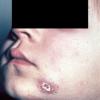
Tuberculous Primary
Complex)
Tuberculous chancre and affected regional lymph nodes constitute the tuberculous primary complex in the skin. The condition is believed rare, but its incidence may be underestimated. In some regions with a high prevalence of tuberculosis and poor living conditions, primary inoculation tuberculosis of the skin is not unusual. Children are most often affected. Sites of predilection are the face, including the conjunctivae and oral cavity, as well as the hands and lower extremities.
PATHOGENESIS
Tubercle bacilli are introduced into the tissue at the site of minor wounds. Oral lesions may be caused by bovine bacilli in nonpasteurized milk and occur after mucosal trauma or tooth extraction. Primary inoculation tuberculosis is initially multibacillary but becomes paucibacillary as immunity develops.
CLINICAL MANIFESTATIONS
The chancre initially appears 2 to 4 weeks after inoculation and presents as a small papule, crust, or erosion with little tendency to heal. A painless ulcer develops, which may be quite insignificant or may enlarge to a diameter of more than 5 cm . It is shallow with a granular or hemorrhagic base studded with miliary abscesses or covered by necrotic tissue. The ragged edges are undermined and of a reddish blue hue. As the lesions grow older, they become more indurated, with thick adherent crusts.
Wounds inoculated with tubercle bacilli may heal temporarily but break down later, giving rise to granulating ulcers. Mucosal infections result in painless ulcers or fungating granulomas. Inoculation tuberculosis of the finger may present as a painless paronychia. Inoculation of puncture wounds may result in subcutaneous abscesses.
Slowly progressive, regional lymphadenopathy develops 3 to 8 weeks after the infection (see Fig. 184-1) and may rarely be the only clinical finding. After weeks or months, cold abscesses may develop that perforate to the surface of the skin and form sinuses. The lymph nodes draining the primary glands may also be involved. Body temperature may be slightly elevated. The disease may take a more acute course, and in half the patients, fever, pain, and swelling simulate a pyogenic infection.
HISTOPATHOLOGY
Early, there is an acute non-specific inflammatory reaction in both skin and lymph nodes, and mycobacteria are easily detected by Fite stain. After 3 to 6 weeks, the infiltrate and the regional lymph nodes acquire a tuberculoid appearance and caseation may occur.
Differential Diagnosis of Primary Inoculation Tuberculosis
· Syphilis
· Tularemia
· Bartonellosis
· Sporotrichosis
· Other mycobacterioses
DIAGNOSIS
Any ulcer with little or no tendency to heal and unilateral regional lymphadenopathy in a child should arouse suspicion. Acid-fast organisms are found in the primary ulcer and draining nodes in the initial stages of the disease. The diagnosis is confirmed by bacterial culture. The PPD reaction is negative initially and later converts to positive .
The differential diagnosis encompasses all disease with a primary complex .
COURSE
Untreated, the condition may last up to 12 months. Rarely, LV develops at the site of a healed tuberculous chancre. The regional lymph nodes usually calcify.
The primary tuberculous complex usually produces immunity, but reactivation of the disease may occur. Hematogenous spread may give rise to tuberculosis of other organs, particularly of the bones and joints. It may also lead to acute miliary disease with a fatal outcome. Erythema nodosum occurs in approximately 10 percent of cases