

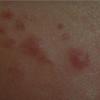
Leiomyoma
EPIDEMIOLOGY
The exact incidence of leiomyomas is unknown. In one study, the 10-year incidence was 0.04 percent with the majority of lesions occurring in women. Although leiomyomas are thought to be relatively uncommon neoplasms, the actual incidence may be higher than previously believed due to failure to recognize and biopsy the lesion.
ETIOLOGY AND PATHOGENESIS
Cutaneous leiomyomas are divided into three subsets: (1) solitary or multiple piloleiomyomas originating from the arrector pili muscles; (2) genital leiomyomas originating from the mammillary, dartoic, or labial/vulvar muscles; and (3) angioleiomyomas, originating from vascular smooth muscle. Most leiomyomas are acquired; however, familial inheritance patterns have been described. Especially noteworthy are patients with multiple piloleiomyomas. Starting in early adulthood, these patients present with increasing numbers of tumors, developing as many as 100 to 1000 lesions. Transmission appears to be autosomal dominant with variable penetrance. Women with multiple piloleiomyomas may also develop uterine leiomyomas, an entity termed multiple cutaneous and uterine leiomyomatosis (also known as familial leiomyomatosis cutis et uteri or Reed syndrome). In addition, some families with multiple cutaneous and uterine leiomyomatosis have been shown to cluster renal cell cancer, and this has been termed hereditary leiomyomatosis and renal cell cancer. Recently, a loss of function mutation in the gene encoding fumarate hydratase on chromosome 1q42.3-43 has been shown to predispose individuals to these conditions. Fumarate hydratase catalyses the conversion of fumarate to malate in the Krebs cycle but is also considered to be to be a tumor suppressor gene.
LEIOMYOMA AT A GLANCE
· Benign cutaneous neoplasm derived from arrector pili muscle (piloleiomyoma), mammillary, dartoic or labial/vulvar muscle (genital leiomyoma), or the walls of blood vessels (angioleiomyoma).
· Present as solitary or multiple flesh-colored, occasionally painful papules; rarely associated with uterine leiomyomas and renal cell cancer.
· Treatment: Surgical; recurrence is common
CLINICAL FINDINGS
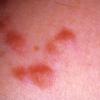
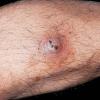
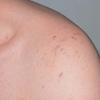
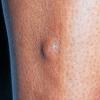
The most common presentation is that of multiple piloleiomyomas. Individual lesions range in size from several millimeters to 1 cm and are usually reddish-brown firm papulonodules that are fixed to the skin but freely moveable over underling deeper structures . They can coalesce to form plaques or linear, grouped, or dermatomal patterns. The extensor extremities, trunk, and sides of the face and neck are the most common locations. Patients with piloleiomyomas often have pain that may be spontaneous or secondary to cold, pressure, or emotion. Possible explanations for this phenomenon include pressure of the tumor on local nerve fibers and contraction of the smooth muscle fibers. Genital leiomyomas are clinically similar to piloleiomyomas except that they are usually asymptomatic. They commonly present as solitary, deep papulonodules or occasionally, pedunculated papules on the scrotum, vulva, penis, or areolar region. Angioleiomyomas present most commonly as solitary, painful subcutaneous nodules on the legs in women that can grow to several centimeters in diameter.
HISTOPATHOLOGY
Pilar leiomyomas are composed of a poorly circumscribed proliferation of haphazardly arranged, bland-appearing smooth muscle cells with characteristic eosinophilic cytoplasm, blunt-ended nuclei and perinuclear halos in cross-section. They are located in the dermis and can infiltrate the surrounding tissue with extension into the subcutis . Genital leiomyomas usually resemble pilar leiomyomas. Angioleiomyomas are well-circumscribed, richly vascularized dermal or subcutaneous nodules composed of well-differentiated smooth muscle fibers . Occasionally, the vessel of origin can be identified. Leiomyomas stain positive with smooth-muscle actin and desmin.
DIFFERENTIAL DIAGNOSIS
Differential diagnosis of leiomyoma includes any flesh-colored or reddish-brown superficial or deep-seated papule or nodule: angiolipoma, glomus tumor, eccrine spiradenoma, neurofibroma, nevus, or lipoma.
PROGNOSIS AND CLINICAL COURSE
Cutaneous leiomyomas do not regress spontaneously, and there does not appear to be risk of malignant degeneration into leiomyosarcoma. A minority of patients may also develop uterine leiomyomas and, in some families, association with renal cell carcinoma has been described. Occasionally, leiomyomas are associated with polycythemia. This may be due to erythropoietin-like activity of leiomyomas, which has been demonstrated in tumor extracts.
TREATMENT
Excision is the treatment of choice for leiomyomas that cause pain or cosmetic concern; however, recurrence is common. In patients with numerous lesions, this method is impractical. Carbon dioxide laser ablation was reported as an effective modality whereas cryotherapy and electrosurgery have been used with disappointing results. Pain may be a significant source of morbidity and, when surgical intervention is not possible, potential treatment options include nitroglycerin, phenoxybenzamine, nifedipine, gabapentin, or topical analgesics