Lymphocytoma Cutis
Lymphocytoma cutis is not a specific disease. Rather, it is a response to a variety of known and unknown stimuli that results in the accumulation of lymphocytes and other inflammatory cells in a localized region. Lymphocytoma cutis is known to simulate lymphoma, as reflected primarily by the histologic findings. However, it is a reactive process and generally has a benign course. When known, the inciting agent should be included in the diagnosis. The term lymphocytoma cutis or pseudolymphoma without modification should be reserved for idiopathic cases.
Related articles include Cutaneous B-Cell Lymphoma and Cutaneous T-Cell Lymphoma. Additionally, the Medscape Skin Cancer Resource Center may be of interest.
In lymphocytoma cutis, lymphocytes and other inflammatory cells are recruited to a localized area of the skin in response to known or unknown stimuli. Most cases are idiopathic. Lymphocytoma cutis is not considered a lymphocytic response to malignancy.
Cases with known etiologies involve a reaction to tattoo dye, jewelry (especially gold), arthropod bites, medications, folliculitis, trauma, infections (ie, with Borrelia burgdorferi, molluscum contagiosum), vaccinations, and acupuncture.
A discrete subset of lymphocytoma cutis, borrelial lymphocytoma, occurs primarily in Europe, in areas in which the Ixodes ricinus tick is endemic. This form of the disease is a response to an infection due to Borrelia burgdorferi subsp afzelius that is transmitted by a tick bite.
.Lymphocytoma cutis is not associated with mortality. It is rarely associated with morbidity other than minor pain or pruritus. It generally heals without scarring.
No racial predilection is noted.
The female-to-male ratio in reported cases is approximately 2:1.
Individuals of any age may be affected, but lymphocytoma cutis is most common in early adulthood.
- The mean patient age at onset is 34 years. Approximately 8% of cases involve patients younger than 18 years.
- Two thirds of patients are younger than 40 years at the time of biopsy.
- Borrelial lymphocytoma is more common in children than adults and is most often observed in Europe.
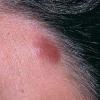
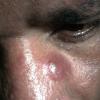
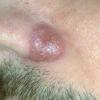
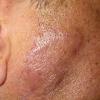
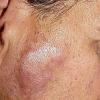
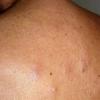
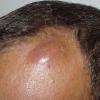
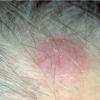
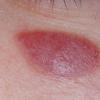
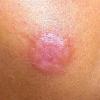
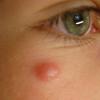
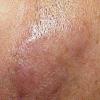
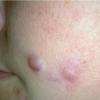
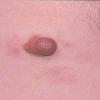
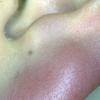
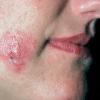
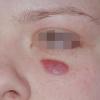
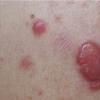
- Patients present with a nodule or group of discrete nodules, usually with minimal associated symptoms.
- Occasionally, pruritus or pain is noted.
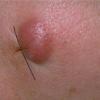
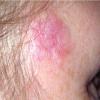
- Examination usually reveals a single nodule with a diameter of one to several centimeters.
- Although the lesions may be soft, they are more often firm.
- Typically, the lesions are red to purple but can be absent of color as well.
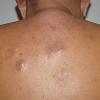
- Approximately three quarters of the cases involve localized lesions.
- The remaining cases usually involve grouped papules in a single defined region.
- More disseminated cases are rare.
- The most common site of involvement is the face (70%).
- Next most common sites are the chest and upper extremities.
- Lesions below the waist are uncommon.
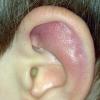
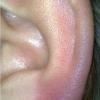
- Sites of predilection for Borrelial lymphocytoma are sites with low skin temperature, including the following:
- Earlobes
- Nipples and areolae
- Nose
- Scrotum
Most cases are idiopathic. Known inciting agents include the following:
- Tattoo dye
- Jewelry (eg, gold earrings)
- Arthropod (insect and spider) bites
- Medications2
- Folliculitis
- Trauma
- Vaccinations
- Materials that come into direct contact with the skin or are injected into the skin (eg, gold, aluminum)
- Infection (eg, varicella-zoster virus, Borrelia species, molluscum contagiosum, Helicobacter pylori)
- Sites where acupuncture needles were inserted
Treatment
- When the offending agent is known, its removal results in disease resolution.
- Cases that occur as a result of infection should be treated appropriately.
- In idiopathic cases, treatment is not mandatory.
- In severe cases, local radiation therapy can be effective.
- Some report a response to topical or injected corticosteroids as well as topical immunomodulators such as tacrolimus.
- Patients with presumed lymphocytoma cutis in whom lymphoma cannot be excluded should be examined for the possibility of concurrent extracutaneous disease. Careful follow-up is required to evaluate the possible emergence of lymphoma.
Surgical removal or cryosurgery may be effective in some cases.