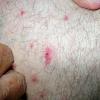
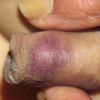
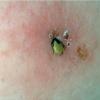
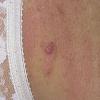
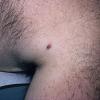
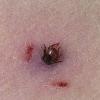
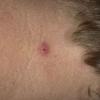
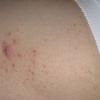
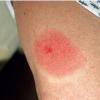
The majority of tick bites occur in the spring and summer, coinciding with the life cycle of the tick. Tick bites are usually painless, as the tick introduces an anesthetic and anticoagulant substance when biting. Often, a person will not even know he or she has been bitten but will see or feel an attached tick while scratching or bathing. Tick bites may incite foreign body granuloma formation, reactions to injected toxins and salivary secretions, and hypersensitivity responses. Rarely, delayed hypersensitivity reactions occur with fever, pruritus, and urticaria. A red papule is usually seen at the bite site, and may progress to localized swelling and erythema. A cellular response to the bite can lead to induration and nodularity after a few days. Foreign-body reactions may occur when mouth parts are retained in skin after incomplete removal of the tick. Chronic tick bite granulomas may present diagnostic problems and persist for months to years.
Tick paralysis is a potentially lethal complication of tick infestation and is thought to be caused by a neurotoxin contained within tick salivary secretions. The illness may start with headache and malaise and rapidly progress to an acute ascending lower motor neuron paralysis, similar to that of Guillain-Barré syndrome, which may result in respiratory failure and death.43,44 Several species of tick are capable of causing tick paralysis, including D. andersoni, D. variabilis, and A. americanum. Typically, the onset of symptoms occurs 4 to 6 days after attachment of the tick. Symptoms resolve once the tick is removed from the patient. Supportive measures, including mechanical ventilation, may be required until symptoms resolve.
Management.
After potential exposure, the skin should be inspected for ticks to remove them before they begin feeding and risk transmitting disease. Once a tick has inserted its hypostome into the skin, it must be forcibly removed. Although many methods have been suggested for removing ticks, physical methods, such as slow, steady pulling on the tick, are probably the safest and most useful. Retained tick parts should be removed surgically if necessary to prevent development of foreign body granulomas. Antibiotic prophylaxis after tick bites is controversial. Although there is some evidence that prophylaxis may help prevent acquisition of Lyme disease and other vector-borne illnesses, the risks of antibiotic therapy must be weighed against the risks and prevalence of vector-borne illnesses in a particular region. In areas highly endemic for Lyme disease, the benefits of prophylactic treatment may outweigh the risks, especially in cases in which the tick has been attached to the host for an extended period of time and can accurately be identified as a vector for Lyme borreliosis. In these cases, the authors suggest a course of oral doxycycline .
▪ CHILOPODA AND DIPLOPODA
The arthropod classes Chilopoda and Dipoploda are composed of centipedes and millipedes, respectively. Centipedes and millipedes are terrestrial arthropods with multiple body segments.
Centipedes
Centipedes, which have one pair of legs per body segment, are nocturnal carnivores that may produce extremely painful bites with a pair of poisonous claws. The Scolopendra species is found throughout the southwestern U.S. and may attack when its habitat is disturbed. In addition to severe pain and erythema following a bite, localized sweating, edema, secondary infection, and ulceration may be seen. There are also case reports of proteinuria, acute coronary ischemia, and myocardial infarction following centipede bite. Treatment consists of analgesia, including injection of local anesthetics, antihistamines, and tetanus prophylaxis. Antibiotics may be required to treat secondary infection.
Millipedes
Millipedes, which have two pairs of legs per body segment, usually feed on living and dead plant matter. They lack poison claws and neither bite nor sting. However, millipedes possess repugnatorial glands on either side of each segment and may emit a toxic substance if threatened. The oily, viscous liquid can cause a brownish discoloration of the skin that can persist for months and may produce burning and blistering. Severe reactions are mainly seen in tropical species. Some species are capable of squirting the toxin several inches. This can result in various eye lesions including periorbital edema, periorbital discoloration, conjunctivitis, and keratitis. Although ophthalmologic evaluation should be considered for eye exposures, thorough immediate cleansing with soap and water is usually adequate for skin contact.